Implants Failing Badly: Suggestions?
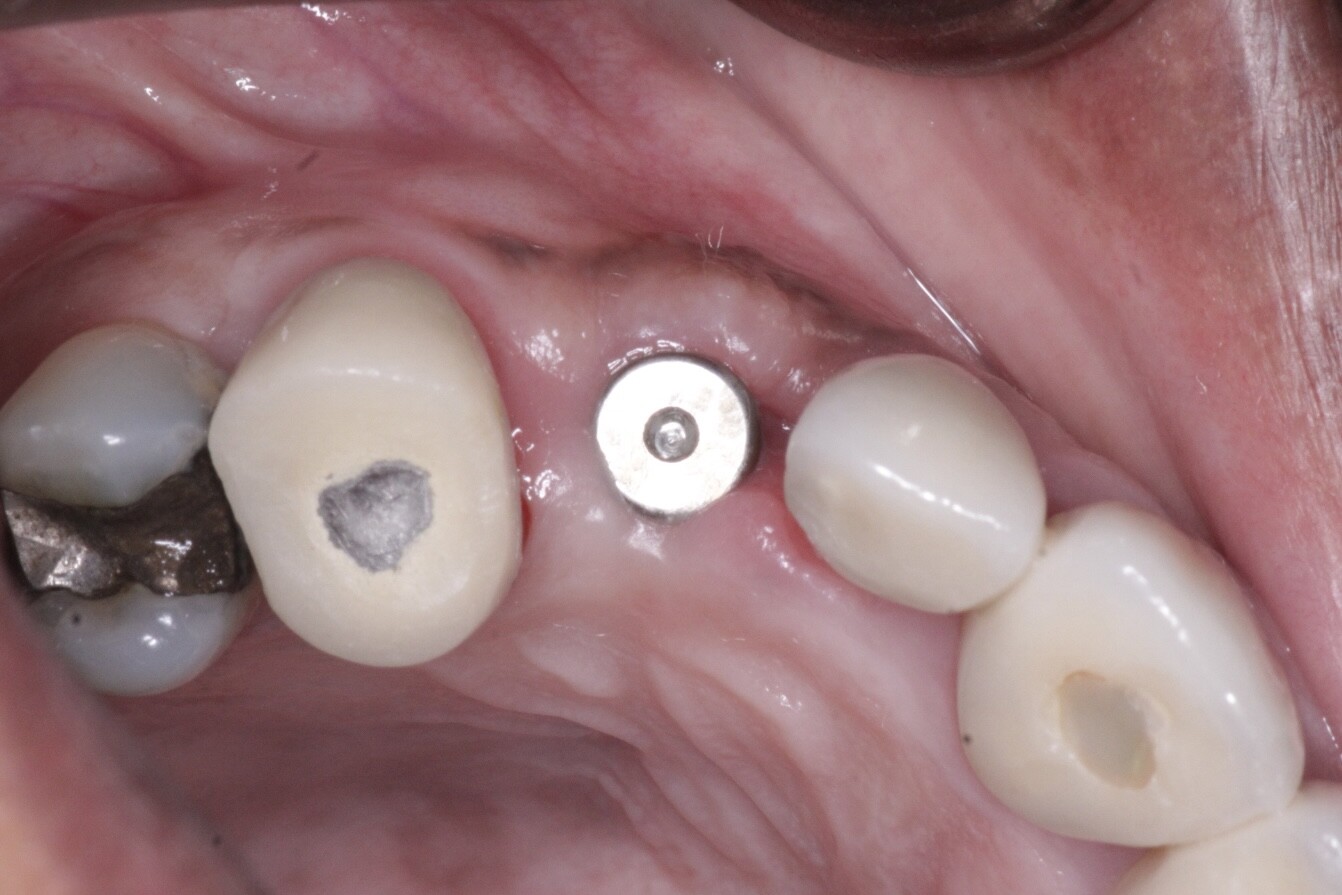
This is a full arch case in which the patient had been edentulous for many years. He has some cardiac problems but no other health issues. He is on a calcium channel blocker and I wonder if anyone has any information on those medications interfering with osseous homeostasis. The implants were placed 2 years ago. The restoration is screw retained. I was the surgeon. The restorative dentist chose to segment the restoration into three segments for ease of restoration. The patient reported irritation around the upper left second bicuspid 6 months ago. I noted bone loss and did a flap/curettage with a stem cell graft. The area responded well. The patient called because his “bridge was loose”.
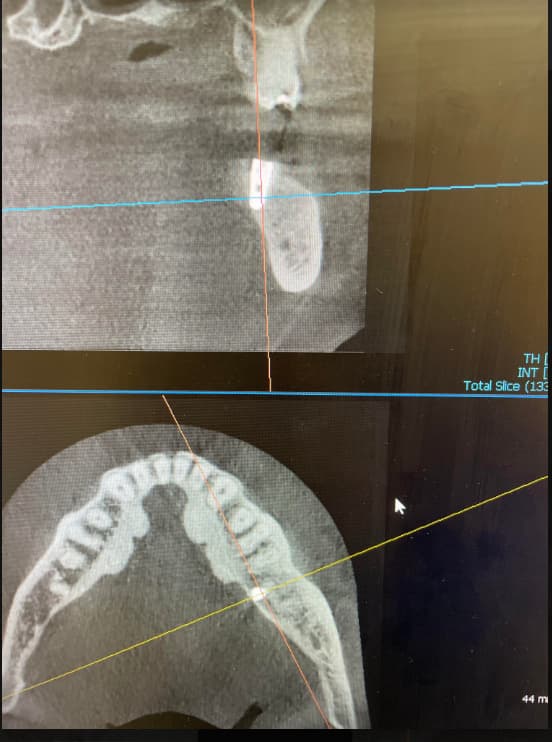
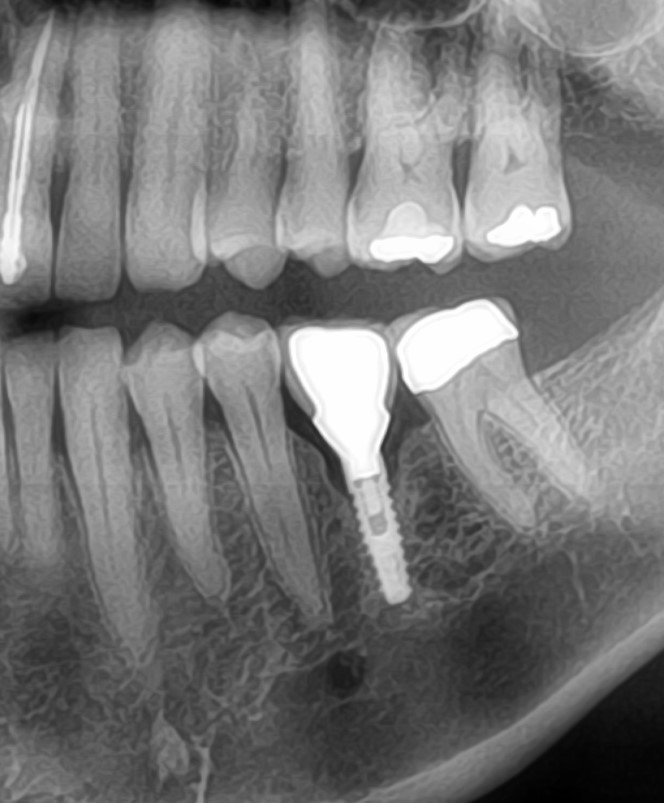
Examination revealed severe bone loss in all four quadrants including the lower molar implants. The upper left quadrant was removed. As you can see bone loss is horizontal and severe. I can remove all the implants, do bilateral sinus grafts, vertical onlay grafts and/or guided bone regeneration and create new ridges for new implants. The problem is this will happen all over again if I don’t find the cause. I must admit I am clueless (of course my wife has been saying that about me for years). Any ideas, suggestions?
 Current Pano
Current Pano