Flapless guided implant: Will this fail?
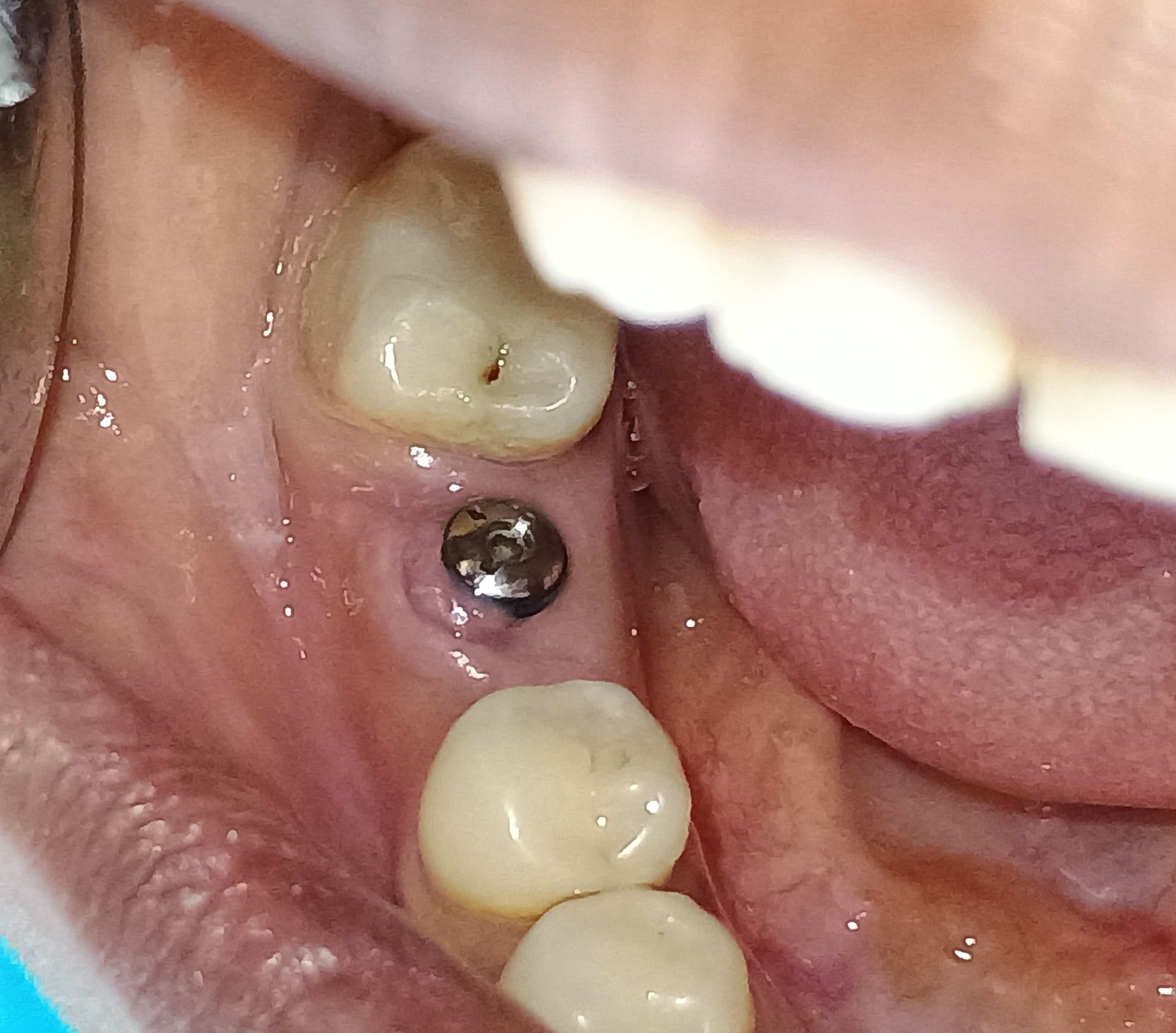
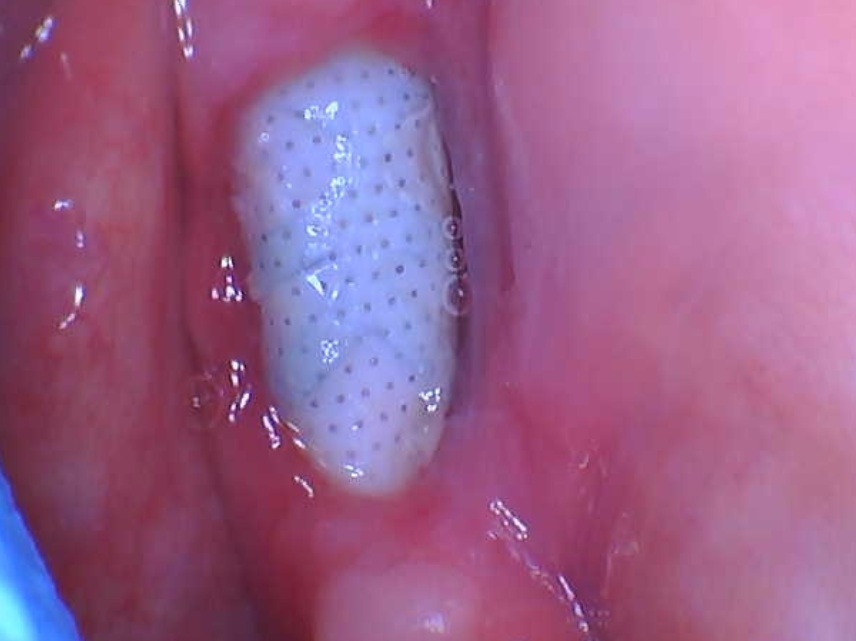
I placed my first flapless guided implant a couple of weeks ago. I am kicking myself at the moment that I didn’t just lay a flap and do it freehand. Access was difficult and it was also difficult maintaining the guide in position. As a result, osteotomy probably overprepped in the coronal aspect. Insert torque I feel was probably too high at 60ncm – I panicked a bit as felt the implant was not seating fully through the guide. First PA is directly after insert. Second PA is with healing abutment 2 weeks post op. Patient has no pain or symptoms, and appears normal clinically, but I am concerned about the crestal bone loss on the mesial aspect. Opinions would be appreciated.


49 Comments on Flapless guided implant: Will this fail?
New comments are currently closed for this post.
Paul
12/15/2017
The only one that can answer your question is the all mighty. If a problem develops, you will learn how to deal with it. The longer you place implants the closer you get to the title of scientist. If you remember math, placing implants is like an equation of three unknowns and only one equation to help you solve it.
ROBERT KORWIN
12/15/2017
I believe 70 nt cm for Nobel Active is max torque, so you are well within limit. Did you graft around the over prepped area? If not, I think 1 mm overprep will heal by itself. When in doubt, I use a cover screw, not a healing abutment, so the tissue over the implant will assist the healing process. You are level with the horizontal bone, so in general, unless you overheated the bone, it should integrate, and look good on your x-ray soon.
Bruce Smoler
12/16/2017
Yep, allow for more creep of tissue. always a good move especially if not loading..
Dr. Rayment
12/15/2017
The positioning looks great and the lucency may just be the fact that you "over prepped" the osteotomy. Good primary stability. I think you will be pleased in a few months. Best of luck and hopefully your patient is NOT a smoker.
Jason
12/15/2017
Could be just an angulation of the new xray. Wait the four months if asymptomatic and re xray
CRS
12/15/2017
I suspect the error was with the healing abutment, most likely trauma from movement. I would have placed a flat healing screw so the implant would be protected. if you had 60ncm of torque that is very stable. Looks like it is failing.
Dean Licenblat
12/15/2017
I find that with the flapless guided approach the issue of drill cooling is a big one. You have significantly longer drills with guided surgery and the associated fact that unless you have internally irrigated drills (which are being phased out due to infection control / cross contamination concerns) you have prevention of the cooling along the long axis of the drill by virtue of the guide sleeve. Couple this with 3+ mm of gingival tissue you have further prevention of cooling. I find dropping the drill speed, chilling the saline (which I do for all cases) and use a more vigorous pumping action with only gentle pressure should drop the drill temperature down. I would also change my drills more often as the sharper drills cut more efficiently and generate less heat.
Dean Licenblat
12/15/2017
It looks like MIS not Nobel Active
Prof. Ehab Abuelroos
12/16/2017
Nice clear systematic answer
Neil Zachs
6/8/2019
Dean Licenblat is completely on the money with his comments
Neil Zachs - Periodontist
12/15/2017
You definitely have some crestal loss on the mesial which seems to only be affecting the "mini-threads" The rest of the implant looks ok and it does appear to be integrating.
I find the reason for this could be a few...1) if the site was not profiled enough and there is increased pressure causing this bone loss. 2) I would say bone heat...but since the osseous loss is so localized I do not think that this is a factor. When doing guided cases, you really need to make sure that the area/bur is getting properly irrigated. Also, make sure you change burs regularly!
I think you may be OK on this....it may not be a bad idea to open this up early and debride the site and place a Bio-Oss graft. Also consider a membrane at this point as you have full tissue coverage and you could lay a resorbable membrane over the implant for really good tissue exclusion.
Best of Luck!
Raul R Mena
12/15/2017
It is a failing implant. Remove the implant before it looses more bone. curettage and graft.
It is my believe that 35 newtons is the maximum for force in order to maintain the proper blood irrigation of the bone.
Ok I know many will disagree with my posting, but give some thought to the use of extreme newtons when placing implants .
Chanh
12/16/2017
Dr. Raul Mena, I'm intrigued by your statement "35 newtons is the maximum for force in order to maintain proper blood irrigation of the bone". I would like to get your opinion on the use of Densah burs for osteotomy preparation in the context of maintaining proper blood supply in the bone. Thank you.
Raul R Mena
12/16/2017
Chanh,
No doubt that the Denash Burrs serve a purpose when you need to do bone expansion, but at the same time they also decrease blood supply.
Chanh,
Personally and that is a matter of technic preference, when I have enough bone for implant placement, I rather stay in the 30 to 35 Newtons.
Again in many cases with dimensions of 2 mm or maybe even less, I do bone expansion a La Tatum and also with bone spreaders, with excellent results.
But having enough bone I rather stick to my Newtons.
Julian O'Brien
12/15/2017
The real question is rather "What are you wanting to guide AWAY from? As there are no nearby structures to avoid plus any deviation in angulation is easily solved with abutment solutions, the premise has to be questioned. A more direct approach would have allowed greater vision, irrigation and less flutter of the heart.
Kaz Zymantas
12/15/2017
The angulation of the x-ray is not the same for both so it is not possible to definitively know if you had bone on the mesial when both x-rays were taken. I would remove the healing abutment and place a cover screw. See what happens. Take an x-ray 3 months later and see what is happening. If there is fibrous tissue between the implant and bone then it is best to remove. All of the commenters have great answers and there is probably no one best answer to this dilemma.
Neni Shriver
1/31/2018
I like your answer best.
Drg
12/15/2017
Looks great! Keep up the good work. After about 1000 implants you will worry less. I promise.
Paul
12/15/2017
Some of us would recommend you do endo treatment on the implant you placed. May I suggest that you hurry up and wait. Why put the patient through anything when there is no indication of anything wrong other than an x-ray with many interpretations. Would you consider sectioning the mandible to learn what is the true picture? The patient is not going to die and in the worst case scenario, you may end up redoing the implant free of charge when it called for. It is always possible that someone takes the implant out, grafts the site, puts in a new implant and the same "thing" happens. This patient will never consider another implant. The all mighty did not design the human beast with a manual where it states that healing is complete in four, six months, etc.
My credentials: Twenty years of experience, many years of learning the subject, and no certificate of brain malfunction. Read medical literature and watch other areas of treatment where grafting and bone are of concern. Dentistry is a small sliver in a big pie. Also, the preservation of my ethical standards are a high priority.
Chames
12/16/2017
It has been a pleasure to read your reply.
K
1/19/2018
hurry up and wait it is - WOW
Oleg Amayev
12/15/2017
Did you used surgical guide? Without surgical guide don’t place implant Flapless, you may miss a bone.
Looks like you missing Musial Buccal bone that’s why you getting resorption. I would remove it place another implant possible narrow diameter and graft that area.
Dorian Hatchuel
12/16/2017
You're on the right track....
Continue doing all implants guided. It's State of the art and well worth it for you and patient.
However, stop doing flapless implants, it's not worth it.
Ideally you get one chance to place an implant so why compromise because the guy down the road can do it faster and with so called fancier techniques.
Do the treatment that gives you most control.
Minimally invasive surgery is more difficult than open flap surgey. It does have more failure rate so why do it?
Leave the immediate loading and flapless to doctors that are experimenting, charging more to make up for failures and redo's.
Stick to the principle of state-of-the-art but conservative. Flapless is not conservative, it is reckless.
All the answers above are good. At the end of the day decide whether you're pushing the edge or performing tried and tested techniques in your office so you can sleep at night.
Immediate gratification is not for everyone and certainly not necessary.
Oleg Amayev
12/16/2017
This is most ridiculous thing I ever heard.
Dr. JOE Orti
12/16/2017
First x ray, a monument to perfection... Then instead of placing with one turn a cover screw, you blew it by torquing the healing one With no force control. Try to remove the cover now and the Implant will come out. Then insert a wider platform with lower torque.
Raul R Mena
12/16/2017
If you don't remove the implant, please send an XRay taken 6 month from now to see how much bone destruction, and periodontal condition exist interproximally.
My credentials 40 years of implant placement.
Diplomate American Board of Oral Implantology Implant Dentistry
Hospital Base Residency of Oral-Cranio-Maxillofacial Implantology
CoDirector with Carl Misch of MaxiResidency CE Course at Pittsburgh School of Dental Medicine
Hope that Paul is right and that am the one that misdiagnosed this XRay
Bruce Smoler
12/16/2017
GAME ON.... good points on both sides. My credentials 30 Years of less known stuff Carl has told me for decades both in his Residency and as a long study club follower. My supposition is bur chatter ate away some of the crestal bone compounded by two dissimilar angulations (front and back ) of films.
Girish Bharadwaj- Oral Su
12/16/2017
Few observations. As many of my learned colleagues have said it is always better in the hindsight.
First of all no need to panic and let us get the information clear enough.
1. It appears the extraction site was not mature enough at the point of entry and this could contribute to early bone loss combined with the impact of drills. Learning point- better to use direct flap approach when in doubt or convert guided to open flap. Can the author explain the justification for this simple procedure which is used by most start ups in implantology.
2. Since the damage is done have a baseline CBCT which will give you exact info on what is actually going on.
3. What is the logic in healing abutment in 2 weeks time . What protocol is it?
4. If you can prove significant bone loss on CBCT and if it were to be my patient, I would put my hands up and remove the implant and start again. Good in the long run.
It is very true no body died of this error , let us take a prudent approach but surgery is and truth can be harsh. We need to stand up to reality.
Paul
12/16/2017
Raul Mean, your credentials are impeccable but I am surprised that you make predictions like a student. People with credentials are many and many of them are guided not by wisdom an knowledge buy desire to impress others. You may consider giving some thought to your personality before the implantology.
Raul R Mena
12/16/2017
Paul,
My only purpose of posting on this forum is to interchange experience and opinions regarding dentistry.
This is not a forum for Psychologists or Psychiatrists, so I will not respond in kind to your comments regarding my posting.
You have my name and my email address, if you want me to respond in depth to your psychological evaluation of my posting, please send me your First and Last name and email and then I will be more than glad to freely respond to your remarks without involving the rest of the other doctors in a personal debate.
Hope that when we do so and understand each other psychological makeup then we could have a respectfull professional relation.
Sincerely
Raul R. Mena DMD.
Duke
12/16/2017
Gosh, I guess my eyes aren't what they used to be, because I don't see ANY difference between the two radiographs, except the second one was exposed longer. The angulation looks the same as does the crestal bone and where the bone appears to contact the implant on the mesial just above the second thread. What I would like to see is the pre-treatment x-ray. Now if the tooth had been extracted years ago and all of the bone had filled in 100% and was uniform, then maybe I'd change my mind, but I'd suspect one would see a similar "bone loss" pattern in the pre-treatment film.
Ramos
2/5/2018
It seem to be you are the only with 20/20 since both x-Rays show exactly same situation with implant the difference is in the X-Rays darkness (grey scale/ exposure).
Chames
12/16/2017
Too early to worry about the fate of the implant.
To compare the 2 images, you need to take into account the angulation and brightness / contrast of the x-rays. It seems that the mesial void did not change. Just monitor the evolution and intercept in the unlikely event of a complication.
Paul
12/16/2017
It would be nice to have a place where all these cases are followed over years and saved. Perhaps we would learn if all our predictions and claims had any merit or not. Science keeps writing new pages every day and we need to be aware of it. We should look into orthopedics and learn that what we struggle with is long forgotten in their discipline. Those that attended dental schools 30 years ago know the faith of amalgams and how much time was dedicated to a simple dilemma while everything else did not matter. If the world went about issues the way dentistry does, we would use vodka as anesthetic and wood for everything else.
Brian
12/16/2017
Hi all - original poster here. Appreciate all the advice and comments. Just some further information;
I have been placing for numerous years but this was my first attempt at guided and flapless. I chose this route to minimise stress for myself during placement, obviously hindsight is 20/20.
The healing abutment was placed directly after the initial X-ray. The second X-ray was taken at review and no additional treatment was performed.
I believe the appearance on the mesial is due to overprep of the Osteotomy. It is visible on the initial X-ray and like others have suggested is possibly worse on the second X-ray but exposure and angulation makes it difficult to tell. My original questioning was essentially will ungrafted defects of this size tend to integrate - which has seemed to split the camps. In hindsight cover screw vs healing abutment would have been advantageous and of course flapped surgery vs flapless
Paul
12/16/2017
Dear Dr. Raul Mena,
I hear you loud and clear and just like you I agree that this forum is for sharing experiences and knowledge. The reason your comment upset me is because I feel that some of our younger colleagues who are asking for opinions and experiences should not subjected to what you have done. Reread your post and you should see that you outright told someone to remove the implant. Your words: " It is a failing implant. Remove the implant before it looses more bone. curettage and graft."
Your post reminded me of many other similar posts and truthfully they tick me off. We turn a question into a parental relationship with colleagues who may not have as many years of experience. I resent comments like your's under the pretext of experience. Many procedures, most of the technology and science of placing implants have changed drastically. Even Dr. Brenemark did not foresee the changes that have taken place (example: immediate loading). It is time that we act like doctors not just be called doctors, professionally and respectful. As to my comment about paying some attention to personality traits, I don't think I was wrong.
Raul R Mena
12/16/2017
If you get upset with my response then you should explain why you disagree with my posting. I try to be respectful and give and unbiased opinion. Again you are again using words like Parental Relationship that have nothing to do with dentistry and much to do with Psychoanalysis way out the expertise of this forum.
When I see an implant with radiolusency almost down to half of the apical portion I can tell that there is a problem. Removing the implant now and grafting will prevent a worst situation in the future. If you think that bone is going fill the void, then advice the Dr. to leave the implant in position. I totally disagree, and my advice is remove, graft and replace.
By the way is not that Dr. Branemark didn't foresee the changes regarding immediate loading. The truth is that Dr. Branemark failed to acknowledge and recognize that many years before he accepted the technic, there were many doctors doing immediate loading, and thousands of implants that had been successfully placed with immediate loading.
Hope that this calms your anger, there are many other important issues to argue about.
Sincerely
Raul
George Y
12/16/2017
I think that defect on the mesial was there previously but the new radiograph was taken at a slightly different angle. Also, difficult for us to help you when we do not see a 3D scan view.
Dr. Arturo E. Gonzalez DD
12/16/2017
Hi there, in my opinion I think it may have been over prepped/possible heated up the bone to much. In my experience with guided surgery anything that is not 100% will effect the optimal out come of the surgery, i.e. you mentioned your guide was moving or hard to keep in place. Things of these nature will cause complications, and I believe that you are correct about the over prepping. Having a very well tight fitting guide is essential, if I am worrying or placing to much effort on dealing with a guide in any way it takes away from my surgery. In most of my cases I have outside lateral irrigation directly to the osteotomy and to the flutes/drills. This prevents from any overheating of the bone/osteotomy and drills, which can also be something that is attributing to this scenario. I can recommend a good lab that has been providing me the last 80 surgical guides or so, the name of the company is DentArt digital dental labs, they provide the option of outside lateral irrigation canals and the guides are extremely fit with no movement, rocking, adjusting, or nothing that would take away from me concentrating 100% on my surgery. The fit is usually so tight and precise that removing it requires some finessing. I can highly recommend them. The planning to post X-rays on my cases show they are highly accurate, if you are interested I can send you some examples in the many cases I have worked with them. Customer service is excellent, fast turnaround, free shipping, Dr. oversight, and excellent prices. I wouldn't trust anyone else at this point due to situations I have encountered as you mentioned in your post with the guide.
At this point I think its a bit to early to accurately say if the implant will fail. I would give it more time to see what develops and take action at that point its very hard to make accurate predications from this stand point. Thanks for sharing.
Prof. Dr. Peker Sandalli
12/17/2017
You can not know the exact reason why there is a resorption around the implant.
I tried to use bone augmentation material just before the insertion implant and never resorption has been occurred. Try it.
Can Bayrak
12/18/2017
According to your experience, can this gap be filled without any intervention? The radiographs are only 2 weeks apart (as far as i can understand) could that be bone resorbtion already?
Should we wait and see?
Augment around the implant?
Remove and augment the area and replace after 4-5 months (how long?)
Thank you
Dr Joe Nolan
1/18/2018
Message for Dr Sadnalli...can you elaborate a little on what it is your technique, it sounds interesting....
Best wishes
Joe Nolan
Ireland
Mark Barr
1/30/2018
hi to all
just reading this thread is a CE course in itself and I thank you all. Take 2 additional periapicals from a bitewing perspective and see where the healing is. Post a follow-up if you can. Ty
Brian Williams
2/3/2018
Hi all. Original poster her
Implant reviewed today 2 months post op and all appears to be integrating successfully. Will try post a radiograph
stikkirice
2/3/2018
2 Month post op healing radiograph
Fernando Campos
2/20/2018
I would not read to much into it,primary stability its great when you place both xrays side to side the second one has sligth distorsion that might account for ( radiolucency in mesial) i do not think that just happened after insertion i believed it was there at time of Insertion. I would wait 4 to 6 weeks more than traditional 3 months . It's going to be ok
Admiral518
6/8/2019
Wondering if there is more to this tale? I am just seeing this June 2019, alot of heated opinions. So, How did it turn out? Is there another xray to view and comment on?
stikkirice
6/8/2019
Pleased to report the implant integrated successfully, was subsequently restored 3 months after the original post and is in function. Will post radiographs when able.
Paul
6/8/2019
The bone overheating issue when drilling the osteotomy is a great exaggeration. I have never seen any study that would figure out a way of measuring the increase in temperature when drilling with irrigation or without. The bone hardness and the speed of drilling can be compared to drilling in non biological materials. The depth at its maximum in the case of osteotomies is also a factor that does not contribute significantly to the rise in temperature. Creating dilemmas is a dentists love at first sight.