Suggestions for Bridge that Will Not Stay Cemented to Implants?
Dr. D. asks:
This 60-year old female complains that her bridge will not stay cemented on her implants.
The implants were placed three years ago. The bridge was re-cemented a number of times. She has recently re-cemented the bridge herself with superglue. She has a lower removable partial.
Recurrent decay exists under the crowns on 6, 11, and 22. She presents with generalized gingivitis. She states that she would be pleased if she could have a bridge that would stay cemented and a new partial.
Any suggestions?
Lower Anterior
Straight on Closed
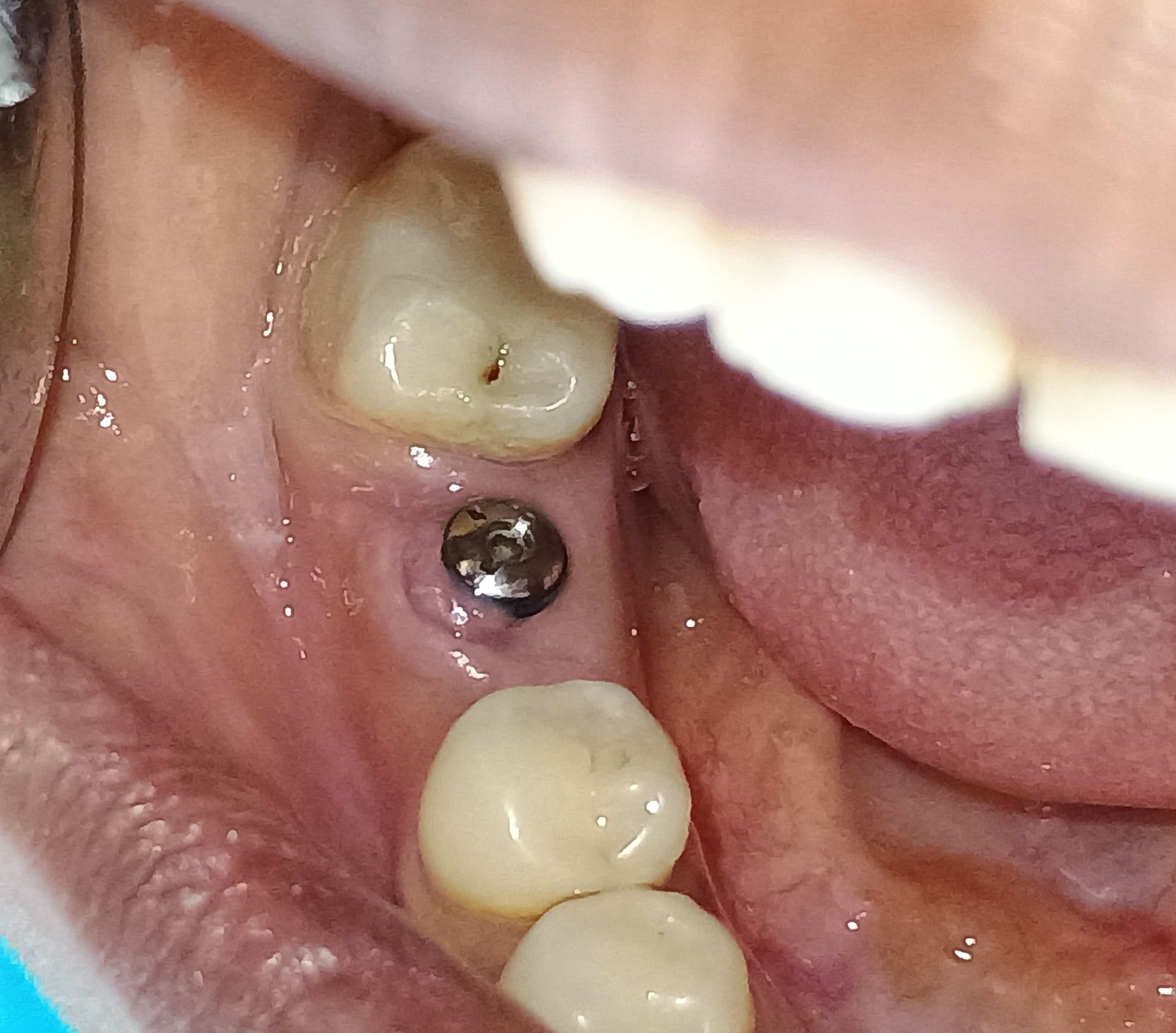
Right Occlusal
Left Occlusal
Pano
42 Comments on Suggestions for Bridge that Will Not Stay Cemented to Implants?
New comments are currently closed for this post.
Dr. Alex Zavyalov
2/19/2012
The first reason is that the crowns are wider that they should be. The second reason is the frontally localized mastication force. It’s surprising that implants are still in function. Therefore, it is absolutely necessary to make a lower partial denture to equalize mastication forces and prevent implants from overloading.
Rodgeru
2/19/2012
She has obviously lost vertical dimension, with occlusal parafunction destroying the cuspids and functional occlusal forces of four teeth stronger than the cement on two implants. Note that there are tremendous shear forces on that anterior bridge.. Conjecture without radiographs or CT scans may be inaccurate, but it would seem that mandibular block grafts with suitable mandibular implants/prostheses would help recapture the vertical, proper restoration of the cuspids (implants?), new FPD #7-10 with appropriate perio treatment and possible implants on #8 and #9.
Dr L
2/19/2012
One word- overload. Need to look at a lower partial or some fixed pros to help spread that load. Also possible bruxing? wouldnt be helping either.
carlos boudet
2/20/2012
The patient needs posterior support for the anterior occlusion.
You restore ir and give her a stable posterior occlusion and that should help protect the anterior bridge from excessive forces.
Since the bridge is already done, that is the necessary treatment, otherwise, adding an additional implant or two to the bridge would also be beneficial.
Good luck!
Richard Hughes, DDS, FAAI
2/20/2012
Carlos, you hit the nail on the head.
Antonio
2/21/2012
Dear Colleague, I suggest you to ask your technician to make 2 palatal screws to let the bridge stay in place. This is, in my opinion, the most practical and economical solution.
naser
2/21/2012
the pt masticate on the ant.segment overloading and rocking force cause the falling of the ant. bridge even if you super cement it .eventually the implants will fail. posterior reconstuction is the best solution which will distribute the force of mastication on verical direction rather than horizontal shear force on the ant. s
looflirpa
2/21/2012
You could roughen up the abutments or even perforate each one at some place above the screw to get a lock with the cement going through and through. But maybe the bridge coming loose is saving your implants from an even worse overloading fate.
Pankaj Narkhede, DDS; MDS
2/21/2012
She doesn't have posterior occlusion. She bites in the front teeth. Make partial to create a posterior occlusion. You may make a lower partial with attachment on the canines (until they hold:-).
The best cement I have used is infinity. BUT, create an occlusion first
SG
2/21/2012
I don't think the answer in this case is to figure out a way to make the cement more retentive....if you do this as is suggested by some of the above posters, and you don't address the loss of posterior F and F, then instead of the bridge coming off, you will see the implants fail. You know the saying, ".....something's gotta give".
SG
2/21/2012
I am also concerned about the fiery red appearance of the gingiva in both the maxilla and the mandible. If this is, in fact what the soft tissue looks like, and is not a result of poor photographic reproduction, then I wouldn't be so casually diagnosing this as "gingivitis". Even though this may not directly relate to your original concern re the maxillary anterior bridge repeatedly falling off, you may have a much more serious problem on your hands. I would definitely run a complete panel of systemic blood tests.
james butler
2/21/2012
lots of good advice, case is undersupported for forces expected. at the least, two more implants and a hard splint at night and when bruxing. posterior reconstruction looks difficult given posterior bone loss, all on four lower may solve a lot of problems!! 22-27 lost cause at the end of the day......
Rodgeru
2/21/2012
Carl Misch just gave a stunning presentation at the IOCI meeting advising against all-on-4 restorations due to the skewing of the success data and the fact that losing even one of the abutments results in a complete failure of the prosthesis. Various presenters make the case for bilateral block grafts and placement of implants in the mandibular region. Of course, not all patients will go for the ideal, but we should at least identify what the preferred treatment is. A lower RPD would suffer from the extensive bone loss, so an alternative is possibly an implant supported RPD on the mandible to effectively balance the posterior occlusion.
Robert Wolanski
2/21/2012
Overload and incomplete treatment (planning). Parafunction by design. Do not screw the bridge to the implants as you risk overloading them and loosing them as well.
Advise the patient the unseating of the bridge is actually a good thing, as it acts as a pressure relief valve, and a small price to pay.
PLD may help but you will be faced with retention issues and patient acceptance. The soft tissue support may not provide as much load distribution as you might hope for.
The answer lies in a larger snowshoe replicating the natural force distribution she has lost. This may require bone grafting (complex location) and many more implants. When you explain the costs to the patient it may help them realize what I alluded to earlier, the small price to pay of annual recementation.
Dr Teeth
2/21/2012
Occlusion imbalance. You are lucky that the cement failled, if you make the bridge more solid, you will loose the implants by overloading the bone. Even a good partial will not solve this, as it will move as bone lost continu, the pressure will be back to the front area in no time.
This case need a complete overall of the occlusion. If possible re-hab the lower arch with implants and crowns. Very drastic idea, but you can also remove all lower teeth, place 5-6 implants, do a fixed lower arch, place more implants on top, and do a proper re-hab of the occlusion. How good are the upper bridges ?
Alejandro Berg
2/21/2012
HI, I would say that this was a dissaster by plan. First you need posterior support and I mean real support with a real vertical dimension gain and stabilization, then you can think of re doing the bridge from the begining.
Dr Teeth
2/21/2012
7 answers in a few minutes ! All say the same things poor occlusion.
ttmillerjr
2/21/2012
It sounds like many of you missed the fact that the patient is wearing a lower partial. In any case those lower natural teeth are, indeed, overloading the upper anterior segment. Dr.D also told us that she has decay under three other crowns. If the patient doesn't want to spend a lot of money I would suggest transitioning to a removable upper. There are many different ways to do it. One option, assuming the perio condition is adequate, is to do root canals on 6 & 11 then place locator attachments on these teeth (section the bridges). You could make a metal based upper partial that fits over her current abutments 7 & 10 (may need some adjustments or new abuts) and is retained by the two locators on the canines. This will help redistribute the forces on more teeth and eliminate the caries problem under the bridge abutments.
I would tell her that the forces as they are now are pathologic ( she can probably understand this, as her bridge keeps coming off) and that it might have been good fortune (as someone said earlier) that the bridge came off instead of knocking the implants loose.
Of course there are countless options for restoring this case, let us know what you decide, it will be interesting to follow.
Dr. Mark Montana
2/21/2012
The comments posted are correct, the cement failure is due to an overload in the anterior segment. However, we should not diagnose parafunction based on the information provided; this patient suffers from anterior hyperfunction and posterior hypofunction or nonfunction. The wear to the lower anterior teeth is expected given that they do all the function and oppose a porcelain bridge; therefore both hyperfunction and abrasion exist. The cement failure is a warning sign and should not be remedied by moving to stronger cements or set-screws. Neither will change the patient's condition, namely lack of posterior support and their application may result in a catastrophic episode like screw or implant fracture. The addition of a distal-extension removable partial denture will not provide posterior support unless it opposes a complete denture, and even then it is often inadequate - see Combination Syndrome. The appropriate treatment is to provide a posterior fixed restoration, probably through a mandibular hybrid prosthesis.
gerald rudick
2/21/2012
Very good comments, this patient's problems started years ago.
Look at the abrasion to the remaining lower teeth as well the severely resorbed bilateral posterior ridges
The tissues as viewed in these photos show extreme inflammation which could be manifested due to systemic disease, poor oral hygiene, alcoholism,drug abuse, excessive tabaco,etc,
As repeatedly mentioned, if something is not done very soon to correct the occlusion, the implants will be lost as well....the loosening of the bridge is a good omen....sending a message to start a definitive treatment plan.
Gerald Rudick dds Montreal
John T
2/21/2012
Question for SG - Er, what's a "complete panel of systematic blood tests"?
SG
2/21/2012
In a nut shell, ask Pt's MD to help you rule out at a minimum diabetes, thyroid dysfunction and Vit D deficiency. There are standard tests that are also ordered including a cbc (complete blood cell count) and differential. I can get you a more complete list if you would like.
Rosemarie
2/22/2012
Can you please tell what complete blood work should be done before implants? I know I have a vitamin D deficiency. I am petrified about having implants but know I need to do something.
Thank you
SG
2/21/2012
I often wonder if whoever posted the case in these threads reads our responses and if s/he gets anything out of our conversations. If s/he is reading these comments, I find it hard to comprehend why s/he doesn't either respond to some of our queries or at least says something!!
Dr. Omar Olalde
2/21/2012
Overloaded. The patient has good luck that the bridge is decemented, otherwise she would loose both implants. I bet you that she doesn´t use the lower removable prostheses. And if she does, it doesn't restore the vertical dimension.
Robert Wolanski
2/21/2012
To SG haha.
It is true, I have also wondered why the person posts does not reply much, sometimes.
SG
2/21/2012
As the old saying goes" "inquiring minds want to know"...
Richard Hughes, DDS, FAAI
2/21/2012
All have made excellent comments. I have seen this situation walk into my office (several patients). It is difficult to help the patient understand about overload, occlusion etc, many times they do not want to pay for additional treatment. So, I let them walk, but with a written explanation. People have short and selective memory.
pirat
2/21/2012
guys...really? okay,she needs some posterior teeth but look at those abutments...mirror smooth...maybe you could vaseline them to make it stick even less. do you polish your crown preps like that? if overload was the sole problem don't ya think there'd already be some bone loss...it's not fallin off daily, so it's absorbing the brunt of the force say, 75% of the time. rough up the abutments and maybe put some retention grooves in 'em. then present your big dollar, long term plan...she'll have alot more confidence in you (read:your tx plan) after that thing's stayed in place for three months
Han Solo
2/22/2012
This practitioner must have skipped physics class.
adw
2/22/2012
Dr D ,
You cant go wrong if you follow the advice of the experts who have given you a solution to this case. To my colleagues who give of their time and considerable expertise to answer (albeit sometimes with acidic comments)and help their colleagues - I say well done.
JIM
2/22/2012
It's pretty obvious it's an occlusion issue as the lower anteriors have supra erupted and the hyper occlusion is evident by the recurrent decay on the facial margin of the crown on #22 as well as the wear on the incisal of all the lowers. Apparently, while she does have a lower partial denture, I agree with the person above who said she probably does not wear it ( who really likes their dentures?) Question is if there is any sort of compromise here? I agree the abutments look way too smooth. What if a screw-down prosthesis made with acrylic and denture teeth is fabricated as an interim prosthesis. The lingual acrylic and denture teeth will be more forgiving on the occlusion. Thoughts?
Alex BLR
2/22/2012
Why doktor start this treatment only in front? may be, it was better to motivate patient for posterior teeth, or dont start at all? Sorry for my poor english.
raghav
2/22/2012
its good bridge is coming out rather than implants. posterior load balance is mandatory ,relieving anteriors out of excessive load..luck's favouring all of us many times actally
SG
2/22/2012
Luck favors the prepared mind....
Dr Samir Nayyar
2/23/2012
Hello
Very good comments made by very experienced docs. I think the person posting them should respect the time & knowledge that has been shared by the docs. It depends on the reader whether to accept the advice or not. Also they should post the treatment they do and their outcome.
The patient may be wearing the lower RPD during the day time but not at night. If patient is ready then first of all give fixed implants in the lower posterior region or give implant supported RPD.
Also give TMJ appliance or a night guard to be worn full time for 3-6 months atleast and then at night.
Baker vinci
2/23/2012
I'm not going to comment on the cement question, but the responses deserve some reply. First , in my opinion , she needs to be cleaned up. This is not photographic artifact and secondly just as the "bosker" or tmi system went down the drain, your great philosopher is on to something , when he suggest the "all on four" , is a poor design. When one part fails, the whole thing is a wash, until the weak link is "patched up". Bv
mamos
2/25/2012
As everyone has stated above, she has lost VD .A new RPD to restore her VD (or changing the acrylic teeth of her existing lower RPD to raise the bite ) should take away the destructive bite forces from the anterior teeth.Secondly the abutments look non retentive.After changing the lower RPD, I would remove the abutments, take another impression and make the lab prep the abutments in flat planes to make them more retentive and make a new bridge.Good luck!
Salim Hazim
2/29/2012
chenging the overloading area from anterior to posterior will shift the distruction to posterior mandoibular residual rigde which already highly resobed, and after while we will loose what we gut by ingreasing vertical dimention due to more bone resorption of posterior manbible under unstable overloaded removable partial denture. as it appear in the radiogragh the bone high is diminshed and contraindicate the insertion of long implant to support fixed partial denture in posterior mandibular rigion, the insertion of short implant and fabrication of removable partial overdenture looklike the wise solution.
Dr Sanjay Jamdade
2/27/2012
With and Occlusion like that what do you expect? Occlusion is the key my friend. Many a poor retention crowns will stay in place simply because the occlusion is favourable. Enough has already been said in thte above posts. Heed their advice. Get those posterios in place and see how the anterior retention improves! Best wishes!
Dr. Shresht
2/29/2012
the problem area for sure is the mandibular denture....the complete occlusal load seems to lie on the anterior segment alone. The other crowns also appear quite bulky and definitely need replacement. Radio- graphically the implants appear fine and decementation is rather preventing the failure of the implants. Plz do check out on the anterior guidance aspect while re-planning.
Dr. D
3/24/2012
Thanks for all of your suggestions. I will definitely take them into consideration when treating this patient.