Sinus Lift Complication Case: How Should I Proceed?
Dr. M asks:
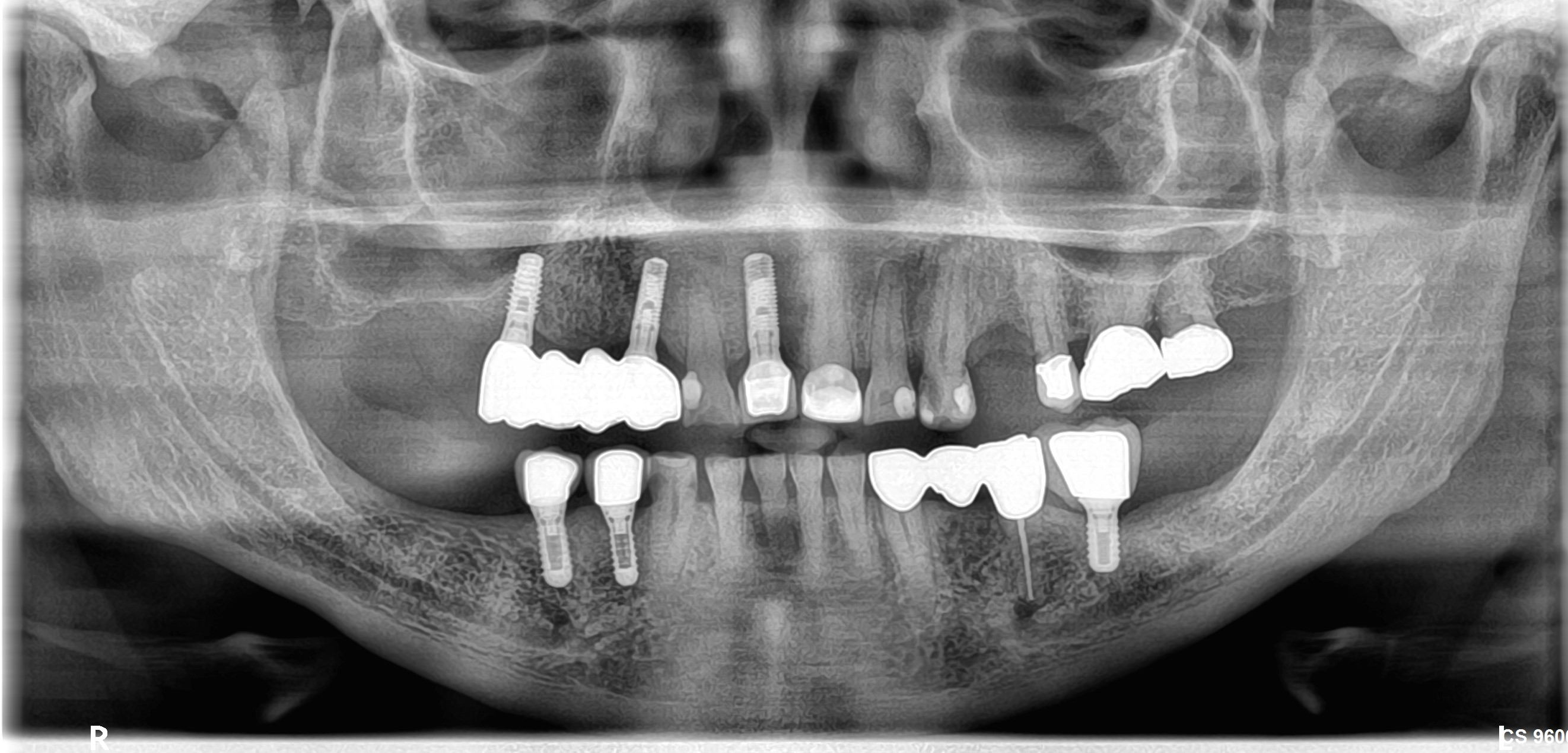
Please refer to the images below.
I did a sinus lift two and half weeks ago. There was a rupture of the sinus membrane in the mesial part of the sinus not more than 4 mm. I proceeded with the lift placed a collagen membrane covering the defect and fill the sinus, then bended the membrane outwards so it would cover the entrance too. The patient had antibiotics prior and then 8 days after surgery.
For the first 8 days the patient didn’t complain about anything. During the second week he complained that when he blew his nose there was some discharge from his nose I put him on antibiotics (augmentin + metronidazole). He got a lot better two days after.
Today almost 3 weeks after there appears to be a small oroantral fistula. But when the patient does the Valsalva maneuver no discharge is visible from the fistula. The post-operative perapical radiograph is within normal limits. Any advice on how I should proceed?
Nasal discharge and oroantral fistula after sinus lift
Small fistula