Large radiolucent lesion on lower first molar: immediate implant?
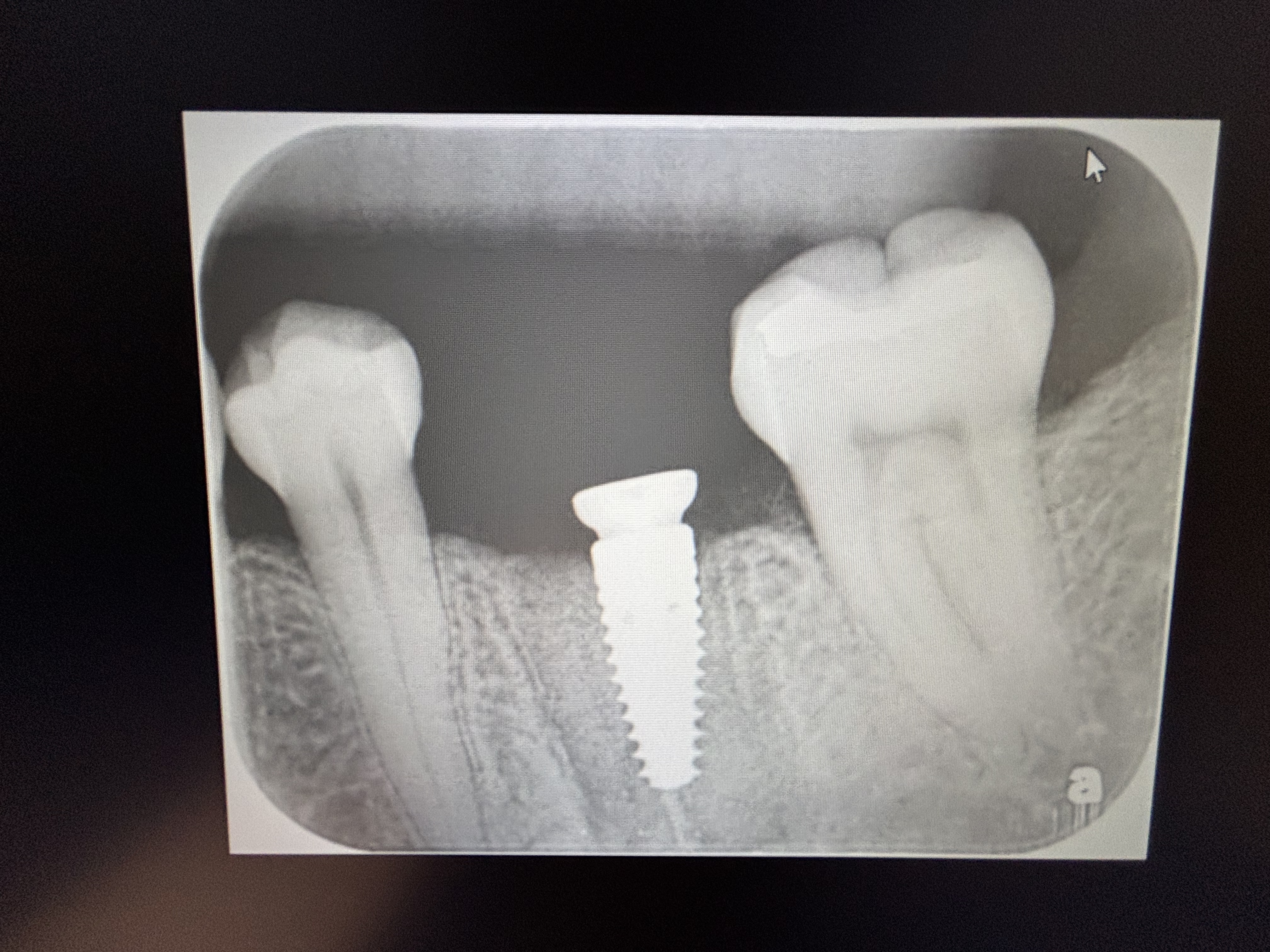
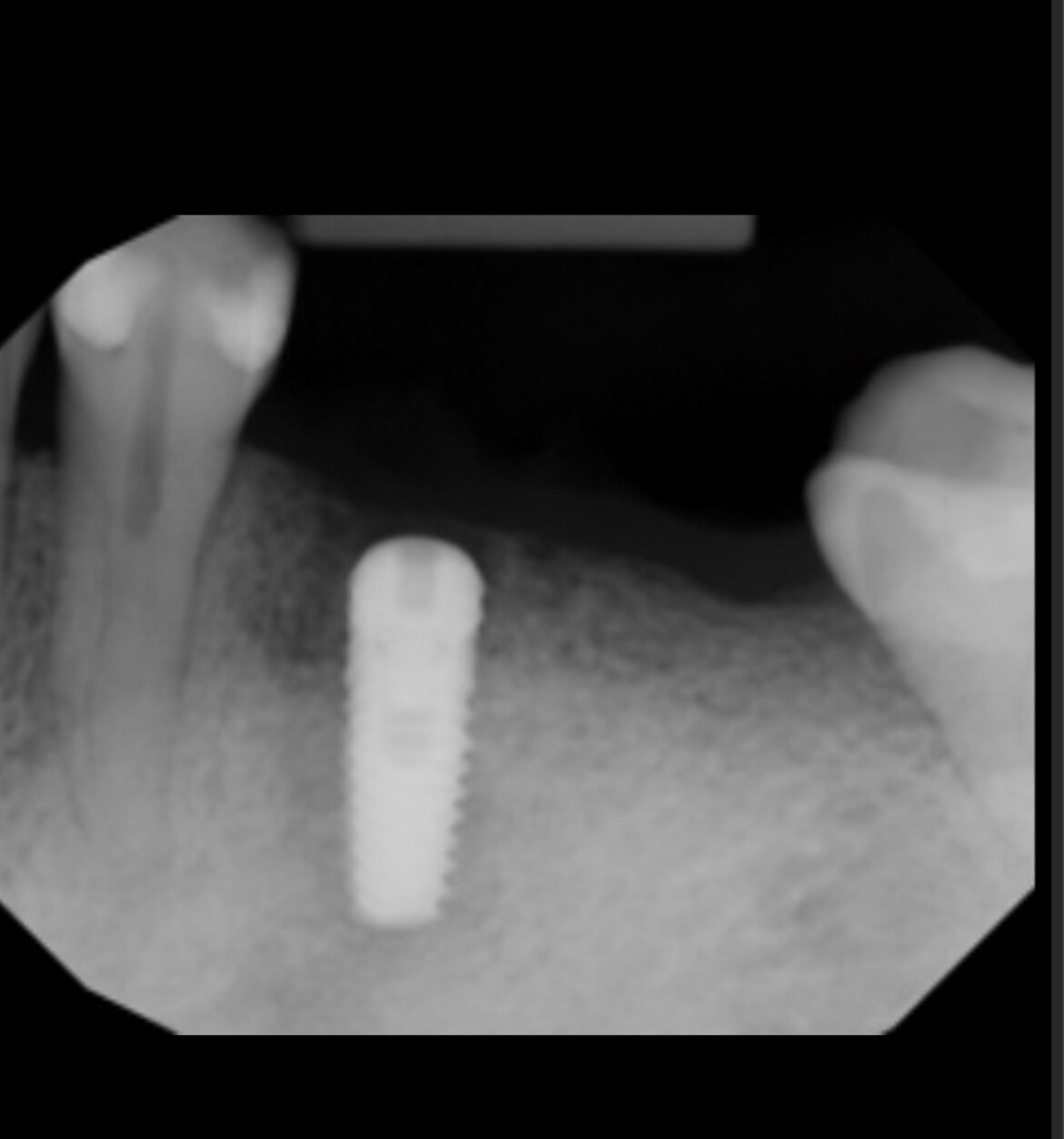
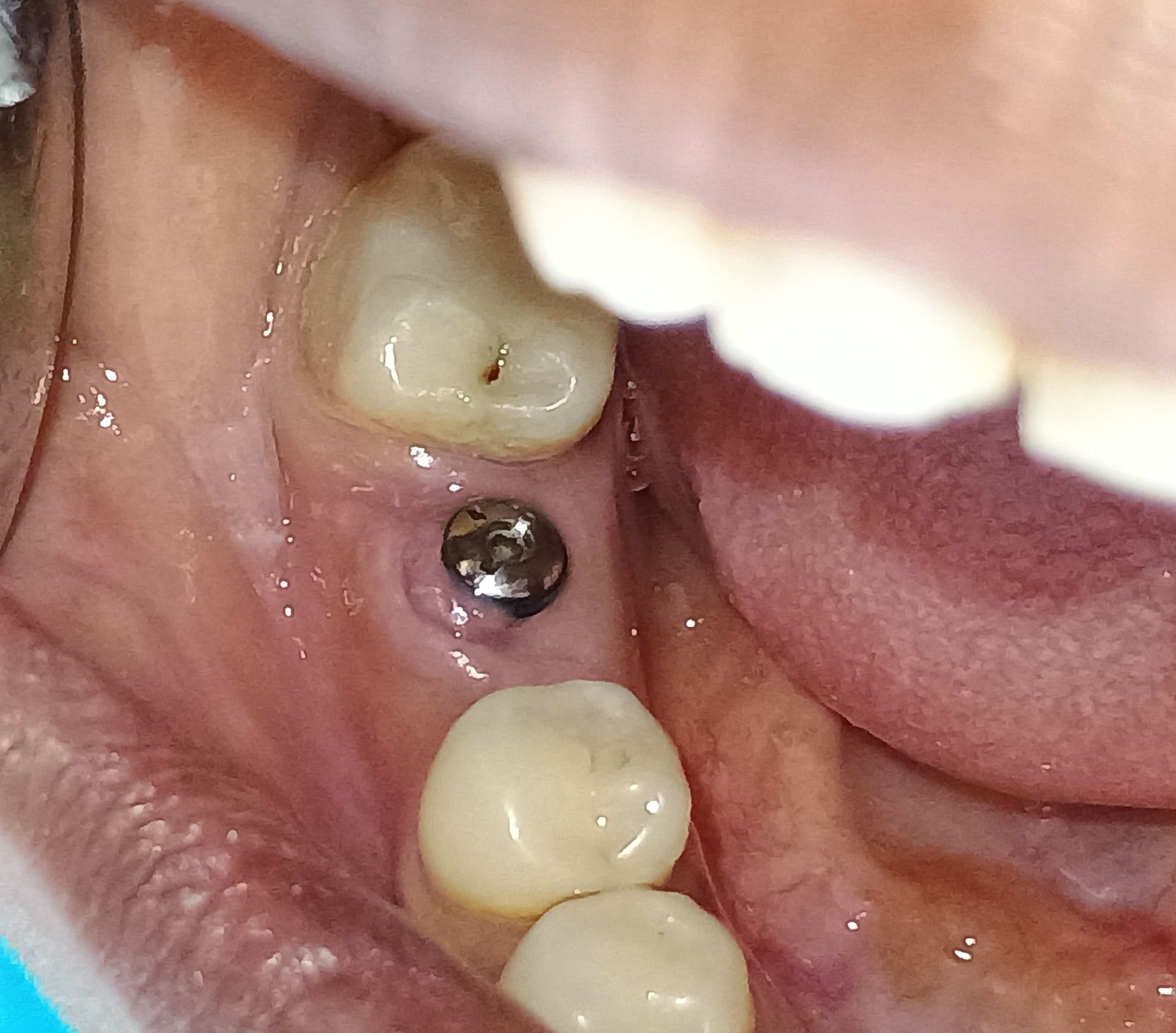
This patient presented with a large periapical radiolucent lesion and a buccal swelling over the mandibular first molar. I would like to do an immediate implant. I plan to decoronate and split the mesial and distal roots and then extract each one. Then I will debride the socket and place the implant. Or would it be better for me to extract, debride and wait for the site to heal and go back in later? What do you recommend?

30 Comments on Large radiolucent lesion on lower first molar: immediate implant?
New comments are currently closed for this post.
Barry J. Litwin
9/13/2017
What's wrong with root canal therapy?
Bradford McLaughlin
9/15/2017
looks like there might be caries under the distal margin of the crown. hard to be sure.
Dr F
9/13/2017
Extract. Wait go back later. What's the rush?
Joseph A Oleske DMD
9/13/2017
The extraction and immediate implant may work, but you must take into account the risk factors of the patient's medical history, their tolerance for failure, the materials you plan to use, and your own skill levels. I've done what you are proposing successfully, and I've had it fail too.
You lower the risks of failure dramatically if you graft and delay placement.
Dale
9/13/2017
Is this the only image you are basing your decision upon? And, why would you place a foreign material in an area already compromised by infection? If you are planning an implant get a pre-op CBCT as well. There appears to be possible resorption or secondary caries on the distal root surface...knowing what is there exactly may help decision...and a surgical guide will ensure success...
Matthew Watson, DMD
9/13/2017
Sounds like there is good chance of buccal plate perforation and significant infection. Why not get good night's sleep, extract, socket graft and place implant in 4 to 6 months. Better for you and patient. I'm not fan of immediates but they seem to do well for many. You just need to know if you are one of them. Good luck
Paul Newitt
9/13/2017
A couple of questions and comments to think about, not criticism but what is going through my mind.
Studies do support the fact that a tooth successfully treated with Endodontic therapy has as great a survival rate as an Implant. Was Endodontics ruled out here?
As far as immediate. how are you going to ensure the infection has been eliminated in the cancellous bone? Curetting the bone is unlikely to rid the area of bacteria.
With that size of defect in the bone, undercutting the septal bone there, what are the chances of having enough bone for initial stability? You are more than likely going to have a 10+mm defect Mesial to distal. Once you prep your osteotomy the septal segment of bone will be gone. Is there enough apically for stability?
If you are going to then graft the area to fill the gaps, how will that graft survive in the low pH environment of the infected bone?
Just a few things to think about and would love to hear some replies.
Adam Pite
9/13/2017
It looks like there is large caries on the distal which may complicate restorative without crown lengthening. This might be the motivation for extraction over endo.
Paul Newitt
9/13/2017
Good Eye Adam. I hadn't blown up the image and didn't see that at first. but yes that would make sense.
Dr Bruce Smoler
9/14/2017
Out of curiosity, what study are you referring to and what constitute success? Not removing the endo tooth in 20 yeas? Or the number of crowns need replacing after an average of 7 yrs(ins statistics). Not to be pedantic, but I am not aware of studies that show endo to be just as efficacious as implant therapy. I did see a study show endo tx being less invasive due to the increase in Peri- Implantitis,
Reg O'Neill
9/13/2017
First thought (immediate), this is an endo case. Acute apical periodontitis treated by titanim implant? This would be hard to support I am sure you will agree when you review your case. The radiograph of course is not imaging the whole crown, hence request for more info. Hint of distal caries on image.
We need much more diagnostic record to help you. If the tooth has to be extracted, no to immediate implant.
Haydar Alkhatib
9/13/2017
Immediate implant in such a case is not the best option niether for you nor the patient , and why wouldn't you do root canal therapy? What would you do if this is your mouth?
Howard Aaronson
9/13/2017
Why is endodontics not your first option ? Bone support appears good unless deep pockets or other indication of fracture Why not treat conservatively and maintain the natural dentition? Implant and endodontic therapy are equally successful.
why place a foreign body if you do not need to. Bone will heal following successful root canal therapy
val
9/13/2017
Endo first !
Rainier Urdaneta
9/13/2017
There appears to be furcation involvement, large caries lesion on the distal close to the bone and at the level of furcation. On top of that a large lesion of endodontic origin with a facial fistula. No to endo, the prognosis of this tooth is poor.
I suggest extract and graft with L-PRF and then place an implant three months later
Paul matusko
9/13/2017
There is also bone loss in furcation. Exo, graft, wait, implant.
Cheers.
Barry J. Litwin
9/13/2017
I've read all the responses. So the tooth is not ideal; probable buccal fenestration that may heal, slight bifurcation involvement, distal root decal.
However, this tooth has a great deal of supporting bone. Root canal therapy, crown lenthgening, post and crown and even a possible apico could give this patient 10 to 15 years of service.
If it were my tooth, I'll take the 15 years then reevaluate!
Mike B
9/13/2017
The patient should be presented with treatment options, educated and helped to make a decision. Root canal therapy may work long term and it may not. The same is true for an immediate implant with debridement. I would not suggest an immediate implant in this case. The risk failure is too high. However, if the patient is educated and accepts the risk it's an acceptable treatment.
Merlin P. Ohmer, DDS, MAG
9/13/2017
I know if one does an immediate implant, the sale is done, but that is not generally the best. I would remove the tooth, perform a graft and allow to heal. Then the site would be wonderful to place an implant with a great chance of success.
Dr. H. I. McDunnough
9/14/2017
Do undo others as you would do to yourself. You would want an implant in a case like this?
I would hope you would prefer to do endo before opting for an implant in this case.
Dr. Nathan Arizona
9/14/2017
To even think of implant before doing endo in this case is being inept.
Merlin P. Ohmer, DDS, MAG
9/14/2017
The decay on the distal is the deal breaker on restoration.
Walter Mick DDS
9/14/2017
This appears to be non-restorable because of the distal sub-osseous caries, furcal bone loss, and periapical abscess. Individually, each of these could be rectified....all together, not so much (especially the distal caries).
Immediate placement of an implant would be very difficult. The distal root will not come out easily due to the widened portion midway apically. The resultant bone destruction, along with the high probability of a buccal wall defect, would necessitate grafting. Allow adequate healing, then place your implant where you would want it with appropriate initial stability.
joe nolan
9/14/2017
merlin got it first time, there is a cavity almost to bone distally, I apologise for not showing this. All replies well worth considering...I would have done endo in a heartbeat, the distal caries did for the tooth, hence the implant avenue....thanks to one and all.
Sean
9/14/2017
I never liked the "if this were your tooth argument", and I prefer, "if this were your friends tooth who lives in another state and is paying full fee". It is a tough case to restore given the perio and distal root decay. Yes, it can be done, but it will be endo, restorative, perio for a fee of $3000-6000? (fill in your number) which may last a few years if perfect hygiene, but will fail and need exo and implant at a cost of another $3-6,000? I like predictable. My vote is extract, heal, graft as needed and implant.
michael valenzano
9/14/2017
Root canal first then if unsuccessful in in 10 to 15, extract wait for healing then implant then when it fails do the implant what is the rush to extract and place implant esp with buccal fenestration.
Afshin Danesh
9/15/2017
The x ray doesn't reveal the entire tooth.
If this would be my tooth then I would go for keeping the tooth.
So in this case if the patient is willing to keep that performing endo and if needed CL and finally to place a crown and may be apico would be the final tx.
In case that the patient isn't accepting any risk to keep the tooth, how come placing an implant in an acute infection which is a contra indication in placing implant.
Extract socket preserve wait for 3-4 months place the implant to satisfy him by a reliable tx.
Leonard Smith DDS
9/15/2017
Experience of similar cases. Predictability of treatment. Cost to patient now and later. Regardless of restorative issues, this is a huge lesion and on ct will be even more invasive appearance. Extract , debride, socket graft , PTFE membrane over crest. Wait six months and place implant, wait 4 months and restore. Predictability! Graft is large, 4 months it will not organize for implant stability , wait 2 more months and it will be bone. Problem with extract and implant/graft in molars is not the implant integrating , but the crestal bone level and tissue level is not Predictable. What I don't want to do is to start a new treatment off with a built in defect . Educate the patient they are not in as big a hurry. They want success not excuses
Leonard
joe nolan
9/16/2017
Thanks Leonard, you are spot on with your opinion and way forward. Once again, I apologize for not showing properly the extent of distal caries which has undermined the possibility of doing rct and which has made the tooth unrestorable. I plan to xla next week and take it from there. Thanks again to one and all for the excellent feedback.
dr robert walton
9/17/2017
I appreciate those who want to save this tooth BUT the prognosis is poor. There is a large carious lesion on the distal that impinges on the biological width which would require crown lengthening. There is also a bifurcation involvement. And root canal therapy is required. So even after all these treats the outlook is dim. Definitely extract the tooth and place an implant. I would not do an immediate placement but would consider bone preservation and implant after 2 weeks of antibiotics