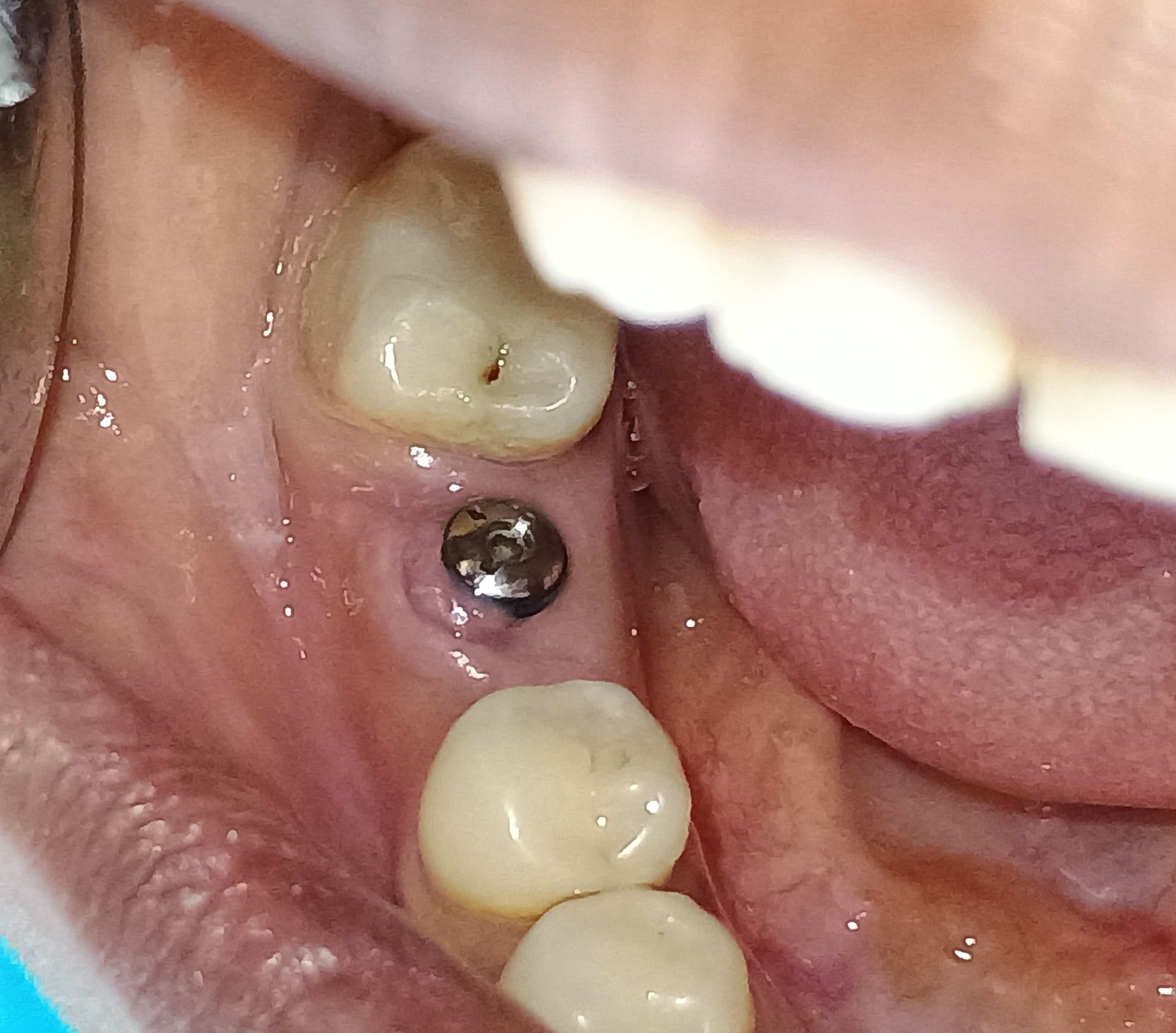
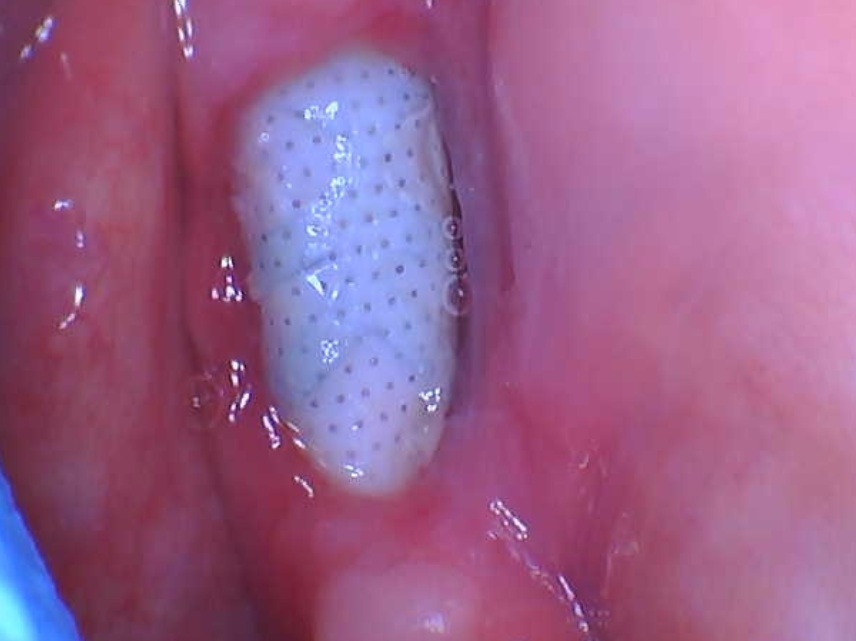
Post-Operative Infection after Sinus Lift: Causes?
Dr. A. asks:
I have had excellent success with direct sinus lifting using mineralized corticocancellous allograft, soaked in Ancef [cefazolin]. I also use a collagen membrane soaked in Ancef as well, and a membrane over the window prior to closure. The patient is put on a Augmentin 875mg , as well a Dexamethsone protocol, Sudafed, and Chlorohexidine rinse.
However I had a couple of cases recently, where the patient was healthy without systemic disease, with no allergies, where the surgery was uneventful. The patient returned two weeks post-operative and the surgical site looked great. Then at 3.5 to 4 weeks patient returns with a moderate size swelling in the upper side where the sinus lift was performed. Intraorally, everything is normal and incision lines are closed. Radiograph shows the graft still completely intact. Obviously an infection has occurred, however anyone know why, and what is the best course of treatment?