Dental Implant Spinning in Socket: How to Manage?
Dr. A. asks:
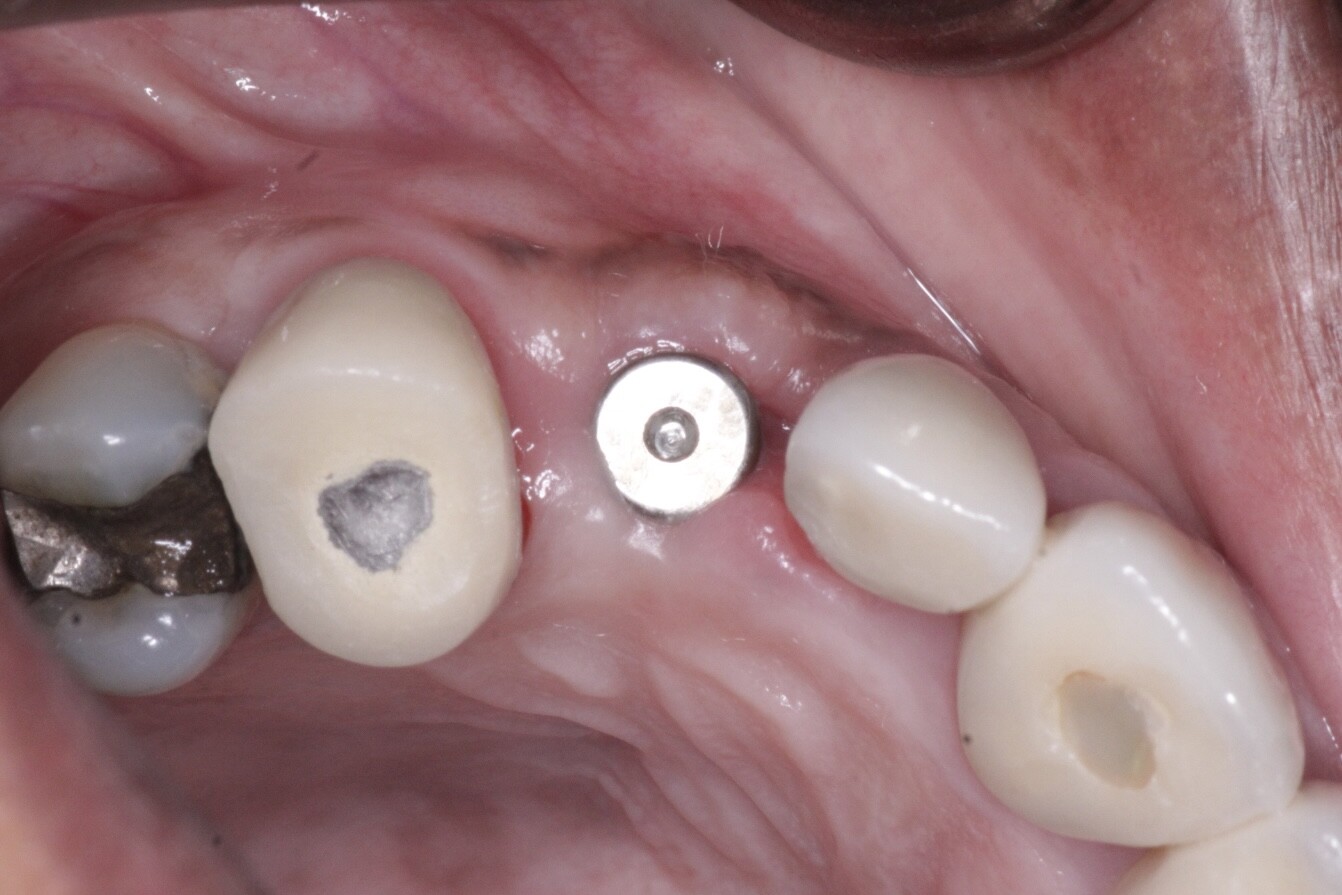
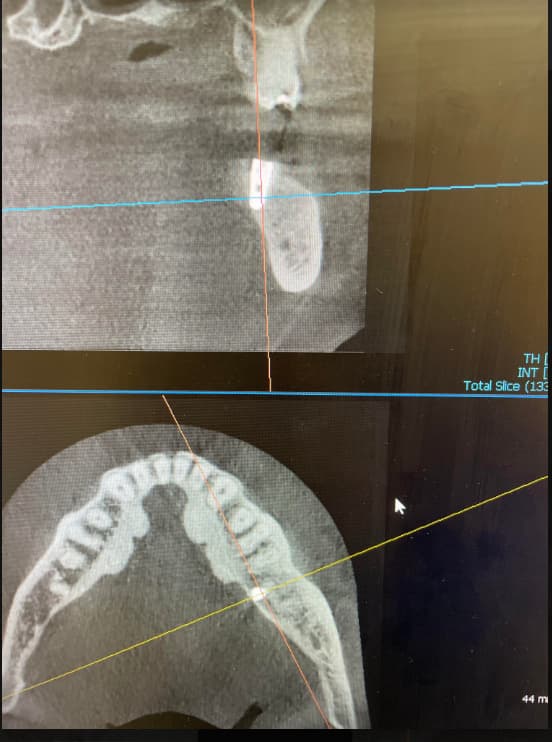
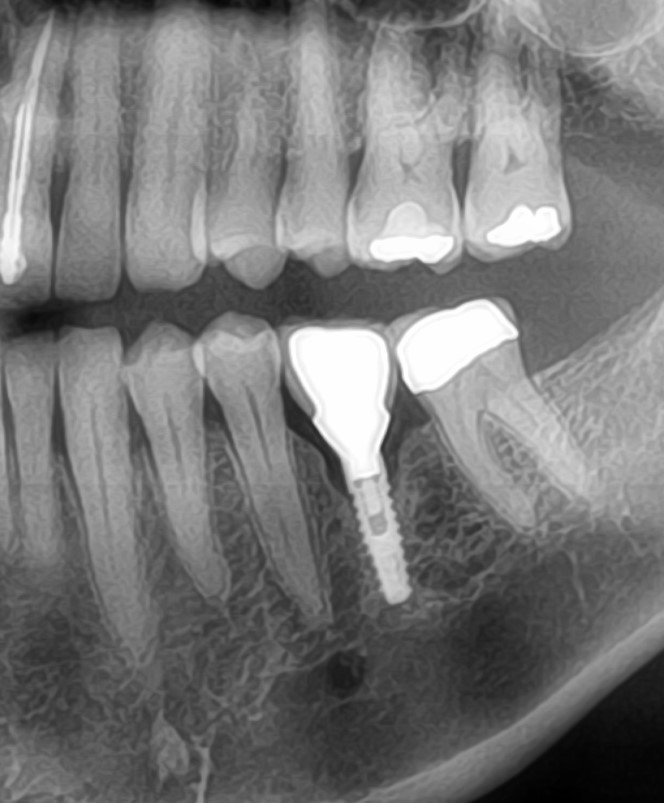
I placed an implant in the maxillary molar area 6 months ago. The bone to implant contact appears excellent on the radiographs. There are no radiolucent areas along the implant and the soft tissue is normal. In other words, all signs were positive for osseointegration having been achieved. But when I went in to torque down the abutment, the implant began to spin in the socket. What do I do now? How do I prevent this from happening again? Are there any standard protocols for managing problems like this?
34 Comments on Dental Implant Spinning in Socket: How to Manage?
New comments are currently closed for this post.
Dr. Dr.
6/15/2009
You can never grade mobility on an implant. If it's not intergrated after 6months. Then you shall remove it.
Put e.g BioOss in the socket. wait for minimum 6 months and place a implant with a good surface. (Astra or Straumann SLActive.)
salim shafi
6/15/2009
This has happened to me before,especially in a grafted site where primary stability was less than perfect.For what it is worth ,here is my recommendation .Remove cover screw ,gently !! ,place implant driver and tighten implant .It would be helpful if implant has aggressive threads.If implant can be driven 2-3mm and has good stability, replace cover screw, leave minimum 6-8 weeks and try again.It has worked for me , worst case, at 8 weeks removal of implant, graft and start over again .
DR. B
6/15/2009
soft tissue develop on implant surface causing mobility. it is hopeless, don't waste any more time, remove it than graft it or place a longer and wider implant if there is no obvious infection.
Peter Fairbairn
6/16/2009
Forget it take it out leave for 3 months and replace you cannot hope or pray in this case.
Dr. H. Ryan Kazemi
6/16/2009
The implant is clearly not integrated and should be removed. The site can be cleaned (remove soft tissue, inflammatory tissues, necrotic bone,etc) and graft if necessary. Otherwise allow to heal for 3 months and then implant placement can be done again.
There may be several contributing factors to this type of problem:
1) Implant not having primary stability in the bone when placed (either due to overpreparation or very poor bone quality)
2) Tissue damage during preparation
3) Excessive forces if done as single stage with healing abutment
4) Smoking
hope this is helpful.
Dr. Kazemi
William
6/16/2009
IF you can remove it and prep for a wider and slightly longer implant, that would work as well.
Bruce G Knecht
6/16/2009
The Paitient could be very osteoporotic and this could cause the impalnt to move on torque. If this is not the case you can remove the implant and use a slighly wider implant and screw it in the same place. The new size will strip aout the fribrous tissue inrtergration and you have a second chance. i have done this once and it worked.
Richard Hughes DDS, FAAID
6/16/2009
Yor will get a spinner every now and then. You cannot always tell from the radiograph due to the fact that the implant is in cancellous bone and the cortical bone is thick. So , the x-ray beam does not penetrate well or the cortical bone will mask the defect around the implant. Solution for a spinner is by one of tthree ways: remove, detox, graft and give it time; the other is to remove, detox, grout with a graft material and replace the third is to tighten and if activated, then fixate. The causes are many from heatinf the bone during the osteotomy procedure, poor inital srability, bone necrosis from pressure, poor regenerative qualities of the bone for various reasons.
jon
6/16/2009
Take it out, degranulate area, replace with a longer or wider implant if possible. If not possible, graft and come back in 4-6 months later.
Mike Heads
6/17/2009
If it has been left for six months then the implant will be encapsulated with connective tissue and simply tightening it is unlikely to solve the problem. I would agree the best solution is to remove it ASAP. If there is no buccal or lingual/palatal bone missing then simply allow the socket to heal for 8-12 weeks before replacing the implant, remember the body replaces natural bone much qicker than it converts grafted bone. If you graft the osteotomy site you will have to wait 6 months to be able to place another implant. If there has been bone loss then yes you will probably have to graft the site and wait the six months.
Peter Fairbairn
6/17/2009
I think the biggest cause of spinners is residual infective tissue or adjacent tooth infection ( RCT tooth with area). As we create the osteotomy we provide a drainage route which lines the implant.
John Clark
6/17/2009
What torque did you use?
Too late for this implant, but with future implants you may like to consider using a staged loading protocol as taught to me by Dr John Giblin (Sydney, Aust). He now advocates staged loading which involves an assumption that integration has taken place (using normal parameters mentioned before on this site), however, the 'cement' (integration) is weak and so only minimal torque is applied during the impression and with the final insertion of abutment and crown (typically 15-20Ncm). Then after 3 months in function, the crown is removed and the abutment torqued up to normal values (32Ncm) with the belief that the 3 months in function has strengthened the integration. John's apprroach comes with 20 years of experience behind it and it works for me! I like to use 2/3 temp bond and 1/3 vaseline for the 3 month interim period and I warn the patient that the crown may come off..
regards John
Don Callan
6/17/2009
You have two choices.
One; Take it out and remove all soft tissue and place a larger implant and allow 3-4 months of healing time.
Second; Take the spinner out and remove all soft tissue and wait 6-8 weeks and place another implant.
Both choices will work
Dr John Murray
6/17/2009
Spinners have failed - replace it
Mohamed H Mohamed
6/17/2009
I was wondering if you can post the X-ray associated with this case especially the one just before the spinning
thanks
xe
6/18/2009
salim shafi and richard hughes only know what theyr talking bout...all the rest just placed an implant once and think they r implantologist.U actually got a chance to get the spinner working...u will have this problems many times in D4 bone as it is in the back of the maxilla.Retorque it like they told u and give it 2 months..will probably work
best of luck
Edentulous Artist
6/18/2009
I have never fully understood how orthopedic surgeons immediately load hip and knee replacements all day every day and we in dentistry cannot seem to accomplish this?
Paul
6/19/2009
Take it out, degranulate, replace with a wider implant. Impress in 3 months.
Richard Hughes DDS, FAAID
6/19/2009
That's a good one. I believe the orthopods used a similar acrylic like we use for provisionals or dentures to lock in the implant. Plus their screw designs are better.
Richard Hughes DDS, FAAID
6/19/2009
Xe, Thank you!
Brian James
6/23/2009
I think management depends upon the clinical radiographic appearance. If there is a frank radiolucency, take it out. If it apparently looks ok, leave it alone and see how it torque tests in 8 weeks. They can recover on occasions, but let the patient know you are not banking on it, and there may be a chance of redo.
kiran kumar
6/23/2009
if the implant doesnt have any radiolucent area around it in the radiograph then it most probably has integrated but is spinning becos it doesnt have enough bone implant surface contact area.
retorque the implant gently and place a permucosal healing cap and allow it to load passively with the tongue and cheek musles acting on it gently.in 6to 8 weeks and the bone around gains density and then u can load the implant with a temporary crown completely out of occlusion.wait for 4 weeks and then make impressions for a permanent crown.
this is no new technique but a very time tested progressive loading always advised for implants placed in d4 bone.hope this suffices all the best.
odo perio
6/29/2009
i tried to place an implant- strauman like- in d1 bone lower jaw,It was very hard to torque it: 1000 rpm/ 56 nt/cm2 couldnt do it with handpiece and removed it and tried agai with the rachette.primary stability ok,wound closure ok
do u think now that the implant is contaminated with saliva or blood and it will fai for sure?
cory c.
7/3/2009
because i hate remakes i've tried to salvage the spinners i've had in various ways with overall about 50% success rate. i've done the careful removal of healing cap and litely placing abutment w/out torq and place crown out of occ. this works if you can stabilize implant crown with tight interprox. contacts,if you're using it for a denture attachment, forget it.i've tried the "screw it deeper" aproach and it worked like 1 out of 3 times.one time i had one that looked great like yours [radiographically and clinically] but was actually strip perforated on the buccal[i had used a tissue punch during placement]i flapped it and grafted the defect and it worked great.point is,it's already there so give it a shot,you might develop a tecnq we could all use.
naji k
7/9/2009
best way to proceed in my opinion is to remove the implant coz any further suicide attempt will bring more damage to the socket and bone loss
i thing you rather assess the bone quality during the drilling procedure and choose either an underprepared site and or conical shaped implants to augment the primary stability
dr. Amir
7/9/2009
There are protocols. Easy - any of the 3D scans would tell you where you put your implant. Most likely the greater part of the implant, if not most of it, you placed in the maxillary sinus, perhaps holding a part of its' vestibular vertical wall. Protocols are simple to the extreme: ISQ (Ostell) value at time of placement gives you insight on what you did and where you put it. At reentry you measure it again and compare to the previous value. It must be over ISQ 65. Otherwise you most likely put it in the sinus or perhaps holding a part of its vertical wall. If you need a conformation, and you most definitely do, go ahead with the 3D scan. And all your doubts go out to the open. 2D radiographs really don't do much help cause of the recession of the sinus. It's all really easy, I don't know what's the discussion all about.
Dentist Thornhill
7/15/2009
Unfortunately, it sounds as though the dental implant is not integrated. You are probably better off removing the implant and starting again rather than prolonging the treatment time for the patient.
salim shafi
7/27/2009
Perhaps, Dr.A could follow up with which course of action was decided upon and if more time was allocated for integration, it would be nice to know the outcome.Please keep us posted and good luck .
Richard Hughes DDS, FAAID
7/27/2009
Remove the spinner and then degranulate if necessary, graft with osteogen, make sure the site is bleeding and place another implant or graft and place an implant at a later date.
jon
7/28/2009
Hey, Hughes changed his mind. You can take it out now or after the implant has been restored. Either way it is coming out. If you take it out now the patient and the GP is much more likely to be pissed off. Do not try to salvage this based upon what you are saying. Ask yourself, if I were the patient would I give it more time or remove it and replace it. That will give you your answer.
Richard Hughes DDS, FAAID
7/29/2009
Jon, Each situation determines what course to take. I have seen many situations, some are similar and some are not. One has to use common sense and think on their feet. A true spinner has to be removed. an implant that backs out, can under the right conditions be used. Here again the term is, right conditions.
Dr.Tawfic Rabi
9/17/2009
Implant is not intergrated to the bone,most probably due to over instumentation,poor bone density.You did not mention how the initial stability of the implant in the bone was(torque).
I think that it is better to progressively load implants in the maxillary posterior area,ofcourse after achieving radiographical and clinical signs of intergration.
Gregori M. Kurtzman DDS
12/29/2009
Unlike with natural teeth, with implants its either completely non mobile or its got some mobility. Any mobility indicates it has failed to integrate. And as such needs to be removed and the area retreated. The exception to this is inthe maxilla due to the softer bone it is possible when removing a healing screw or abutment or placing a part to get a green stick fracture in the area adjacent to the bone implant interface. This will typically be noted as slight rotational movement of a few degrees. when noted the implant should be put to sleep and allow this area to heal for 6-8 weeks then renter to check integration. If you get significant rotation this indicates a fiberous area which can be very thin between the bone and implant and may not be noticable on the radiograph and the implant should be removed as it will not integrate at that stage. So we need to differentiate between "spinning" and "rotating"
Gopianandan
5/3/2018
I am inserting implants sincerity Feb 1996.From 1998 my implants were manually turned ,in situations like this I increase the diameter of the implant by 1mm and insert it.