Chances of Injuring the Nasopalatine Foramen During Implant Placement?
Dr. M. asks:
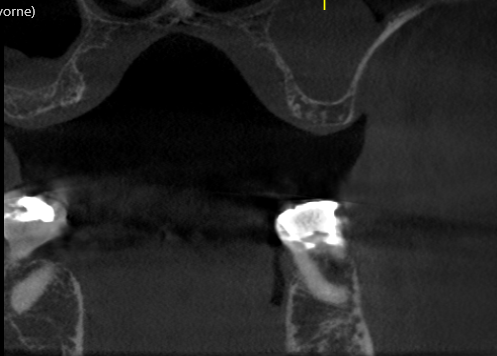
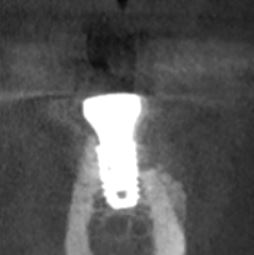
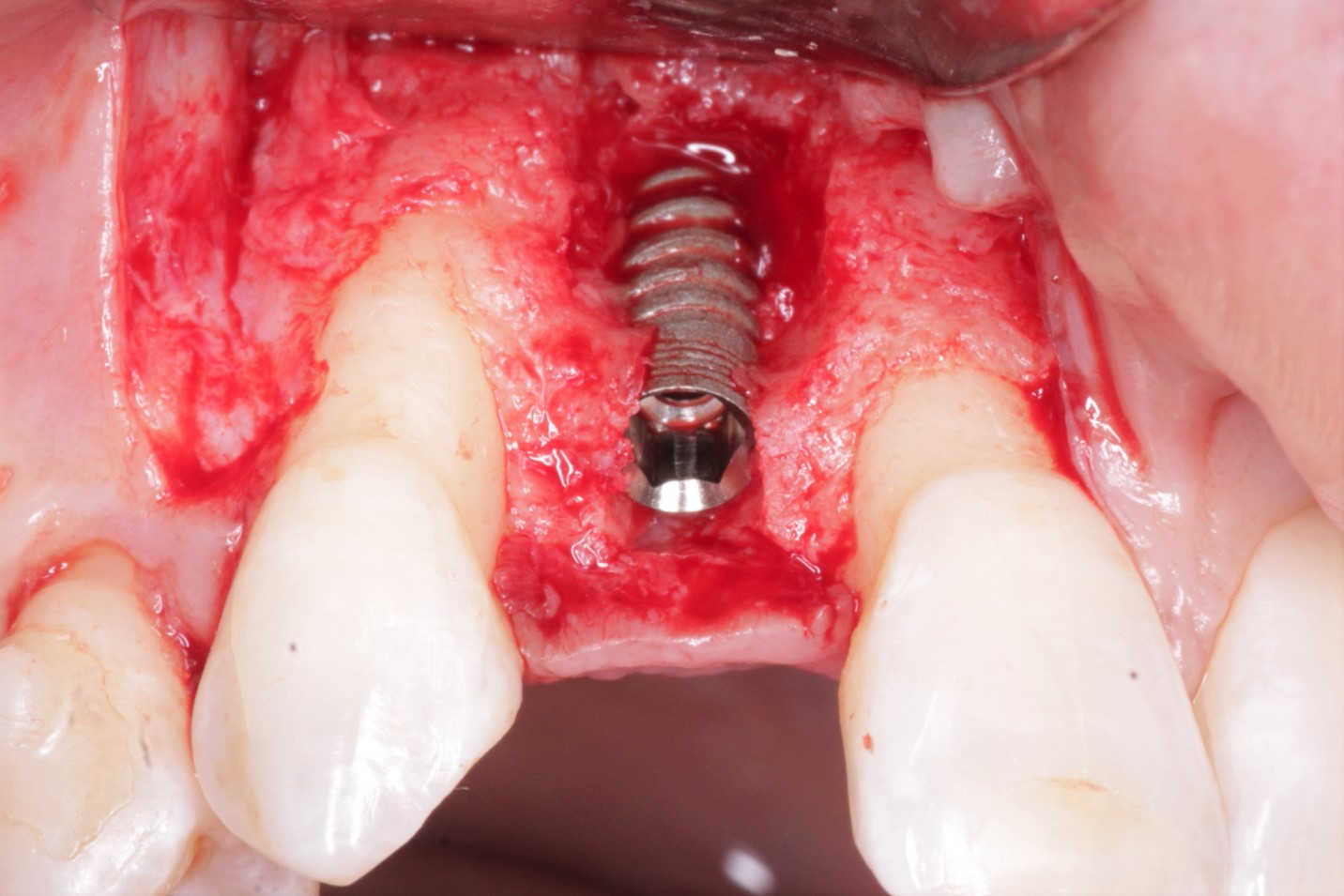
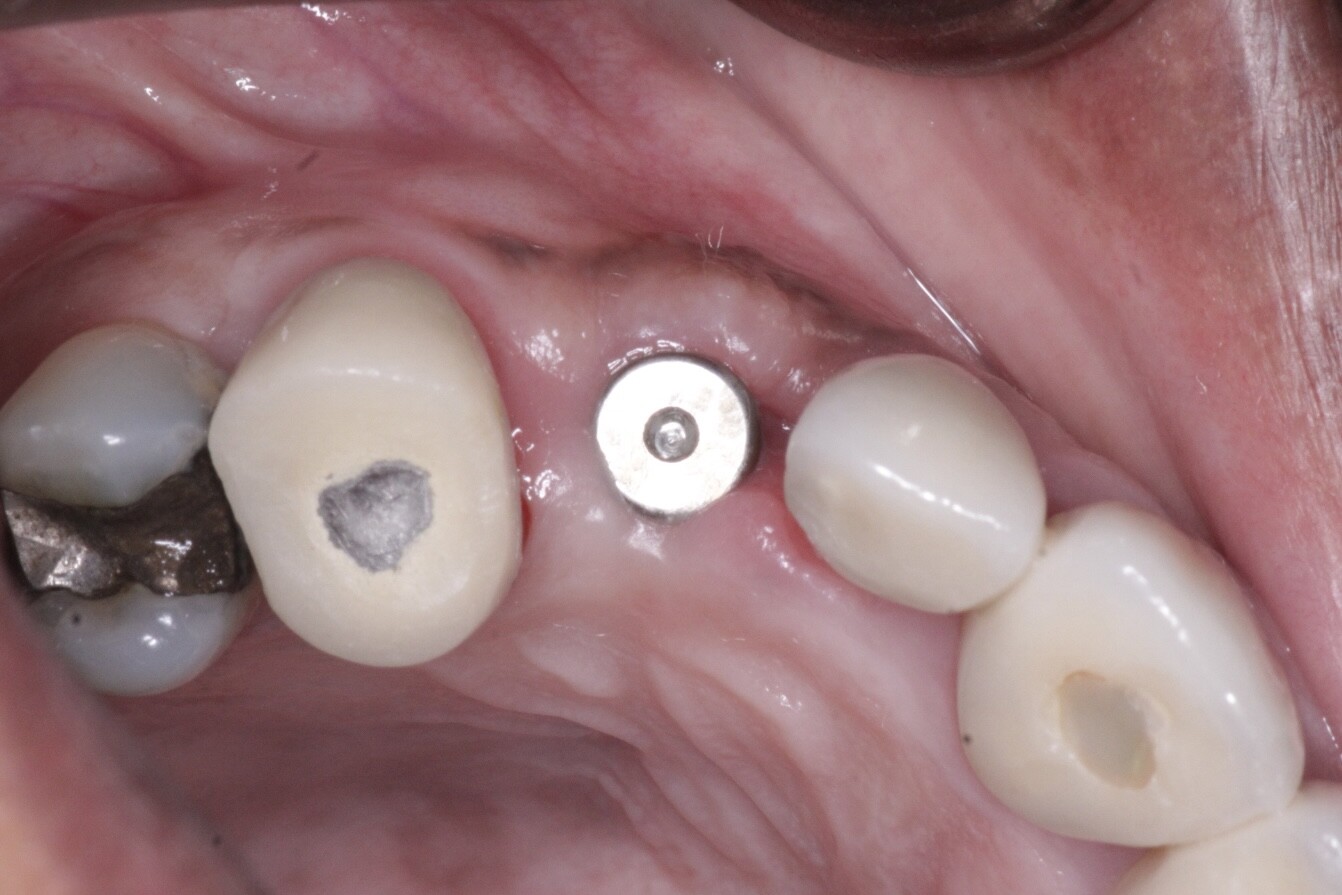
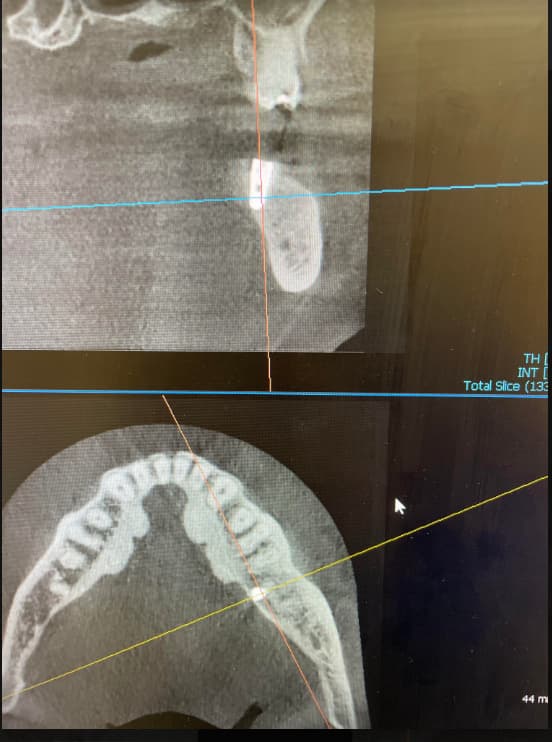
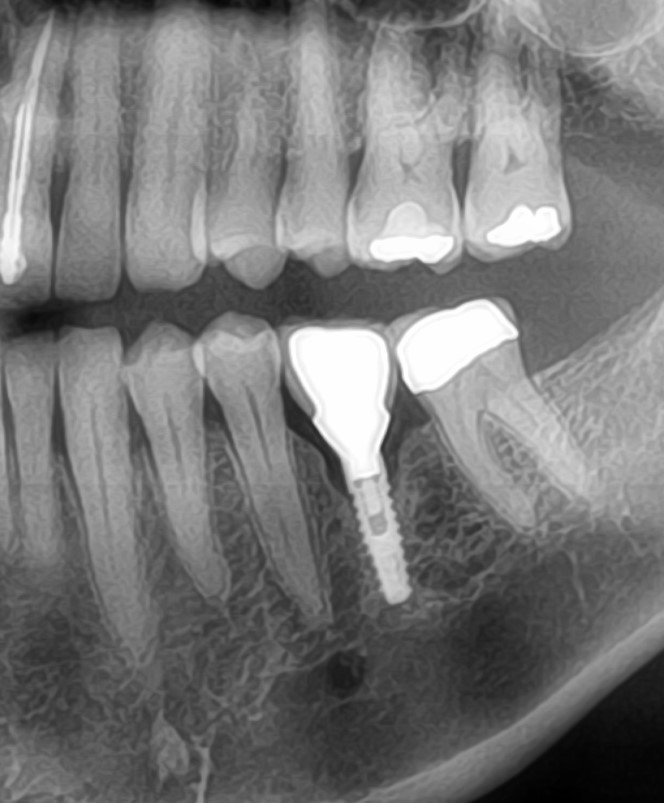
I am new to the field of implants, and I am doing just my second case. I have a patient with a fractured right maxillary central incisor [11 or #8]. I am planning to place an implant immediately on extracting the tooth . On the periapical radiograph the root apex appears very close to the nasopalatine foramen. What are my chances of injuring the nerve? Would it be enough if I maintain the mesial limit of the extraction socket when drilling to place the implant and when torquing down the implant? Would this be a situation where a cone beam volumetric tomographic scan would provide valuable information?
8 Comments on Chances of Injuring the Nasopalatine Foramen During Implant Placement?
New comments are currently closed for this post.
Randall N Ruff
6/15/2009
I routinely remove the contents of this canal, graft it and place implants in it, or more accurate, infringing into the space. The soft tssue contents of this foramen should be removed though, if an implant is going to be involved in this space. I do not want any soft tissue to infiltrate the implant itself
alejandro berg
6/16/2009
I agree with dr ruff, but I try to avoid it when i can, try to drill and torque the implant away from it if possible, if not , be agressive and go all the way with the removal and the graft.. usually if you dont do it that way you will get into trouble.
Dale Miles
6/16/2009
The "soft tissue" contents are the neurovascular supply to the anterior palate and surrounding tissues. Why would you remove these since they bring some of the blood supply to the very region you want to heal? Any problem with palatal "numbing" post NPC content excision?
You may want to read the article below...
http://dentistry.ucsf.edu/continuing/0111008coursedocs/Implant%20relevant%20anatomy.pdf
Joseph Kim, DDS
6/16/2009
Very little sensory deficit from removing nasopalatine soft tissues. Well documented in the literature. The reason you need to avoid with the implant is increased chance of fibrous integration in the area of the foramen.
If you hit an artery in the area, this is how I deal with it: Artery in bone: place surgical suction directly on the bleeder, so I can identify the exact location of the artery. Then, using the sharp end of a periosteal elevator, I crush the bony housing directly inferior to the artery in a superior direction (towards the palate). Sometimes you need to start a little further away from the lumen, usually no more than 0.5 mm. Soft tissue: these are kind of tricky if the artery is larger, but I never place a hemostat on it. I always suture with polyglycolic acid (generic Vicryl). Suction as above, then raise a full thickness flap that incorporates the artery. Then place the suture from the periosteum side, being careful not to go past the epithelium, keeping the suture in the subdermal tissue, or just above the artery. Then tie a triple knot (doubles always slip for me with PGA sutures), and a double square know on top of it. Trim it short, and close normally.
Having said all that, I don't mess with the foramen unless it is definitely in my way to achieve an ideal prosthetic result.
jon
6/16/2009
Dr. M,
I would strongly recommend, since it is your second case, to refer. The maxillary anterior is the most challenging area to treat with implants as it is in an aesthetic area and soft and hard tissue is critical here. If you have a fracture you may have bone loss and thin tissue and this could end in terrible aesthetic results (especially if the patient has a high lip line). The bone in the maxillary anterior is very thin usually (even without fracture) and I routinely have to flap and graft the area at the time of implant placement. You really need experience in these cases. I am biased as I am a board certified periodontist but I have seen enough cases done poorly and it can be horrible if you do not have experience. Start out in molar areas with good bone width and height as aesthetics are not as much of a concern and then move to the maxillary anterior once you are comfortable. #'s 8&9 are my most challenging cases still and I have placed thousands of implants. A patient will appreciate your wanting to do the optimum care for them and be much happier if the implant if placed well. Ask youself: Knowing what you know, would you let yourself or your wife have an implant placed by you in this case? If the answer is no, refer. If it is yes, go for it.
RB
6/16/2009
I did one of those but the socket was so huge having done an atraumatic extraction that none of my pilot drills would engage properly I had drilled about 2mm.
So I stopped and told the patient that if I can't engage the drill , it means that I won't be able to engage the implant in the fresh socket and at that time the best I could do was to fill up the socket with bone grafting material and wait a minimum of six months.Patient agreed. Reported nose bleeding three days post-op. No bleeding immediate to surgery. I placed the implant eight months later and restore it six months after and no problems sofar.
RB
Gerald Rudick
6/16/2009
Dr. M... what a great question!!
I just returned from the AAID North East and Southern Districts combined annual meeting held in Boston June 11th - 14th, 2009.
We had the priviledge of listening to lectures by Dr. Hilt Tatum, and celebrating his 75th birthday.
Dr. Tatum, the father and originator of sinus lifts, amongst other things, introduced us to his new concept of vacularized bone grafts.
He demonstrated and lectured on a new technique of being able to disconnect a segment of bone in the #11 or #8 that was the original socket, but was resorbed to the point that placing an implant into that bone ( if left in the original state) would lead to having an implant that would be restored with an over elongated crown at best.
Dr. Tatum demonstrated making two vertical incisions in the adjacent soft tissue one tooth removed on either side, and then gently peeled open a small vertical view and proceeded to chisel vertically through the bone just mesially to both adjacent teeth, and from buccal to the palate... a complete cut.
Then, he gently opened a horizontal tunnel at the level where the root apex was and disected the mucoperiosteum as high as possible thereby releasing the soft tissue apical to his intended horizontal bone cut.
With his own brand of Tatum Chisels, he chiseled a horizontal cut into the bone, making sure that as the chisel worked its way horizontally across the buccal plate, it was directed slightly downward toward the hard palate, to avoid entering the piriform plate and possibly the anterior sinus.
He made a semi lunar incision midline in the palate in an antero-posterior direction ( not cutting the soft tissue behind the section being cut, but pushing it aside, in order to preserve the blood supply)and reflected the soft tissue behind the #11 (#8)and continued his chiseling until the segment of bone was disconnected. The bulk of this block was still fully vacularized on the buccal,the crest of the ridge, and part of the palatal aspect.
Once the block of graft was lowered (because of the released apical gingival tissues)to a position lower than the approximating bone on either of the neighboring teeth, a block allograft or autograft was fitted into the space created to hold and support the lowered disconnected original socket.
I asked him if he was concerned about damaging the neurovascular bundle of the incisive foramen when making this cut through the bone; and he said that this was of absolutely no consequence or concern.....as a matter of fact the excessive bleeding from the bundle is very good to supply and nourish the bone block. The bleeding is controlled by suturing,using glue, and placing a pack over the
wound.
This procedure, developed by Dr. Tatum, is a technique that should be attempted by the more experienced dental surgeons.... but it is the beginning of a new era in bone grafting that will ultimatley result in the development of better boney sites for anterior implants with ideal emergence profiles in the esthetic zones.
I have not as yet seen an article published by Dr. Tatum on this technique but I am sure it is in the making.
Gerald Rudick DDS Montreal, Canada
Scott Noren
1/9/2017
any diagrams of this technique available?
Scott