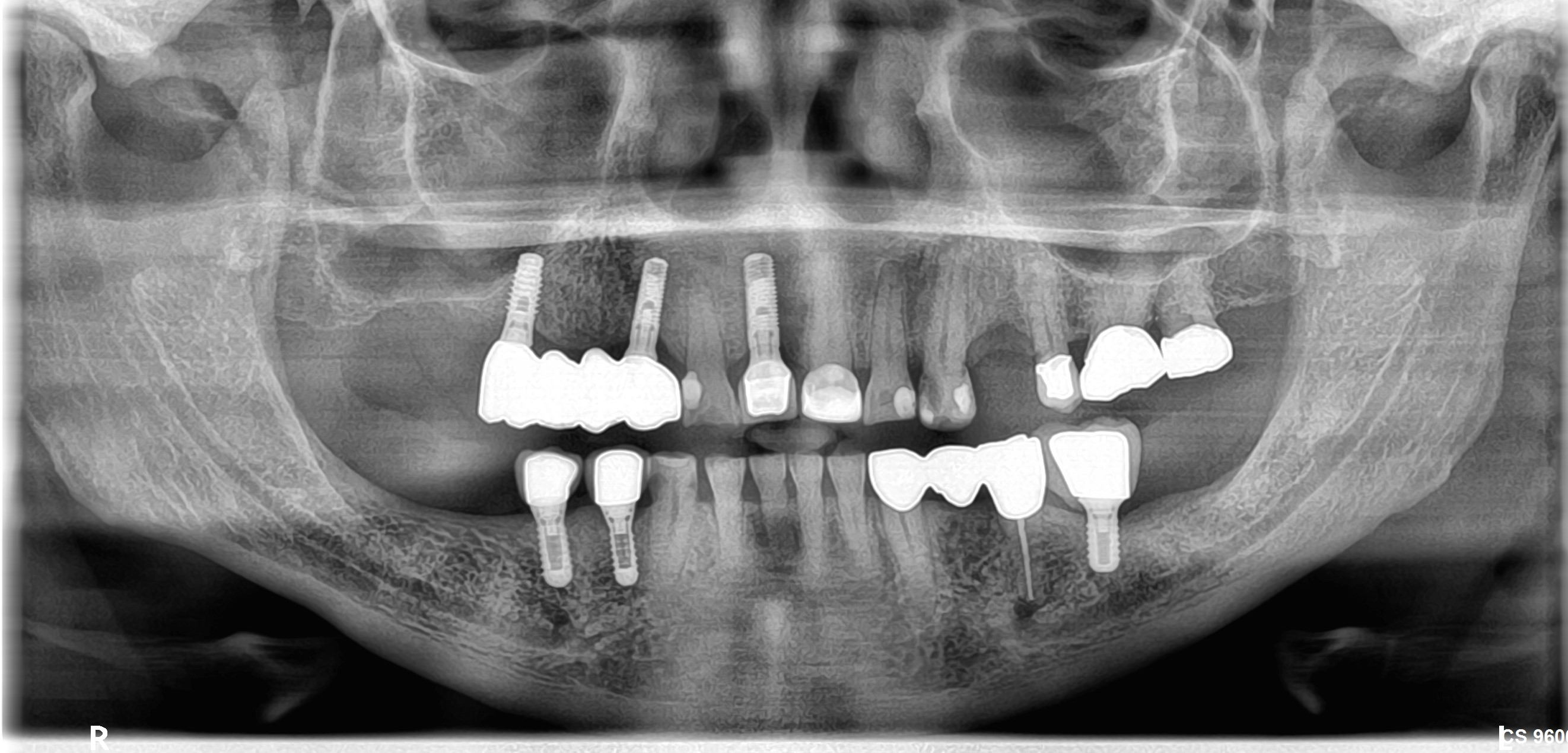
Both of the implants should be removed, as they are beyond any reasonable hope of salvage. To pretend otherwise is wishful thinking. There are many protocols for regenerating bone around infected implants, but they seem to be designed for implants that are within the form of the arch, that is, the threads don't protrude past the buccal or lingual outline of the ridge. So, a space making osseous defect. Dr. Stuart Froum just published a textbook about implant repair and Dr. Myron Nevins, along with some Japanese compadres, is presenting cases of bone regeneration around implants, using a laser, at the current AAP meeting in Los Angeles. Again, the common theme seems to be that the implants are within space making defects. From the description, one or both of the implants are beyond the confines of the ridge. The canine is hopelessly involved also. If this section of the dentition is any indication, the patient may have other problems, and deserves a thorough workup. As for severe pain, if the lingual threads are exposed, then the patient may have a large traumatic ulcer on the ventro-lateral surface of the tongue. Grasp the tongue with gauze and lift it up to see. These ulcers are quite painful, especially upon swallowing. The pain radiates to the ear and throat. You have to get rid of the cause, whether it be an osseous sequestrum, sharp edge on a tooth or restoration, or exposed implant threads.
Baker k. Vinci
9/28/2012
You don't think this doctor examined his patient? He took the time to post the case, certainly he examined the patients tongue and lingual aspect of the mandible . The natural tooth, is most likely salveagabe, unless you are one of those guys that uses his "hammer for every procedure". Keep the natural tooth please. No one likes to place implants more than myself, but nothing replaces a natural tooth better than a natural tooth . I'm tired of saying it ! Bvinci
DrT
9/28/2012
I appreciate your desire to save natural teeth Bv...however, it all comes down to diagnosis. In this instance, if you consider crown to root ratio post crown lengthening as well as the ferrule rule, not to mention what you will have to do to the bone on the adjacent teeth and implants, I would have to say that in this instance, retaining the canine is an unwise choice.
DrT
periodoc
9/28/2012
Unfavorable crown/length ratio; insufficient ferrule, remove it. I don't know whether the dentist examined the patient thoroughly. I merely suggested a possible source of the pain, if it please you.