Failed Bridge with Bone Loss Case: How Would You Place the Implants?
Dr. M asks:
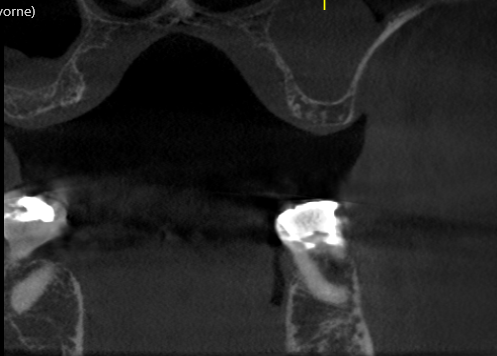
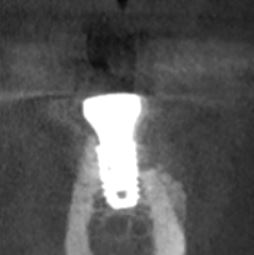
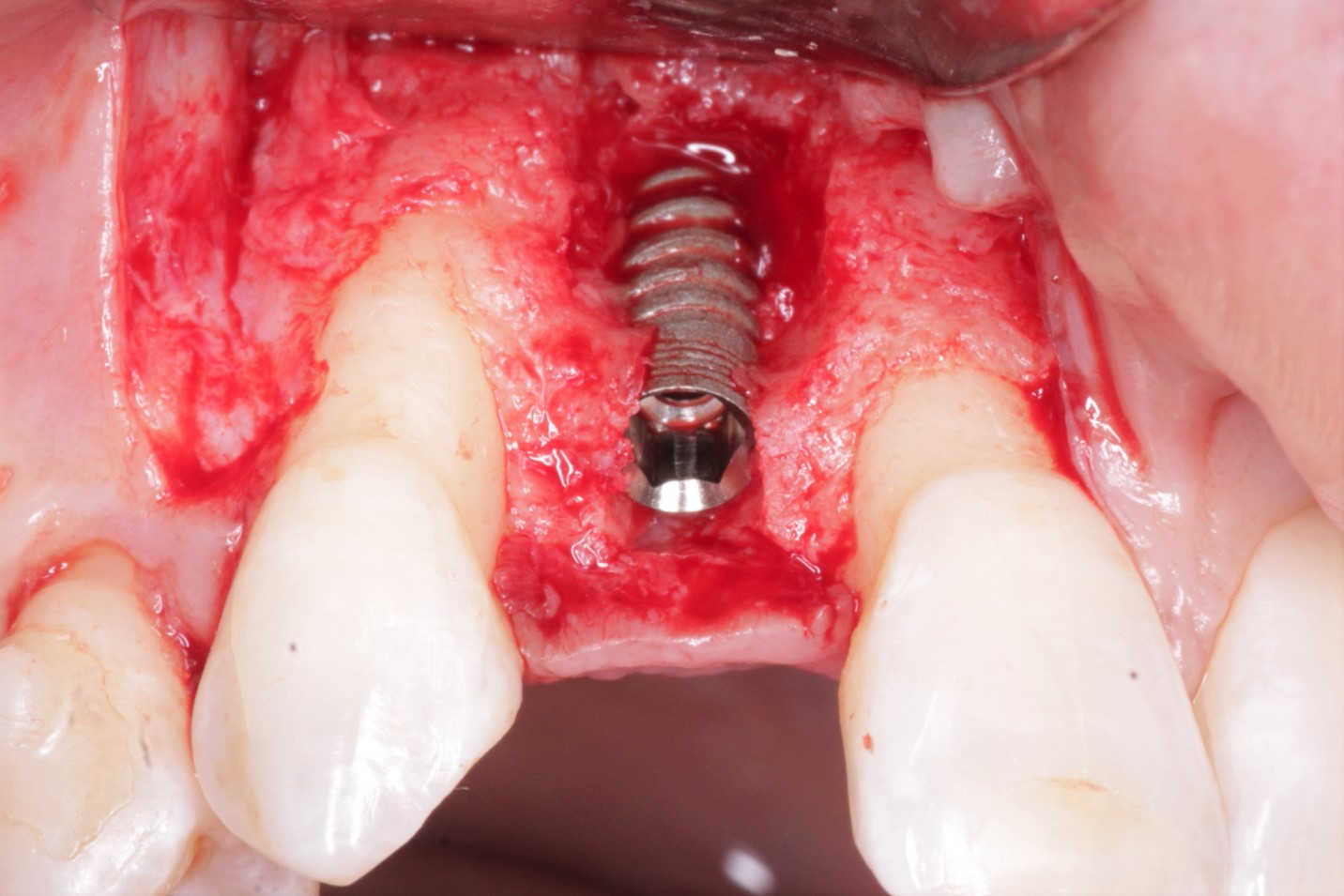
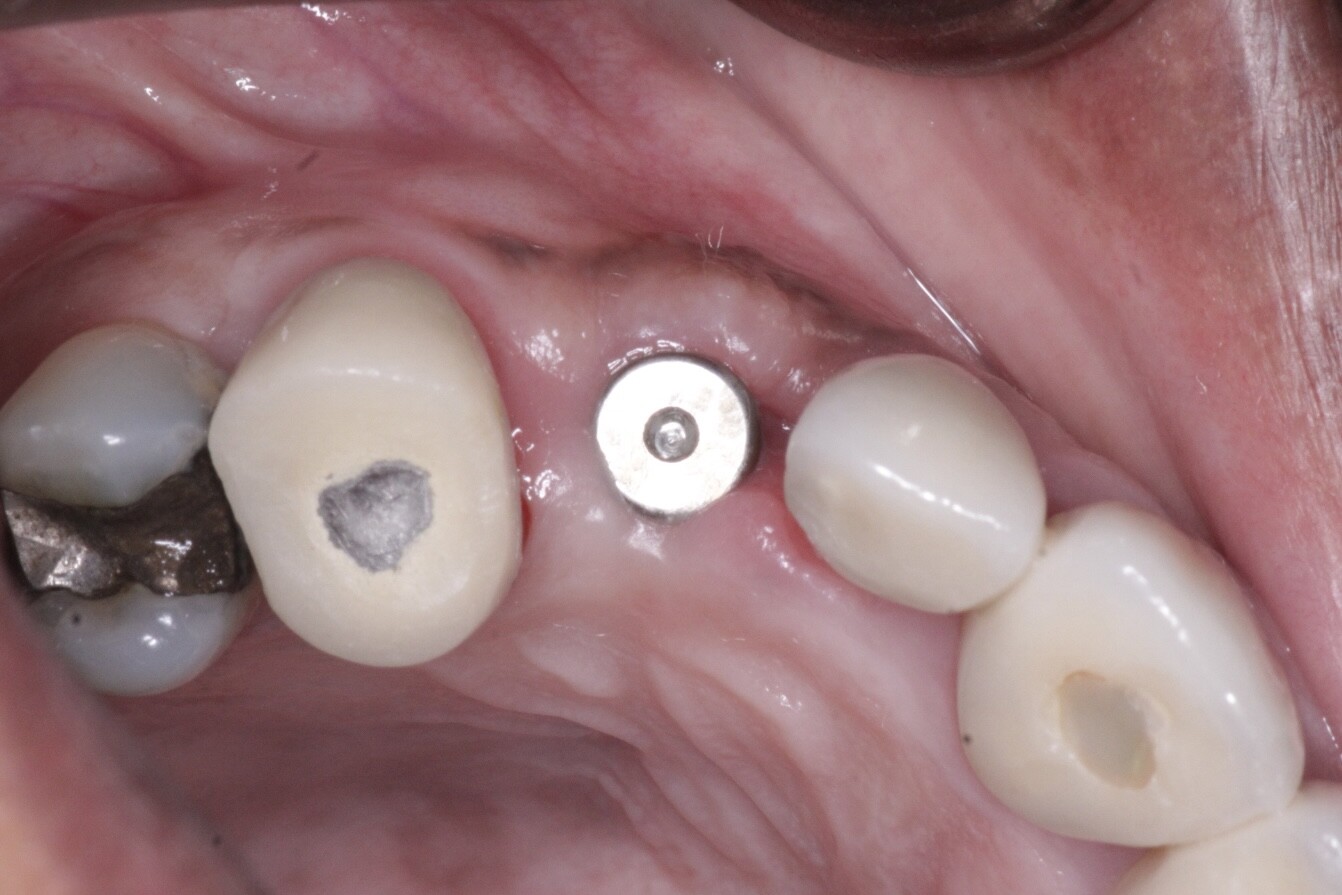
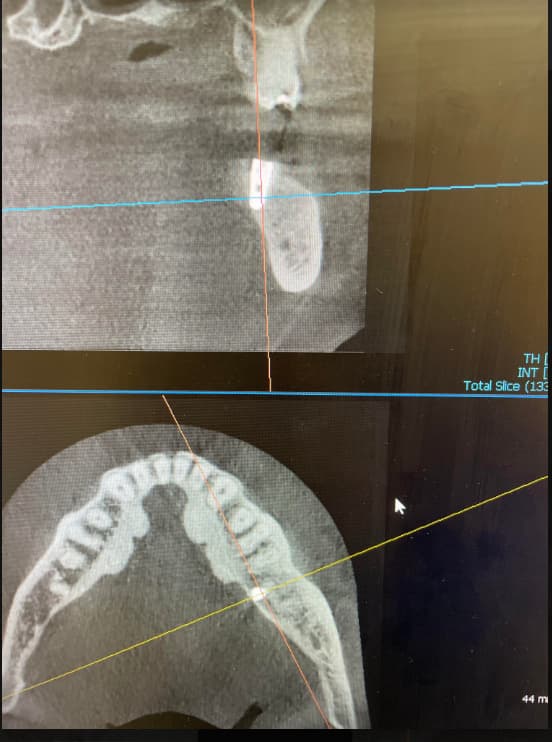
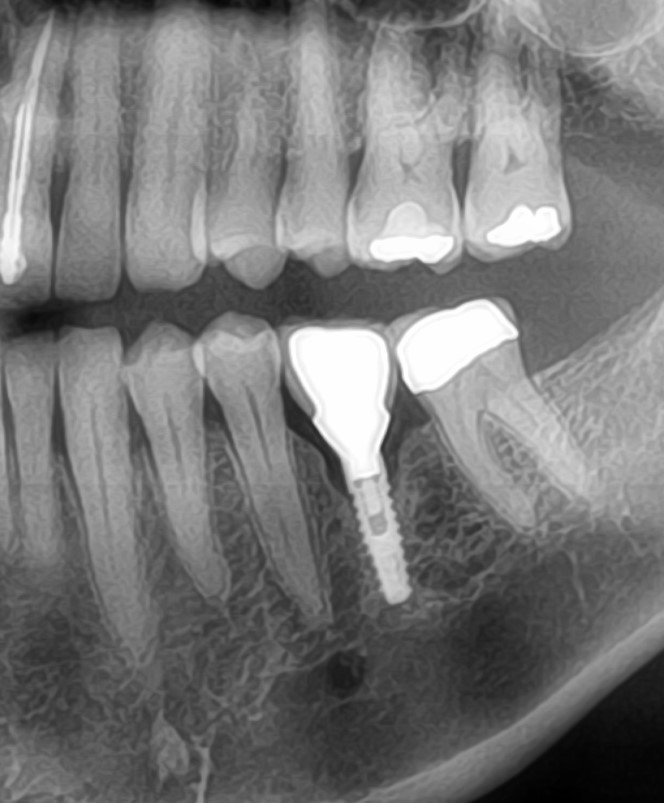
This 40 year old patient (see case photo below) has a failed bridge extending from the maxillary left second premolar to the maxillary left canine as well as a single crown on the maxillary left lateral incisor. Although a chronic periodontal infection related to the canine and lateral incisor (grade II mobility) has resulted in moderate bone loss and a crater-like bone defect, the overlying soft tissue appears clinically in level with the gums around adjacent teeth and a CBCT showed it was about 6 mm thick over the alveolar crest. My plan is to have the canine and lateral incisor extracted to avoid more bone loss, the second premolar endodontically treated, and 3 implants placed in the edentulous area. Regarding this degree of vertical bone loss, would you consider placing the implants like 2 mm supra-crestal together with vertical ridge augmentation using a Titanium reinforced membrane to avoid having long crowns (but I am afraid of the deep pockets that would res ult around the abutments!!) ? Or would you place the implants in level with the available bone and depend on the good vertical position of the gums to give you nice looking restorations?