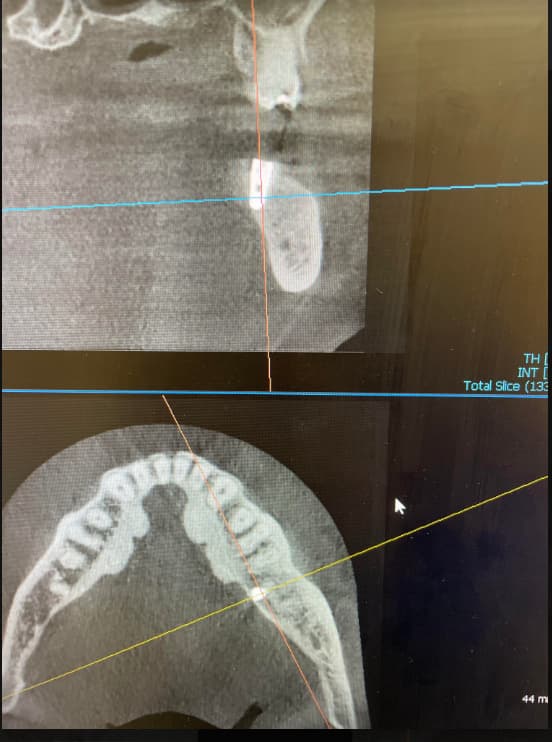
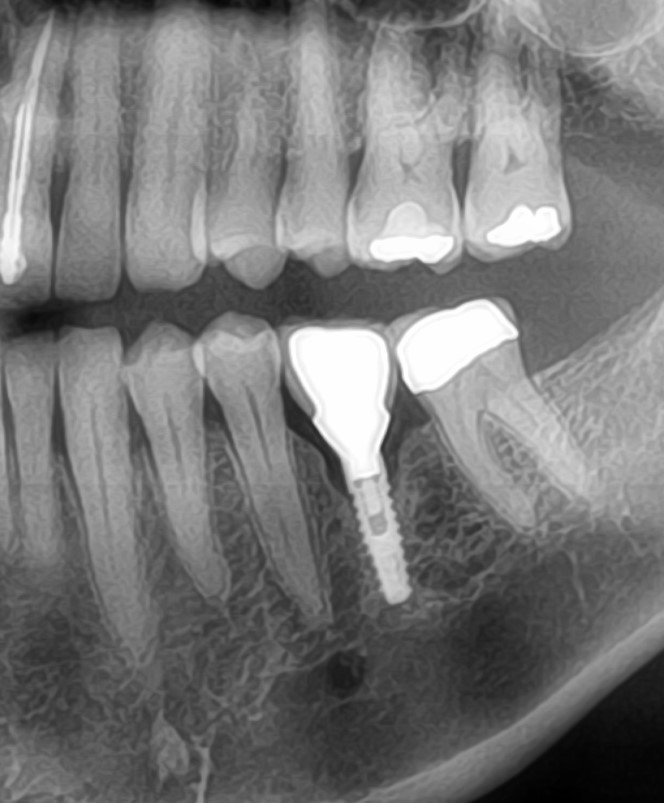
Recurrent Infection after Implant Surgery: Causes?
Dr. R. asks:
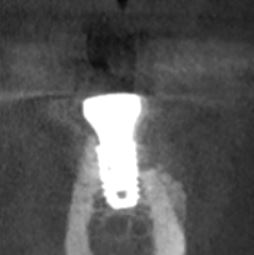
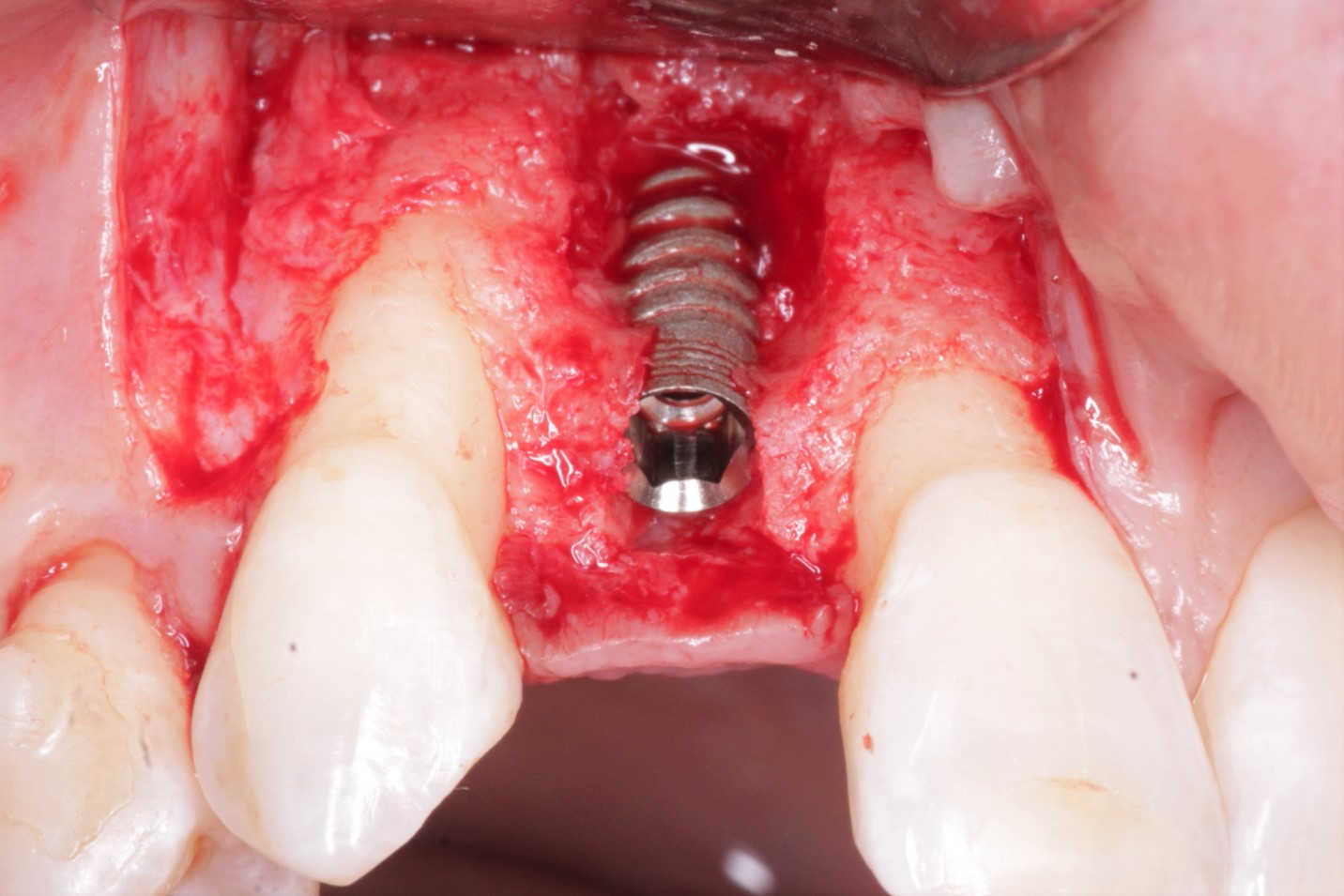
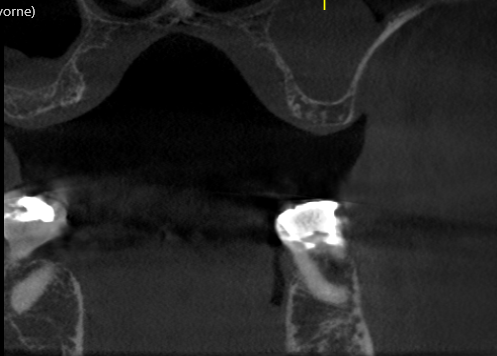
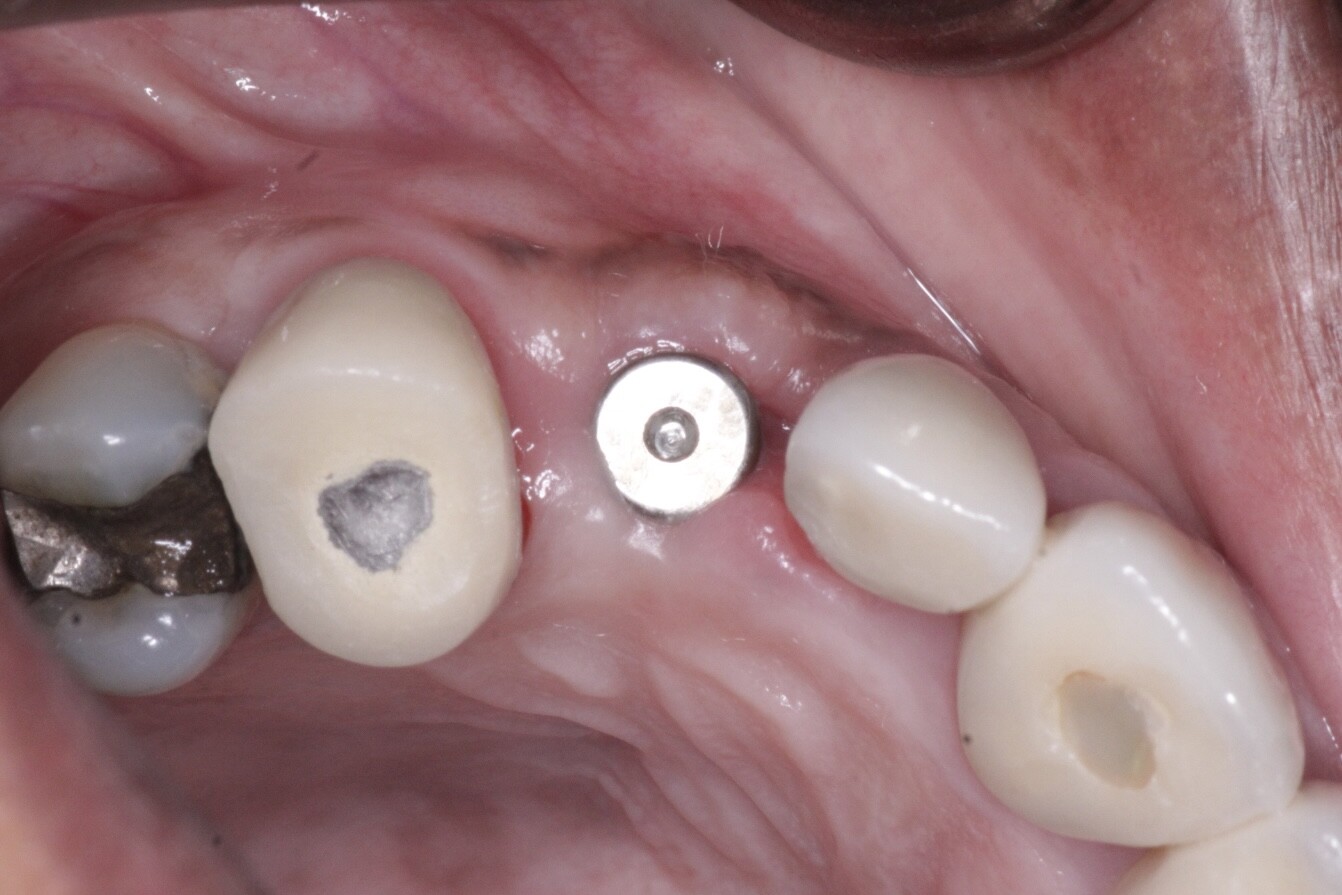
Four weeks ago I installed an implant into #18 area [mandibular left second molar; 37]. The bone type was type II -III. Two weeks following the surgery the patient presented with a fistula to the coverscrew area. I exposed coverscrew checked for mobility of coverscrew which had none and detoxified with tetracycline. I tried to leave the coverscrew exposed. I placed the patient on antibiotics. But, 2 weeks later the gingiva grew back over the coverscrew and the fistula was back. I exposed the coverscew again and again detoxified.
I realize now that I probably should have placed the healing abutment on at the 2 week time frame. Could this have caused the infection? From my understanding, if the implant is in softer bone, it is not recommended to remove the coverscew at this time since it may cause the implant to back out. That was my premise, at least, and the reason why I did not remove coverscrew at the 2 week mark. In general, what is the time frame that is recommended?
One other point that may be significant is that at the time of the initial surgery, the coverscrew fell down and it was replaced with a cover screw that had been used previously but had been cleaned and autoclaved. Could this be a factor? What do you recommend at this point?