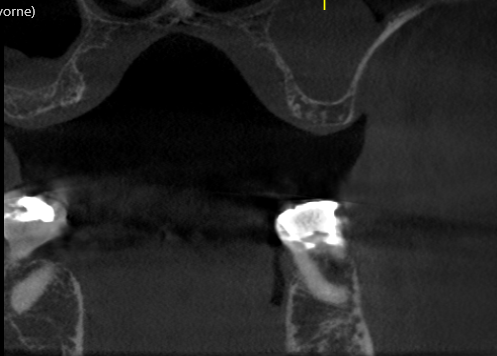
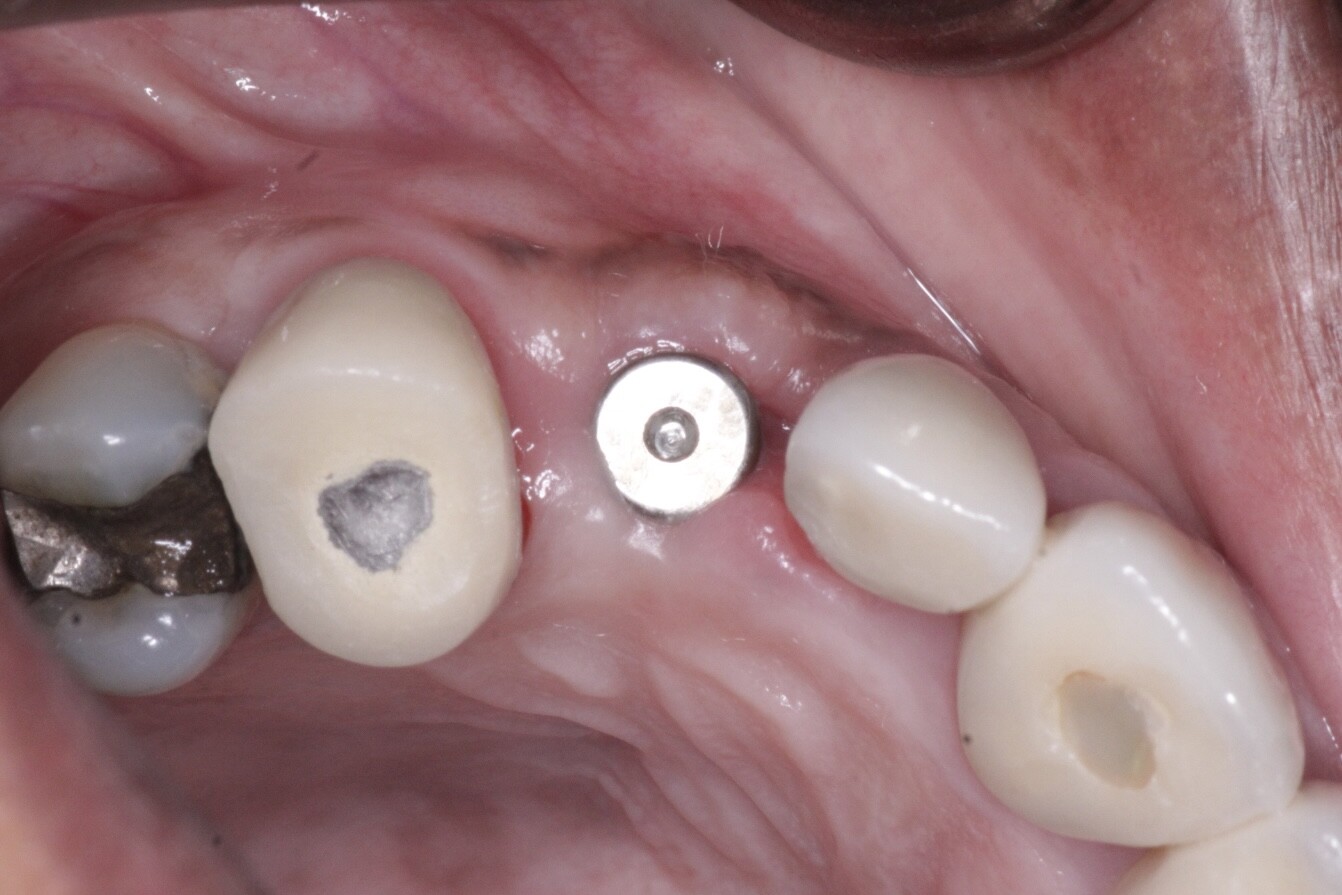
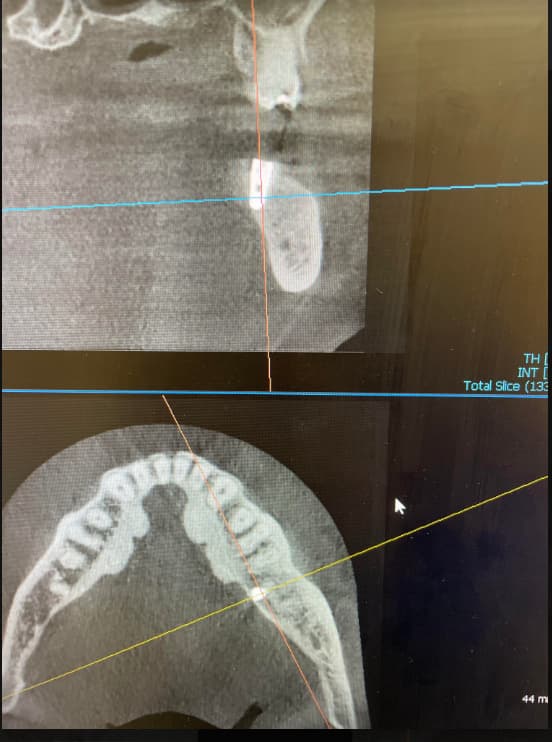
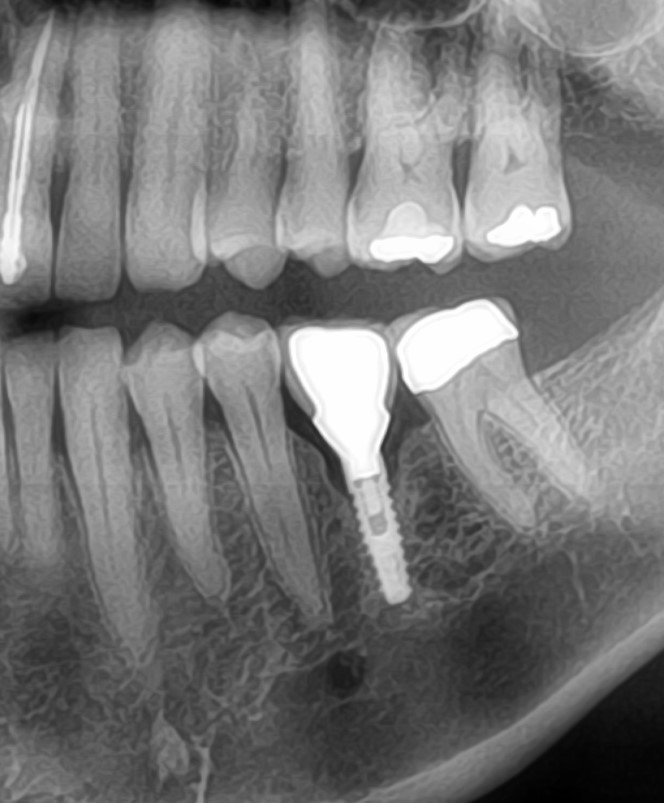
Larry, what you are asking is very difficult within the constraints of this website due to the time it would take for me to type up all I know. What I will do is give you a few basics and then urge you to go back to Dr McHorris's website and contact him to buy his book "A compilation of Papers" - which has all of what you need (in particular his article 'The condyle-Disc Dilemma from the the Journal of Gnathology Vol. 3, No.1, 1984. You may also look at attending one or more of Bill's workshops - his knowledge is amazing.
Anyway, you start by placing enough leafs between the patient's incisors until they no longer have posterior contact whilst biting in the retruded position. By doing so the only muscles contracting are the superior head of the lateral pterygoid (which is attached to the disc) and the anterior and middle fibers of temporalis. Without posterior proprioception, the remaining closure muscles masseter and internal pterygoid do not contract. What happens now is that the patient's habitual bite is being deprogrammed and the condyle will slowly move up towards the eminence. Very shortly the patient will let you know that they can feel their back teeth touching and at this time you remove the leaf guage add a few more leaves and continue as before ('forward and now back') - it is important to advise the patient that they are not to close their mouth at any time unless the leaf guage is in between the front teeth!!!!!. Continue with the therapy adding leafs as necessary until the patients bite appears to have stabilised and no further leafs are required to maintain an open space between the posterior teeth - Do not take a bite until the guage has been in the patients mouth for at least 5 min. It's worth spending a few secs explaining what has just happened. Pretty much all adult patients have a poor occlusion in which prematurities abound which results in the patient occluding in MIP 'out of CR' - that is the condyles are not fully seated with their disc assemblies against the eminence. So, when we use the leaf guage, the condyle and disc are in a way, forcibly seated against the eminence through the actions of temporalis and the s.head. of the lat ptery. As the seating progresses posterior contacts between the prematurities start to come into play but are then removed through the addition of more leafs. Eventually, the condyles find their way home the posterior contact remains open and a bite with beauty wax can be taken -WITH THE LEAF GUAGE STILL IN PLACE ( I use my DA to remove and replace the leaf guage at the bite stage. Only cusp tip indexing is required and so for some patients who had only minimal interferences, only a small space may exist between the posterior segments once the condyle is in CR, and so it may be necessary to add a few more leafs until you have the correct gap so that only cusp tip impressions are obtained. I should warn you that the leaf guage is also used in TMJ pain diagnosis and management and during the course of the therapy it it is quite common to cause transitory pain to the TMJs (managed with warm towels) with patients who unknowingly are bruxers and have a superior head of the lat pterygoid that is in a state of tetany (the isolation of the temporalis and the lat pterygoid will initially load the fatigued muscle and then allow it to relax - this is when the patient suddenly feels 'relie'). Mounting of the patients casts on the articulator with a face bow record will require approx 3-4mm of opening when mounting to accommodate the thickness of wax.
Larry, I have tried to give you a snapshot of how it works but I have left out a lot of detail. I urge you to contact Bill, get the compilation of papers and find out who is the closest member of the International Gnathology Academy and watch how its done. Gnathology members are incredibly knowledgable people who really enjoy spreading the message and mentoring others. It's amazing that such a piddly little device can so empower you in the operatory.
Hope this all helps. Regards John