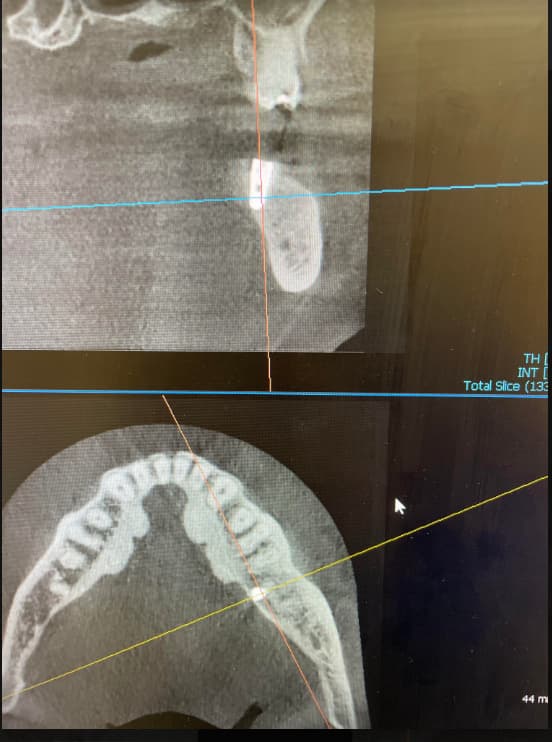
Early Dental Implant Failure: Clarification of Possible Explanations?
Dr. B. asks:
I have been confronted with a case of early implant failure resulting in the removal of the implant, I am trying to figure out what went wrong with a case that I just did which failed immediately.
My understanding is that there are two possible explanations here. First is the potential of “burning the bone”, i.e. I may have overheated the bone during the osteotomy phase creating heat-generated bone necrosis. Another possibility is that I contaminated the osteotomy site or the implant and caused an early infection. For each explanation, I would appreciate some clarification.
In regards to “burning the bone” are we talking about too low RPM’s, too long contact (time) of the drill against the bone, using room temperature water to irrigate instead of chilled water, a dull osteotomy drill, etc. External irrigation of the osteotomy bur does not really allow much irrigation into the osteotomy so do you pump the drill in and out with only seconds of contact?
With regards to contamination , what about flapless when the crestal tissue is lacking ? What about placing ophthalmic gentamycin on the implant itself prior to insertion? What do you think?
Thanks.