Fixed Bridge or Implants?
Hello everyone,
First I want to say that I’ve learned a lot about complex cases here on OsseoNews than in any textbook or journal of implants, so here is one for everyone, where I am sitting on the fence. Your opinions and suggestions are welcome, as we need to get into replacement options sooner than later.
I have a 55-year old male patient in excellent health but a smoker with severe bruxism and clenching. In September 2010, He sustained a vertical fracture in #13 [maxillary left second premolar; 25] which I extracted atraumatically and placed Osteograf LD 150 for socket preservation. The fracture most likely was from his severe clenching habit, but patient will not admit to it.Â
Cut to January 2013. Now #12 [maxillary left first premolar; 24] has fractured resulting in dislodgement of the DO resin and another vertical fracture with necrotic pulp. The fracture may not go do far enough to render this tooth non-restorable. I want to extract #12 and place implants in #12 and 13 sites with single crowns. Sinus is low and I may have to do a sinus lift. Patient has some ideas about his treatment plan. First plan is to extract #12 and do a 4-unit bridge from #14 to 11 [maxillary left first molar to canine; 26-23]. Patient also wants me to try to save #12 first with a root canal. If this can be done successfully, he wants me to run a bridge from #14 to 12.Â
To summarize, all our options right now are:
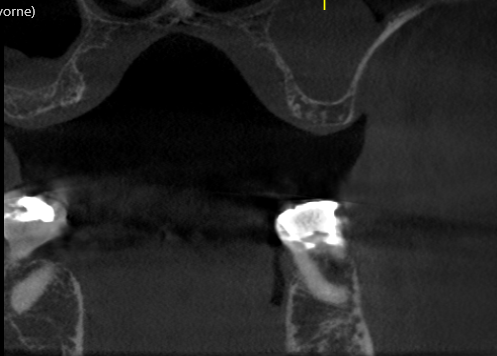
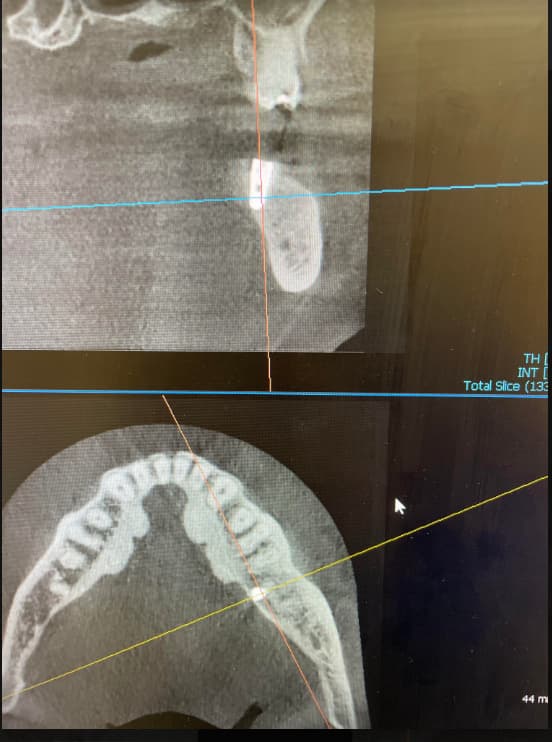
1) Extract #12 (24) and do two implants at the same sitting, then two joined crowns in 4 months time. Note that there is only about 8-9mm bone height in the #13 (25) area due to the sinus floor, and if an immediate is planned in 24 area, I could go with a 13mm here, but going beyond the socket apex is not possible, due to sinus floor.
2) Extract #12 (24), no grafting then wait 4-5 weeks, then place two implants in the #12 (24) and #13 (25) area. Delayed immediate placement.
3) Complete RCT on #12 (24), then using #12 (24) as mesial abutment, make a three unit fixed bridge to replace #13 (25) as well as hold #12 (24) together. Non-surgical option.
4) Complete #12 (24) RCT, crown it. Implant only in #13 (25) area with a single crown on it.
How do you think we should treat this case? Which of these treatment options do you think would have the greatest chance of success?
Case images (click any image to enlarge)
![Fractured 25 in Sep 2010. Tooth surgically removed in two halves, socket preservation done with HA particles [OSTEOGRAF LD-150 -Dentsply]](https://osseonews.nyc3.cdn.digitaloceanspaces.com/wp-content/uploads/2013/01/Fractured-25-in-2010.jpg) Fractured 25 in Sep 2010. Tooth surgically removed in two halves, socket preservation done with HA particles [OSTEOGRAF LD-150 -Dentsply]
Fractured 25 in Sep 2010. Tooth surgically removed in two halves, socket preservation done with HA particles [OSTEOGRAF LD-150 -Dentsply] Split down the root into two
Split down the root into two
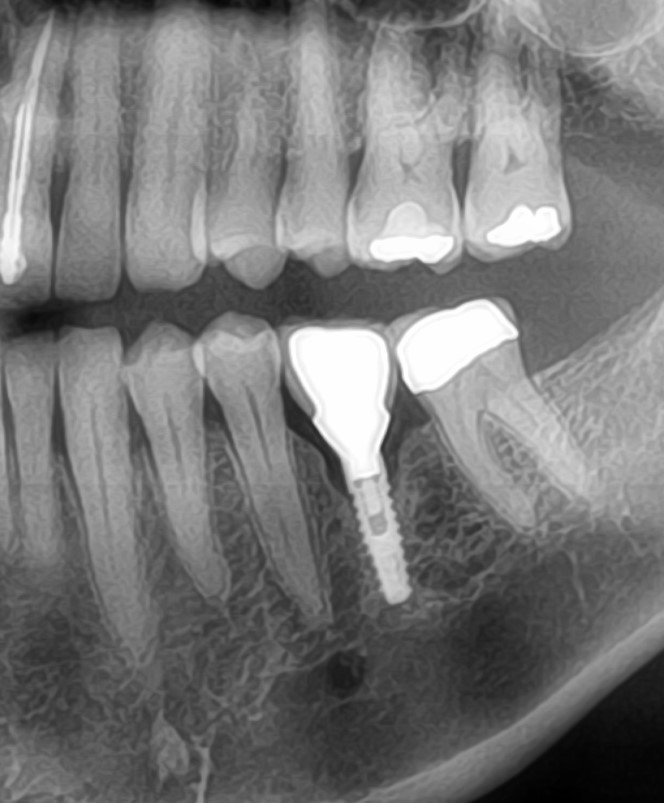
![In January 2013, Xray of pain over 24, and OD composite lost on distal.]https://osseonews.nyc3.cdn.digitaloceanspaces.com/wp-content/uploads/2013/01/Image000.jpg)In January 2013, Xray of pain over 24, and OD composite lost on distal. Image of 24 as remaining occlusal composite came away very easily, complete debond failure, rare with my composites.
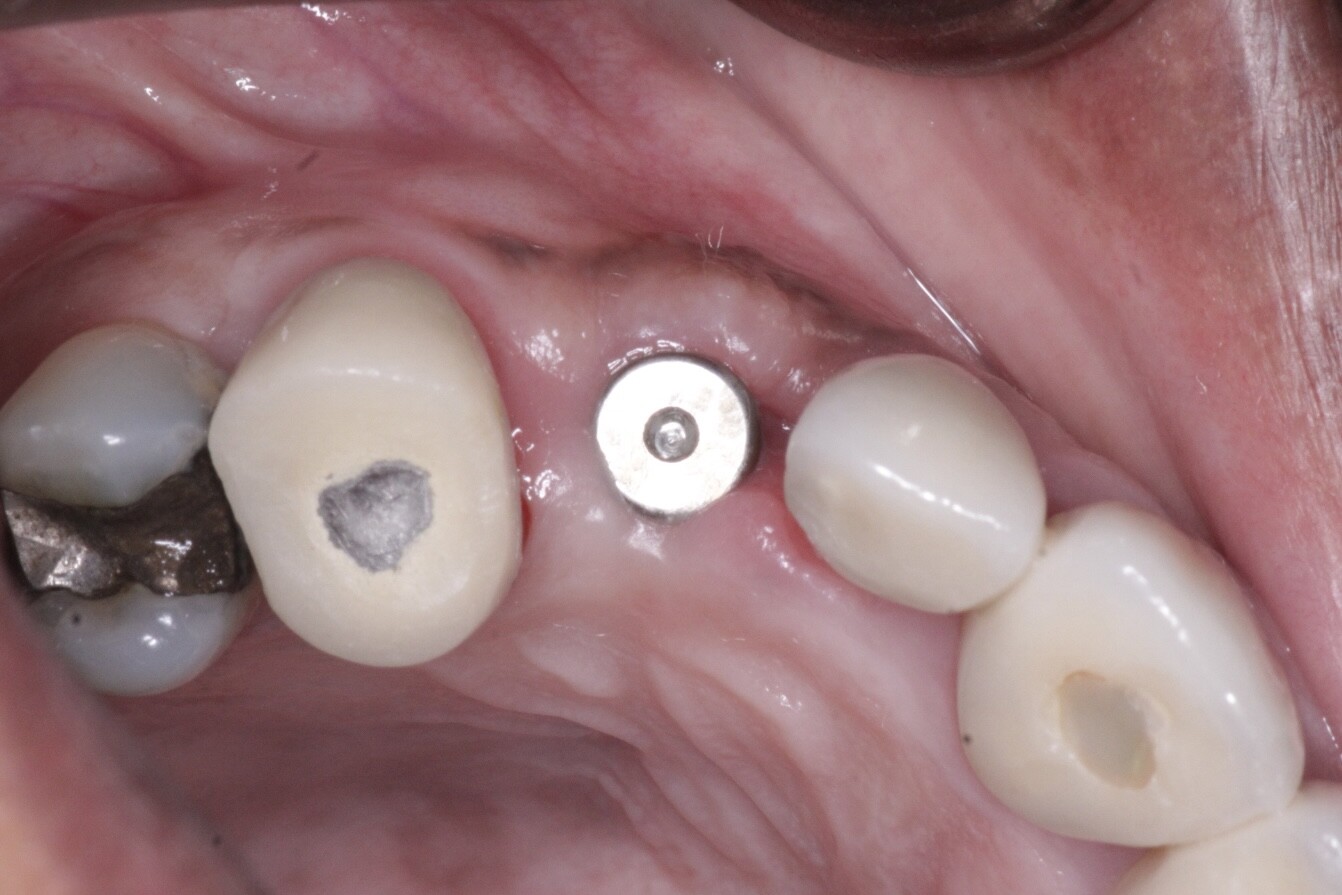
Image of 24 as remaining occlusal composite came away very easily, complete debond failure, rare with my composites. Close-up of Tooth#24, after pulpectomy and before placing CaOH dressing. To keep this tooth or not?
Close-up of Tooth#24, after pulpectomy and before placing CaOH dressing. To keep this tooth or not?