Pneumatized Maxillary Sinus: Correct Treatment Plan?
Dr. D. asks:
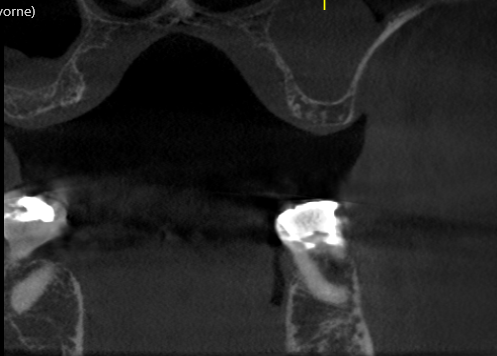
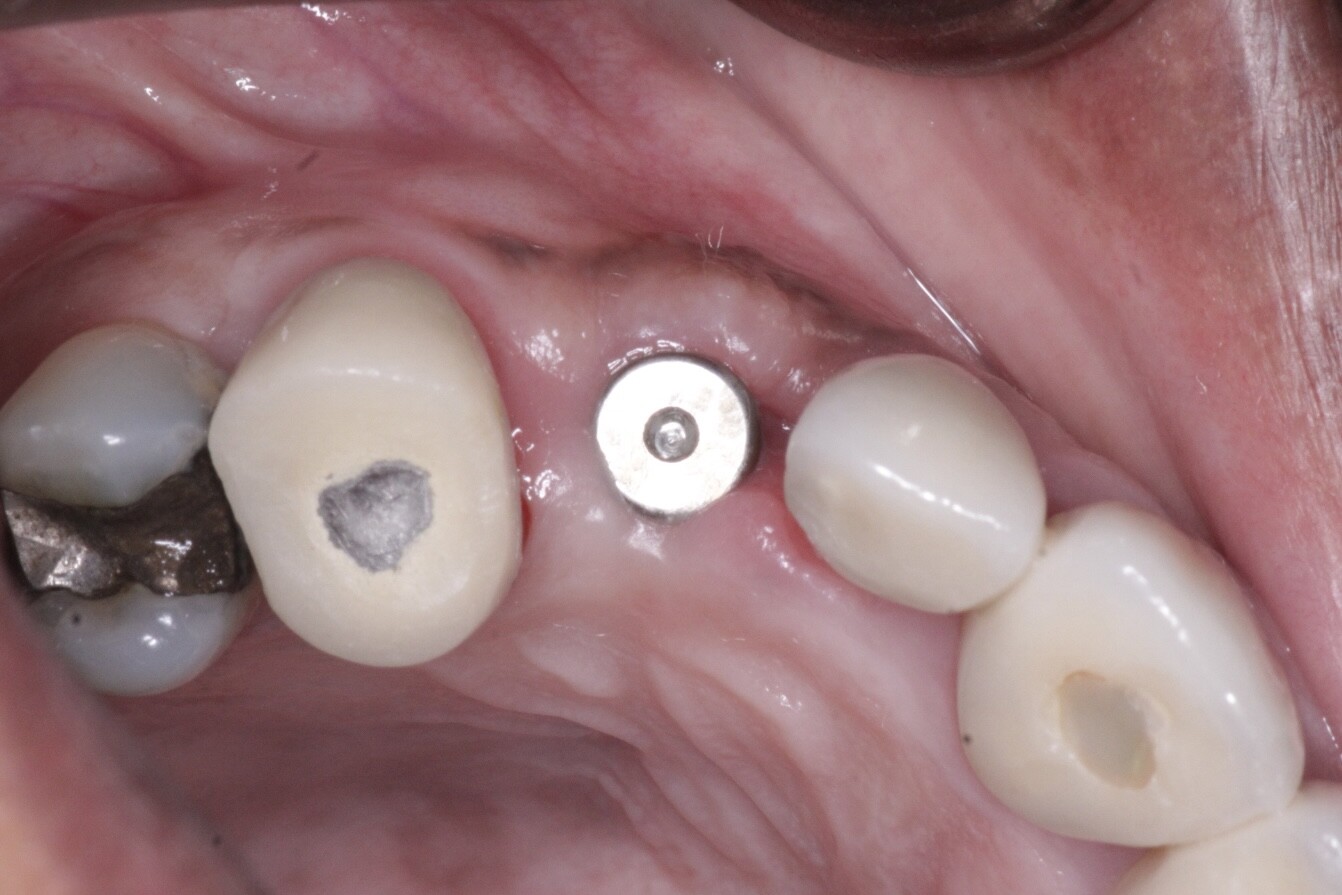
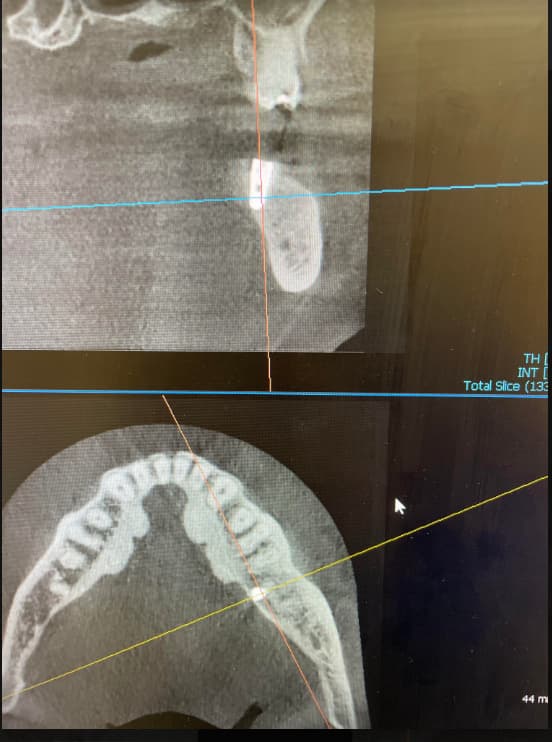
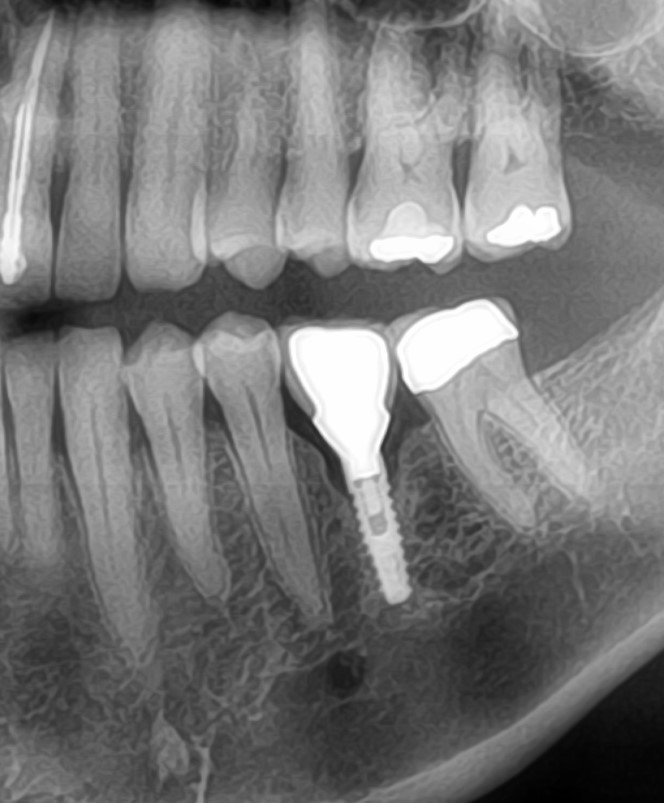
I have a somewhat pneumatized maxillary sinus in my patient. I am planning on doing sinus lifts bilaterally. My goal would be to have adequate sinus lift and bone graft for accommodating 8mm long dental implants. I would rather place 10mm long implants but given the conditions in my patient, I do not think that is going to be possible. I think in this case I would rather be cautious and only lift and graft enough for 8mm implants. My overall treatment plan is for six 4.3mm x 8mm implants to support a screw retained fixed partial denture. I plan on placing one implant in each molar, premolar and incisor areas. Do you think this is a sound treatment plan?
20 Comments on Pneumatized Maxillary Sinus: Correct Treatment Plan?
New comments are currently closed for this post.
DR.C
9/29/2008
if 8mm is possible, why not 10mm?
Neda-Moslemi
9/30/2008
Dear Dr. D.,
Obtaining pimary stability which is the most improtant criterion in implant success will be much more difficult with 8 mm implant in such case (poor quality and lack of natural bone). The shortest implant that I use in my cases in posterior maxilla in 10 mm. Bridging implants that are placed far from eachother is not justified, as well.
Good luck
Neda
Dr. J
9/30/2008
If you are doing 8mm why not 10mm or 13mm. If you're to afraid to lift more, don't be. I would also think about a couple of more implants (4 on either side Lateral/K9,premolars and molar) and not place in the central incisor region. In case one fails, your prosthesis is safe. You may have phonetic issues down the road. Charge the patient a fix fee (case fee) and not per implant etc. what is few hundred dollars.
Dr.F
9/30/2008
If you are doing the sinus lift, what condition precludes the patient from having 10-13 mm implants. Also, a sinus lift bone quality of D4 may not be enough for supporting the fixed prosthesis. The bone in the posterior maxilla is going to be soft and you should either increase the implant length, implant diameter or better by increasing the number of implants to be safe and prevent any bone overloading. I would go with 7-8 implants in such a situation. If the patient can't afford the extra implant, put it in for free. The patient will appreciate it and if for any reason one implant fails in the 6-implant scenario, you'll be redoing the whole case for free. Save yourself some aggravation and money and make the patient happy by explaining to them why you feel the extra implant(s) may be required and you'll do it at no cost.
Bruce G Knecht
9/30/2008
If you have 8mm of bone height and width to accomidate 4.3 implants, Place the 13mm length. Use a osteotome lift and raise the sinus with particulate bone. I like conical implants when I raise sinuses and place impalnts due to the swedging of the body making it impossible for the implant to fall into the sinus. I love to see 8mm of bone. Most people breath better after you tap their sinuses. As long as there is no sinus infection at the time. Remember a fearful dentist will hurt the patient more than a confident one. Hope this helps!
ziv mazor
9/30/2008
Dear Dr D.
Experience,experience,experience....It seems you need more confidence and experience in doing the sinus lift procedure.There is no justification for placing 8mm implants after sinus lift.To my opinion 13mm long implants are the standard implants in these procedures.In order to gain primary implant stability undersize the osteotomies and use tapered implants.
Alejandro Berg
9/30/2008
Why the problem?, Use endopores 4,1x7 or 4,1 x9 that can hold a molar no problem and you skip the sinus lift..... less intervention the best prognosis specially when you dont have to much experience.
Best of luck
Empirical Medicine
9/30/2008
It is my opinion that we do not have enough information to help you.
With that said, It is my assumption that you have VERY little bone if you need to augment to get support for an 8mm implant (A length with a history of increased failure rates - see above comments).
If you are dealing with "egg shell" maxillary bone, which is my assumption, an autogenous graft may be required or at least highly advisable. Normally, I would suggest you could place just about any product in a lateral sinus augmentation to form enough bone to support 10-13mm implants.
The exception is poorly vascularized extremely thin bone.
You might want to refer this patient to a more experience surgeon for the grafting should this be the case.
I hope this helps
M. Pinto
9/30/2008
Just be sure at time of sinus lift to place enough bone, If needed at implant placement you can perform a second sinus lift with Summers technique using osteotomes or MIS bone compression kit and add 3-4 mm to your implant choice.
Just check the surgical protocol and be sure to have confidence ir your knowledge and skills.
ttmillerjr
10/1/2008
Why don't you attach a pano for us to see. I'm assuming your patient is in a full upper denture, what about the opposing? How old is the patient? Health history; fosamax, hx of sinus infections, diabetes, smoker etc etc.
* Place eight implants.
* 3mm or more bone "below" sinus, most likely you can place implants with bone graft. You are planning on lateral window entry correct? Use 13mm, try to get 5.0 in molar areas.
* I say use some autogenous bone with your mix. If you are not comfortable harvesting a block, get one of those "scrappers" and harvest bone that way. Although it's mostly cortical Arun Garg showed a couple of years ago that there is no difference in outcome verses ground block, I think the study actually compared it to bone from the hip. You can actually get quite a bit atraumatically. If you have or can borrow a prp machine (only use Harvest) that would help alot.
* I agree with not putting any implants in the central spots.
* If your patient is used to wearing a full denture it's easiest to just bury all the implants and restore later. If you want to do more you could place healing abutments and fit them to the denture, leaving the fixtures in the sinuses buried.
* fees; quote one fee= case fee. Explain your are charging for six implants(or seven) but that you are going to place eight if you can. That way if one goes south it was the free one, and the patient is getting a deal otherwise.
I could go on, but I think you have all the info you need and I need to sleep. Good luck.
DrAshish
10/1/2008
If you are doing Direct Sinus lift use autogenous bone graft along with allograft.Easy would be to use PRGF from patients blood.10-13mm a must for Posterior Maxilla along with atleast 5 mm width.
Dr.Ashish
PCP
10/1/2008
Is it a full edentulous patient? If so, why not place an All-on-4? You will have 4 long implants, in good or very good bone, with immediate function and skipping the sinus lift and the bone graft? I bet the patient would certainly prefer it.
anonymous
10/7/2008
If you plan on placing 8mm long implants, take a look at your native bone height. You may be surprised, and avoid doing a sinus lift altogether. Primary stability is the key. There is solid scientific evidence based on primate studies, that implants protruding into the sinus for a distance of 1-2mm undergo bone formation around them without any bone grafting.
Dr.K
10/20/2008
Why not just go with 24mm and call it natural root...what the hell
Dr I
11/7/2008
do any of you do direct sinus lifts and implant placement at same time? how long is adequate if done in two stages? leo
Dr I
11/7/2008
about the all-on-4 in the maxilla; anyone experience trouble with immediate torquing of implants? seems to never be an issue with lower all-on-4 's. anyone know the protocols for upper all-on-4's? leo
Dr. Bill Woods
11/14/2008
What classification is the sinus? Can you do localized lifts? Can you get primary stability? DO you have a CT? Whats the bite relationship? Bis it a bruxer? Are they wearing a denture at present? Im getting the feeling you are "thinking" abot a sinus lift. If its a lateral window, thats alot of SX to stop with 8's. Alot for the patient. Plus, you are going to lose some graft height anyway. 8's may work all the way around, but bilateral lifts are alot of work for that. Every time I have had to go to an 8 for some reason, some miscalculation, or the Sx didnt turn out like I wanted , I was a little disappointed. From an 8 to a 10 is a 20% difference in possible BIC, nothing to sneeze at. At 6-8 implants, thats 12-16mm in direct implant support. Over-engineer, I was told over and over. 8's wont do it.Go for longer and wider where you can get it. Width adds BIC. More than length. JM2C. Bill
prof.Dr.Hossam Barghash
11/16/2008
from the point of load distribution ,the diamter of the implant is more important than the length.but regarding retention, then length is more important.so the question well be what is the minimum length for good retention? quality of bone playing a role.but I belive that engament of the sinus floor cortical bone is also an important thing for good retention in this area.so tenting the implant by the sinus membrane without grafting is what we do now, plus with follow up of the cases we find out that there is new bone formation & it looks like that grafting was a factor in delaying bone foramtion ,as the graft material should be resorbed during creeping bone formation.we still studing this point.
jerry
12/29/2008
I am not aware of any literature that would contraindicate or demonstrate a lessor success rate using 8mm implants in the maxilla. If you can use longer fine, but it is not a requirement for success. As long as you are not using a turned ( smooth surface ) you should be OK.
UR
5/5/2009
Its a wide range of experiences and suggestions. Has anyone comment about the outcome of a direct sinus lift,with a tear in the lining , no infection ,no smoking and perfectly bone grafted and membranes used still ended with oroantral fistula second time repair ended again opening , any comment and advice