David M. H. Lambert DDS (
I personally take a case specific approach to flapless versus open approaches or even guided approaches. For example, what I have found, primarily from the school of hard knocks, is that having a very very accurate and detailed dental history is absolutely the most important aspect when determining the need for flapless surgery in the maxillary anterior region. If there has been blunt trauma, surgical trauma, multiple endodontic procedures, apical surgery, external or internal resorption - these are some predictors that suggest an increased possibility for vascularity issues and the need for flapless surgery. These cases I try to do guided and flapless. Nevertheless, even with a flapless approach, I stil have seen cases melt.
Another situation where I'll go guided and flapless is if I need to place multiple implants, say in an edentulous maxilla case or any case where I'm really concerned about parallelism (even with angled abutments, lol). It's just easier, IMHO.
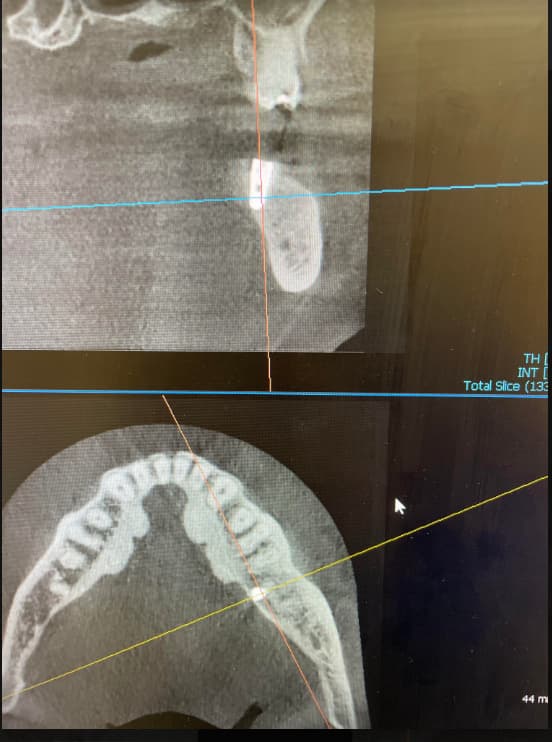
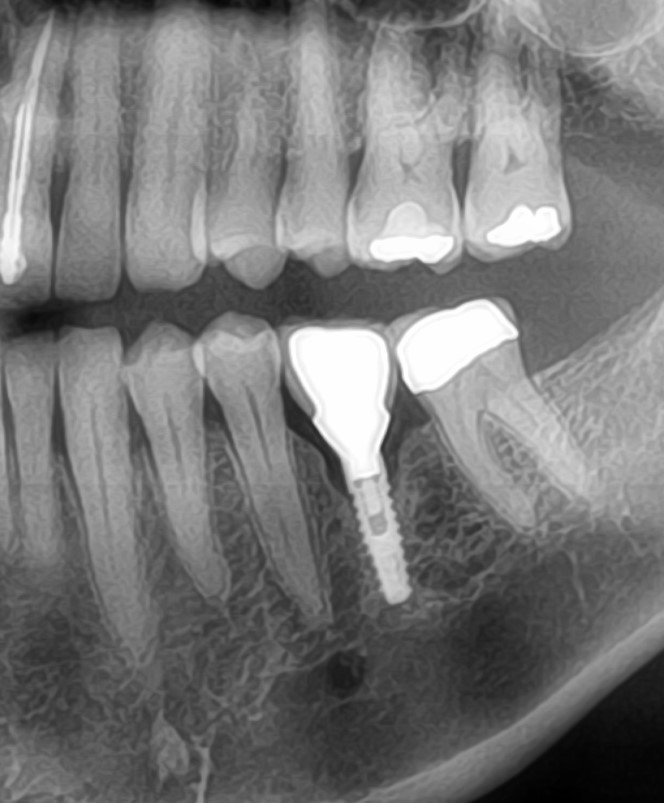
If I'm in a situation where I'm concerned about nerve impingement, I'l go guided and flapless.
Actually, if you go guided, theoretically there's really no reason to raise a flap right?
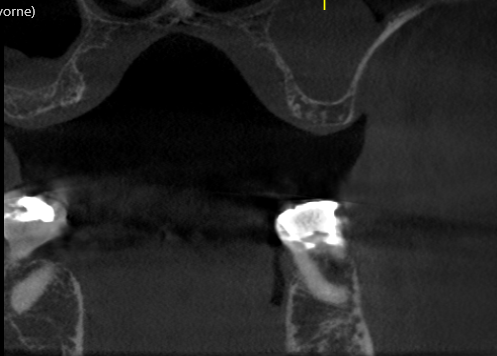
Well, not always. I have found using the Materialize stents you need to be very careful. If your virtual surgery shows very very little space between the cortices, don't thing you can use a guide to split hairs...it won't work. The tolerances of these systems really do need you to have at the very least 1/2 to 1 mm at a minimum of distance between the implant and cortical plate. These systems are accurate, but they are NOT precise.
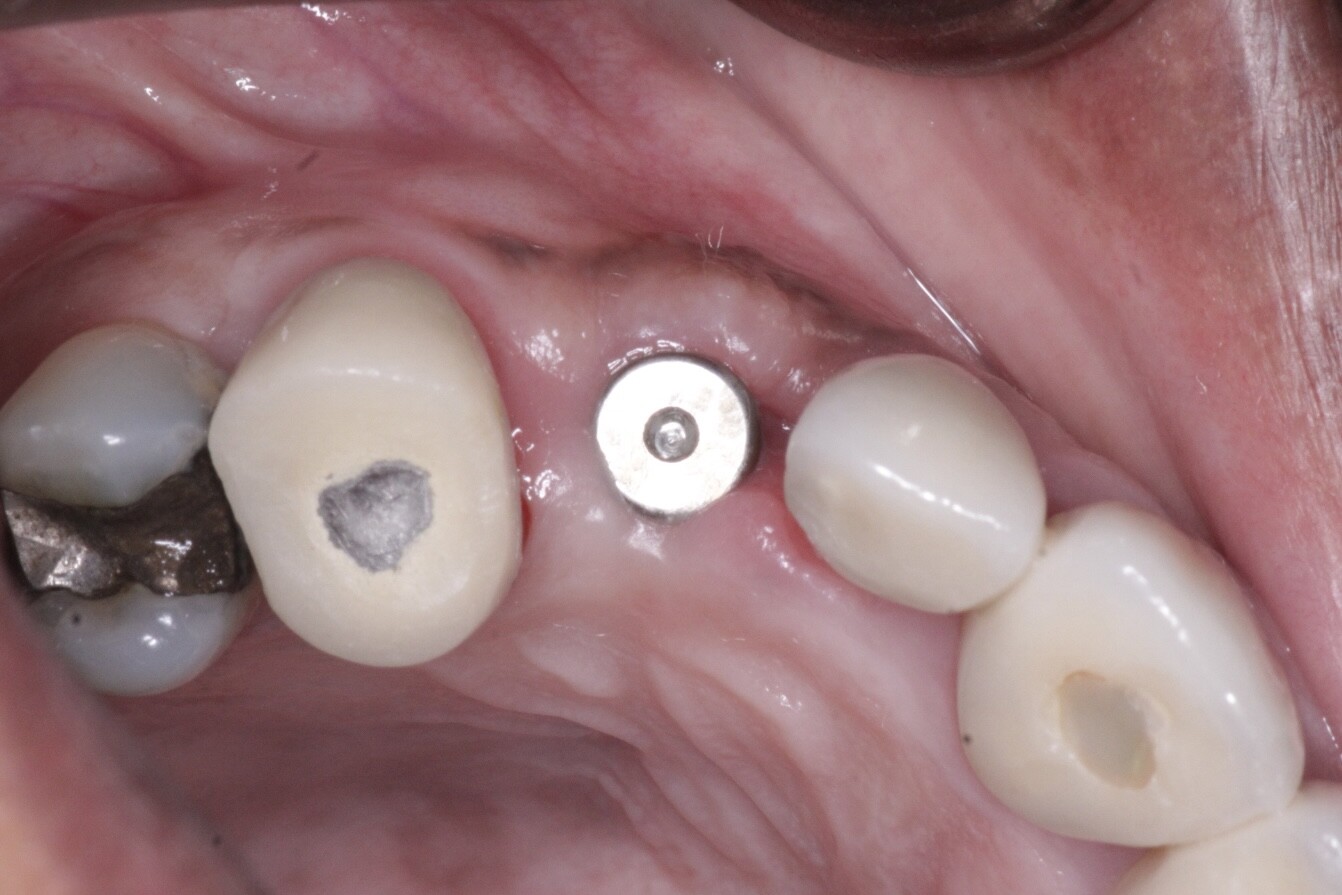
Just a few indications in my private Idaho. The biggest is in relation to the anterior aesthetic zone and concerns about risk of periosteal stripping and bone loss. On the other hand, if I have a big wide ridge in the mandible with gobs of height, I go flapless and don't use a guide either. So really it's kinda dependent on the situation. In my book, never say never, and never say always.
I would say, be very careful about the use of guides in the posterior quadrants. Always CHECK your vertical height to see if a tall burr will work. Been quasi-burned on that before. Lastly, on guided distal extention or edentulouse guided cases, ALWAYS use a guide that has been generated using a properly rendered CBCT for direct bone contact. Distal extention cases will have "wiggle room" that will make it hard to anchor precisely and get the proper orientation.