Discovered fistula during implant restoration: suggestions?
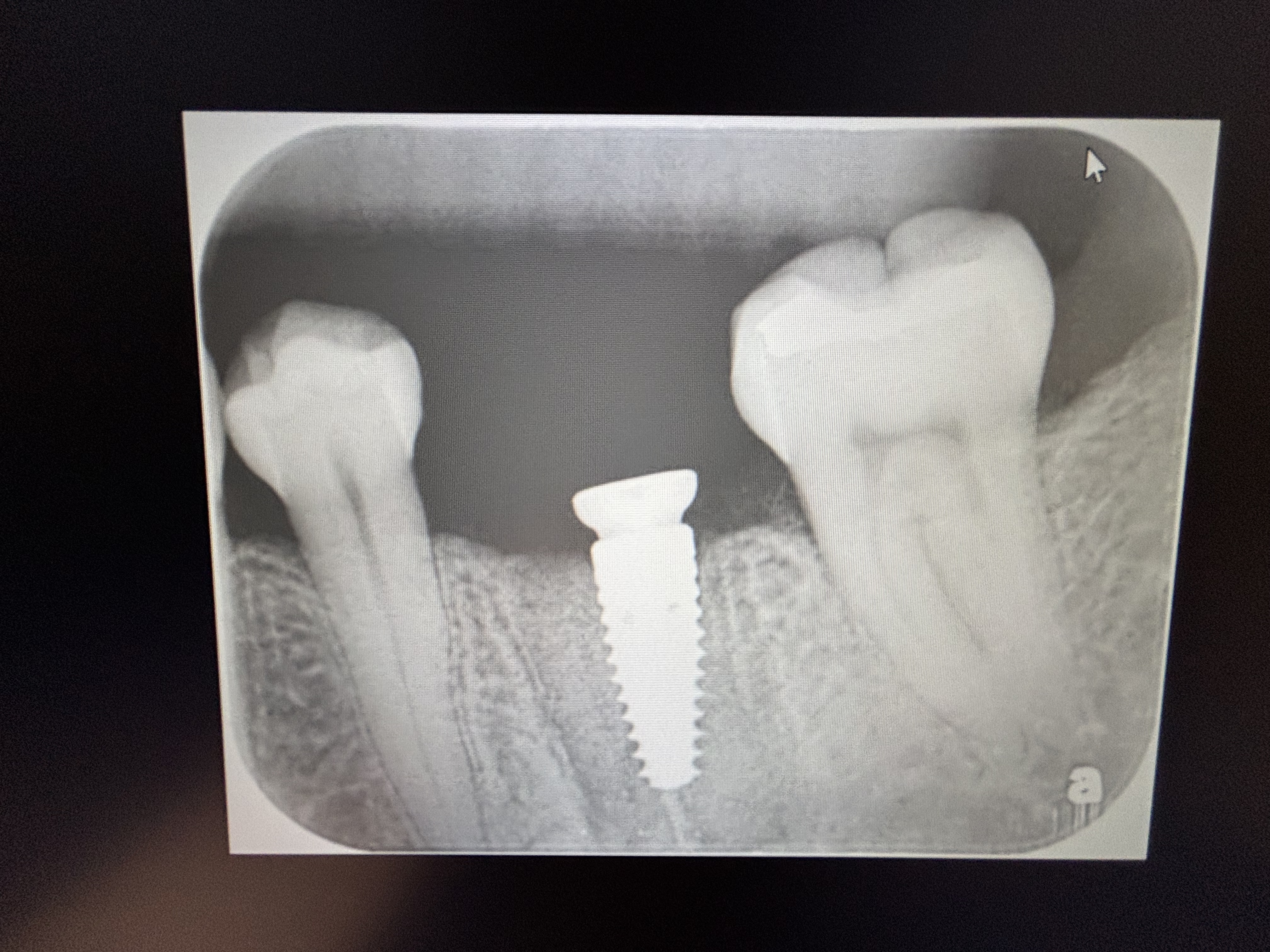
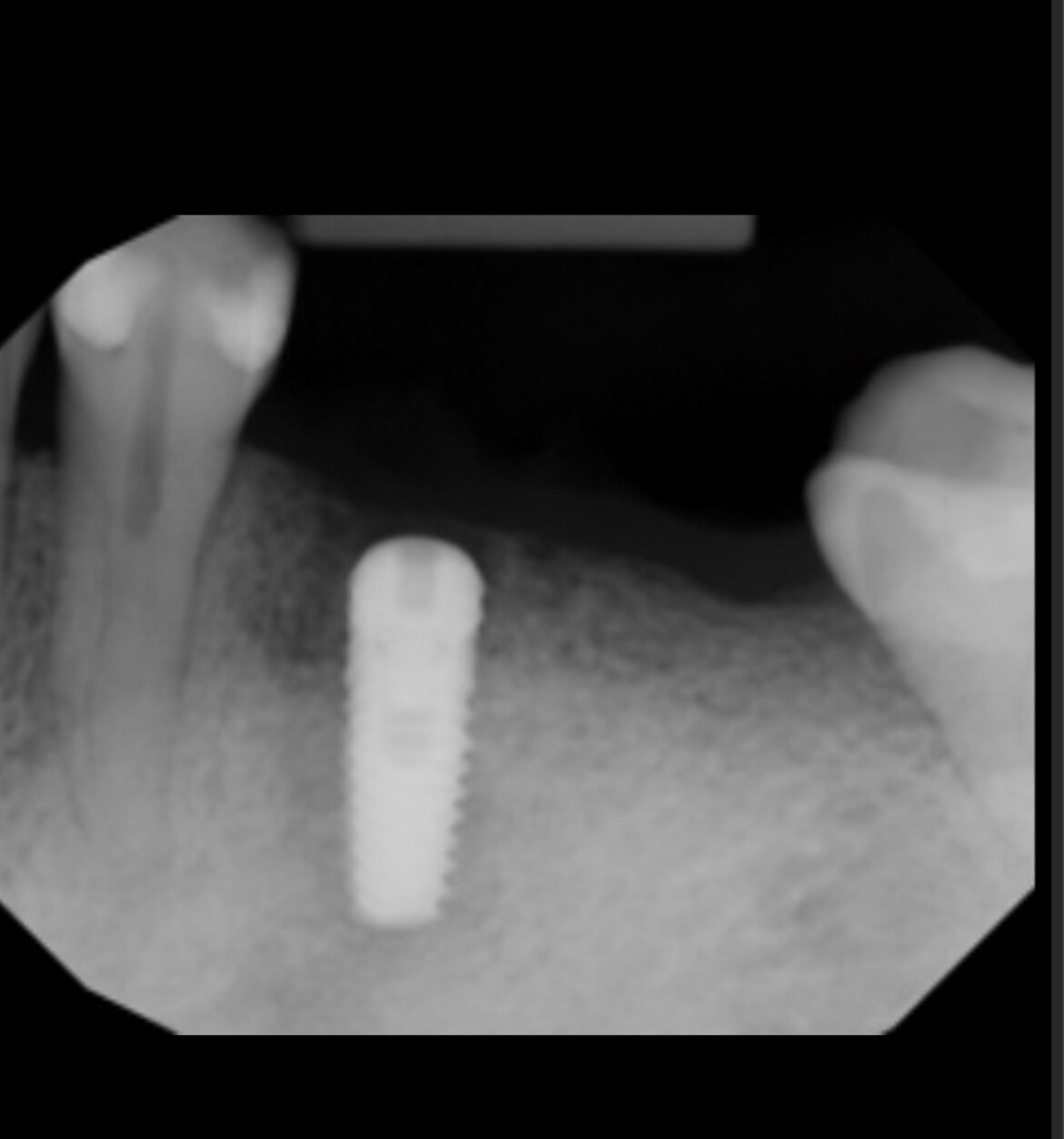
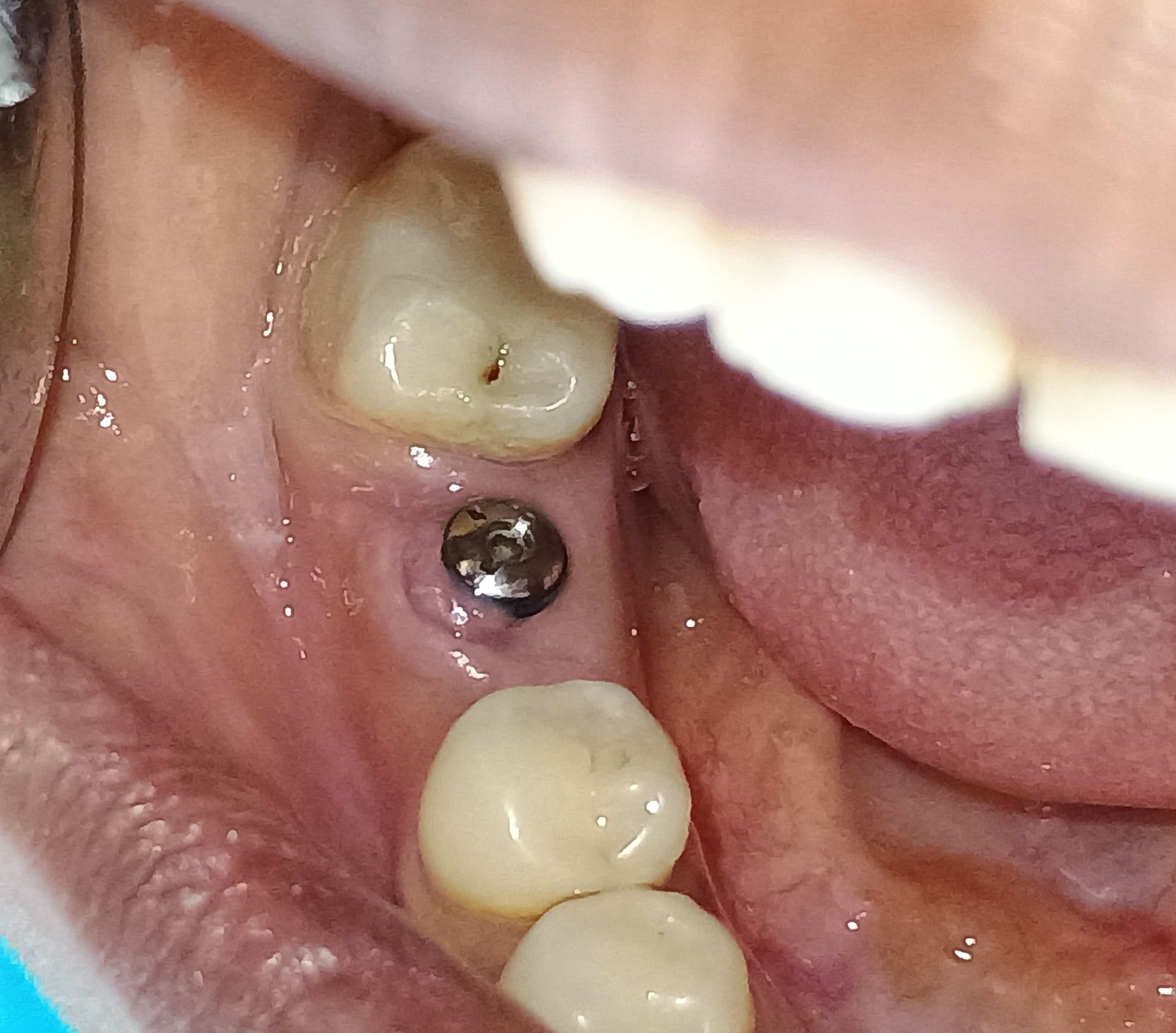
Patient presented in July 2016 with long standing pain and infection in the area of tooth #5. I extracted the tooth in September 2016 and placed an implant that day. I started to restore the implant yesterday and I discovered a fistula. I traced it with a gutta percha point (see pa). I probed the fistula, but could not sound to the implant. I placed the patient on clindamycin 1,200 mg/day and seated the final restoration and hand tightened the screw only. Patient called today in pain and says the tooth in front of the implant is numb. Any ideas on what’s going on? Any suggestions?
41 Comments on Discovered fistula during implant restoration: suggestions?
New comments are currently closed for this post.
grwez
5/11/2017
As a follow up to my post, the patient came in yesterday and the pain and numbness turned out to be a slightly tight contact from the new crown. But the question still remains about the fistula.
doc
5/11/2017
that's avoiding the fact the patient needs further care which is at least a flap to inspect the defect of a draining infection. And "new crown" or not, it's likely to soon be the "old crown". That's what fistula's are--not mystery, but infection.
grwez
5/11/2017
I agree it needs additional care. The implant was buried for months, asymptomatic, and at the seat appt. the fistula appeared
For me the question is what options do I have available? Should I do a semi lunar type of flap, inspect and repair with the implant in place. What types of materials do you like to use to treat the defect. I have my own ideas. I am looking for constructive suggestions. THANK YOU.
Dr mark bishara
5/11/2017
It looks like you have had a buccal plate fenestration without realizing it.get a CBCT.
Dr. Steven Kollander
5/11/2017
Remove implant, wait two months, replace (BTW, clinda 1200mg may lead to nasty GI sequelae.....should limit it to max 900 mg/day).
doc
5/11/2017
Despite any CBCT notions or other proposed interdictions into an obviously failed implant, this is what CBCT combined with open surgery is designed for. The fistula is possibly not "new" but present prior to extraction, a buccal plate perf longstanding before the extraction from a failed endo/cracked tooth, or whatever. Now, in a blind surgery, the buccal plate can't be inspected, let alone grafted. So a good guess is the procedure was done "blind" (ie with only extraction, curettage, and no open visualization of the socket, the buccal plate or anything else). So without CBCT to know how fragile the buccal plate was prior to surgery (an all too often finding) warranting careful extraction (piezosurgical prep) as well as augmentation grafting, and without knowing if there was either compromise of the plate with extraction OR an existing preextraction defect, this case was destined to fail, as it likely has. Remove, graft, wait at least 6 months, redo.
doc
5/11/2017
Dear Doc,
I'm not sure where you get your info, but the max dose of clindamycin is 2700 mg/day. I grant this is for more serious infections, but as a surgeon, the dose you advocate is but a "whiff"--and that for a BACTERIOSTATIC, not bacteriocidal drug. Simply put, the dose mentioned (in the appropriate patient), virtually NEVER causes "nasty" GI sequelae, and this misinformation is what leads to avoidance of one valuable drug. Stick to dentistry.
grwez
5/11/2017
Maybe your cbct is better than mine but in my experience there is no guarantee that a CBCT shows every fistula or defect.
Leal
5/12/2017
Actually you can go up to close to 5g/day (4,8g specifically) for serious infections.
Marcus
5/17/2017
Max dose of clinda is 450 mg qid. Is there data that shows increase in GI issues with higher doses? I find there are patients that can be selectively intolerant of clindamycin regardless of the dose. Three hundred mg Q6h is an appropriate dose to treat an active infection.
Notwithstanding, after uncovering likely there was introduction of bugs straight down the non-osseointegrated threads resulting in colonization of the threads. I think in the patient's best interests either remove the implant, graft and redo OR open the site, debride and clean the implant threads mechanically and/or chemically (ideally both), graft with GBR and wait before spending their money on a crown.
Dr. Steven Kollander
5/11/2017
Dear Doc,
We are asked not to be obnoxious in our comments but you obviously have not paid attention to that request. Giving 2700mg /day of clindamycin? Three tabs tid? Where did you get your info? I guess that your spectacular practice administers I.V. clinda. Very impressed. Stick to paddle ball.
Oral:
Serious infection: 150 to 300 mg orally every 6 hours
More severe infection: 300 to 450 mg orally every 6 hours
Parenteral:
Serious infection: 600 to 1,200 mg via IV infusion or IM injection per day, in 2 to 4 equally divided doses
Severe infection: 1,200 to 2,700 mg via IV infusion or IM injection per day, in 2 to 4 equally divided doses
More severe infection: Up to 4,800 mg via IV infusion per day
Mark Bornfeld DDS
5/12/2017
Gentlemen,
Despite the very real risk of pseudomembranous colitis conferred by a number of different antibiotics (clindamycin, cephalosporins, fluoroquinolones, and even the old standard, penicillin and its iterations), you're not focusing on the real issue: whether the benefits of antimicrobials outweigh the risks in the current antibiotic stewardship environment.
Any infectious disease specialist will tell you that the fundamental approach to an infection should almost always be source control. You don't treat an infected IV line by pumping antibiotics through it; you remove the infected line.
Dentists need to take a more holistic view of how our therapies affect a patient's health beyond the scope of our narrow discipline. This is particularly the case when the payoff is only the temporary comfort of seeing a fistula close for a few weeks.
Dr. Steven Kollander
5/12/2017
excellent point
Marcus
5/17/2017
Ya but ID docs commonly agree to infected implant microbial infinite suppression with antibiotics. However this is in the context of a damned if you do and damned if you don't scenario (e.g. If you take the hip replacement out there is no option for another). This situation obviously does not fulfill that test. I have yet - after a couple thousand implants seen one case with a fistula get magically cured by antibiotics. The place for antibiotics here would be straight before re-surgery to suppress the bugs as much as possible, clean the implant, place bone and pray.
adil albaghdadi
5/11/2017
This is most likely caused by infection due to dehiscence of the buccal wall which was initially undetected or very thin with infected socket. if the implant is integrated and the dehiscence is less than 3 mm to the platform of the implant should be treated as an ailing implant with prep of the implant surface and bone graft with membrane after the removal of the crown and place a cover screw for 3-4 months. good antibiotic coverage like Vibramycin 200mg/day. hope the defect small. good luck
grwez
5/11/2017
Thank you for the constructive suggestion. Seeing as the defect is well below the "attachment" of the implant , do you feel I am being too risky laying a semi lunar style flap apical to the attachment and attempting to repair it that way? What is your preference of materials in treating this type of defect? THANK YOU
adil albaghdadi
5/12/2017
The flap I would lay is two sided and the vertical incision goes distal to #4 , clean the implant threads apply citric acid or tetracycline paste wash and pack the bone and cover with absorbable membrane 15x20 horizontal with tacks if you have them. small size allograft 50/50 corticocancellous would be a good choice.
Joe Nolan
5/11/2017
grwez doesn't need the needle , give the guy a break ! He had the guts to show his problem, so putting him down is not on.
Why condemn the patient to implant loss, when there is every possibility that - as doc himself said in his initial post, in fairness - possibly lifting a flap - cleaning the area, place some ethoss, cover it up, antibiotics, see how it goes....there's nothing to lose and everything to gain.
At this stage I would have refunded 100% costs and had the patient rooting for me...
FS , DMD
5/11/2017
There is one valuable little bit of info that you didn't provide, and that is whether or not the implant was torque tested. I suspect that it was not, nor would it pass, if it was. Regardless, I cannot justify placing the final restoration with an obvious fistula present, that clearly is associated with the implant. Don't need gutta percha to see that. You really only have one option here and that is an open flap procedure. I agree with doc's comments above, you probably have a buccal plate perforation, with a failed implant.
One final remark, here. Antibiotics aren't going to eliminate a fistula, regardless of dose or class. First principal of dealing with odontogenic ( or related) infections is to find and eliminate the source of infection. Antibiotics are useful as adjunctive treatment for minimizing fascial space involvement of the infection, but they aren't to be prescribed as sole treatment. Doing so, will just lead to antibiotic resistance. Prescribing antibiotics without documenting (and treating) the source of infection is not good practice.
grwez
5/11/2017
The placement of the implant restoration was done because the fistula did not appear clinically till the seat appointment and there is no harm in doing so as a temporary measure. For me the question is what options do I have available? Should I do a semi lunar type of flap, inspect and repair with the implant in place. What types of materials do you like to use to treat the defect. I have my own ideas. I am looking for constructive suggestions. THANK YOU.
Bob Aron
5/11/2017
Thoughts on immediate implant placement in failed endo?
grwez
5/11/2017
Yes , maybe I was a bit aggressive but when I inspected the area I felt the area looked good enough to place the implant. ...Hindsight my friend....
Amir Mostofi
5/11/2017
1) I assume the implant is fairly good integrated and when you did screw the crown to a torque of 35 Ncm.
2) You can raise a flap and clean the area where the fistula and fenestration is and wait and see if the infection goes away or not.
3) you should not use any bone graft material or membrane when placing the flap back. The bone graft material absolutely does not work with infection in the site.
4) If after a few months if you are lucky and the infection in the site disappear then you have the opportunity to raise a second flap and do some bone augmentation in the fenestrated area.
5) Considering all the above options I think that it is unlikely that the infection clears just by raising a flap and cleaning the site.
6) I think the most likely outcome will be to remove the implant and perhaps to place a second implant later.
Branimir Karmakov
5/12/2017
If I were you I would make a triangular flap in this case. After observing the problem the flap can be extended if needed. Clean bone, implant and fistula. Then make the place bleed, don't leave it dry. Place back​ the flap. Don't bother if blood comes out through the fistula. I suppose that the problem is in the marginal part of the implant. The implant is quite long so integration is enough.
Dr. Bob
5/12/2017
If a cover screw is not completely seated into the implant body at the placement surgery a fistula can appear after some time passes. It could take weeks or a few months before it is seen. The cover screw may seem to be seated and tight if a little tissue is trapped under it. Open a flap as if you had a defect on the facial aspect of the implant that needed repair. Start from the junction of the gingival attachment on the adjacent teeth and the facial over the implant. You will be able to see what the problem is and correct it. Is the fistula blind? It may just be a short healed tract lined with epithelium similar to an ear ring hole. Is there any drainage?
grwez
5/12/2017
I did not post the pa of the gp point I placed because it was inconclusive...I did probe the fistula and it seemed to go nowhere. As far as I could tell I could not feel the implant at all. This is one of the reasons I posted because I am not sure of what I have. I have never heard of a "blind" fistula. Assuming you are right, how does one treat it? THANKS
Dr Bob
5/13/2017
If the source of infection was eliminated at the initial placement surgery or when second stage surgery was done the deeper tissue then could heal. The remaining fistulous tract over time could have been lined with epithelial cells. This would prevent complete closure of the tract leaving something like a narrow invagination that no longer communicates with an infection deeper in the tissue. I see this on occasion with re-treatment of failed endodontics. When the tract is short and has a definite "blind" termination and there is no drainage I do not treat it unless the patient requests it. However, if there is any doubt that it is healed and that no infection remains, I will open a full thickness flap to confirm that the site is healed.
The flap should be large enough to do corrective surgery if needed. The remaining tract can be closed by removing the epithelial lining. A periodontal curette or a large barbed broach will work. Just because you can not pass gutta percha through the tract into an infected site does not assure that there is no infection. The cost of leaving an infection untreated is to great.
DrG
5/12/2017
I see the main question you are really asking is in regard to flap design. Let me clear that up for you.
Without a CBCT it is impossible to tell you what flap design would work best.
If this is a small Apical perforation and the implant ends in soft tissue then no flap will help.
If this is a long buccal fenestration then a semi lunar flap will miss the coronal portion that needs to be detoxification and grafting.
Get a good 3D image for us and we should be able to help you know what to do.
If you don't have access to a CBCT then anticipate a full buccal and palatal flap, grafting, gtr and burying the implant. Or just take it out wait for healing and start again.
Aziz Amro
5/12/2017
Dear
We would like to find out what is the main cause of the problem.
I think this is one of disadvantage of immediate implant placement.
Rob D
5/12/2017
First step- place 35 size gutta percha into the fistula and push it until resistance is felt. Take radiograph to trace the infection origin. The source may not be the implant? If it is the implant, you can now plan appropriately. Plan your flap design based upon the amount of buccal bone present. Determine your goal (therapy) based upon the size of the lesion as well. Your diagnosis determines all of this.
Good luck.
rsdds
5/12/2017
without a cbct its all speculation talk. How do you know if this implant is in bone this area seems relatively easy but it does have a palatal angulation most of the times and this is a very long implant, you don't see fistulas that often with implants if you place them into bone.
Elijah Arrington III
5/12/2017
Do a vertical releasing flap posterior and anterior to the implant. Keep the base wide of course. Include the teeth if u want be careful of the papilla if u decide to include a tooth. Raise the flap into nonkeratinize or just enough to see full defect. Currette the heck out of the cystic lesion that you will fine. Curaterize it if u have one. There should be no soft tissue left in the defect. Clean implant with citric acid scrub. Perforate the bone with 557 bur regraft with collagen membrane and graft materials
Add Metronidazole to graft. Undermine flap of course to get primary closure. Resuture; don't worry about a scar. You are a surgeon save the implant. If u find that the implant torques out then just remove it...and still remove lesion...and follow above info...Get an Ellman cautuery machine 4Mhz and use versah burs....
I graft with a Calcium Hydroxide, DFDB xenograft,and Metronidazole Mix BTW. Hope this helps...#weAREall brothers&sisters#BlessGOD
Elijah Arrington III
5/12/2017
Cont...Remove the temp as well to allow for proper healing and to gain primary closure.u can put it back...in 3wks...OR if they have to have one u make can make a temp with a wax up on a model..hand putty pvs copy it and then place copy on edentulous area filled with temp material...lubricate sutures prior. This will hold temp in via mechanical retention..because it will be held in by adjacent teeth...trim accordingly...u will have to cut temp out with bur when ready after area heals or when u are ready to take perm impression BTW. Hope it helps.....
FS, DMD
5/12/2017
Given the new information regarding when the fistula appeared, here is how I would manage:
1. Take the crown and abutment off, torgue test the implant. If it is stable at 35nCm, put cover screw back on and be certain that cover screw is firmly seated. Proceed to step 2.
2. Place Atridox in the sulcus around the marginal aspect of the implant. Discontinue systemic antibiotics. They have no role here. Place the patient on Peridex per Atridox protocol.
3. Re-eval in 2 weeks. Fistula most likely will be gone. Start back over with seating of abutment.
Note: If implant is mobile when you torque test it, proceed to open flap procedure, replace implant and graft accordingly.
Peter Fairbairn
5/12/2017
Yes late to party , but my 2 cents , could be non indexed abutment fit ... hence bacteria .. depends on system ....
or a chip of root or bone in the site ... happened to me last weeks ...
Peter
Dobs
5/12/2017
I have just reviewed this. The fistula appears to be at the level of the apex of the endo treated tooth. There is probably a bony deflect of the labial plate. It is also possible that the curettage at the time of extraction left bacterial contaminated material in the osteotomy site. The Implant is compromised. Clindamycin is not the panacea that we once thought it was. Check with the ÃD service in your city. In my city 70% of all Oral infections have resistance to it. Most of the organisms in a fistula are mixed and in most environments there will be some resistance. Torque test the Implant. If it is stable, then it is reasonable to try to do a salvage procedure. Put on a cover screw. Then design your flap in such a way that your flap margins will be on intact bone. You need to have a wide base to your flap. Wash out the deflect with 500 to 1000 cc of Bacitracin solution. Make sure that you remove all necrotic soft tissue and bone. Pack the deflect with your bone of choice and use a membrane. I use Snoasis in this case. Use a fine - 5-0 or 6-0 non resorbaable suture - Proline. Cover with antibiotics for 7 days and offer a 50 50 chance for survival. You should not image this preop to see where the bony margins are.
Robert J Miller
5/12/2017
Can you probe to the level of the fistula? The photograph you posted indicates that infection has reached the sulcus. If you cannot probe to the level of the fistula, the likely diagnosis is a fenestration of the facial plate. If the alveolar mucosa is now in direct contact with the implant threads, NO amount of antibiotics will clear this up. This is a trauma related inflammatory response from tissue moving over the roughened surface. The only treatment then is open flap debridement and grafting of the defect.
Mikey E. Calderon
5/13/2017
As long as you get primary fixation , GRAFT and close it up.
#implantmike
5/13/2017
Hey Bob, it's Mikey. Good direction. Is this case still being discussed or has it been determined what was done and what should be done. We all know the obvious but what was the end treatment here.
Robert Miller
5/14/2017
Hey Mikey; no indication it's been treated already. I've opened many of these cases through the years. Virtually all of them were fenestration defects and just needed to be grafted. The toughest part of the procedure, however, is complete debridment of the implant surface, especially if the soft tissue defect has expanded to the palatial side. This is where ablative lasers, with side firing tips, really shine through.
ez
6/6/2017
As a follow up here's what went down. Flapped and found a buccal fenestration , explanted the implant and bone grafted. So far the patient is doing well.
Thank you all for you input.