Sinus perforation and insertion torque: feedback?
First off Happy Holidays to everyone, and thank you in advance for your feedback on this case.
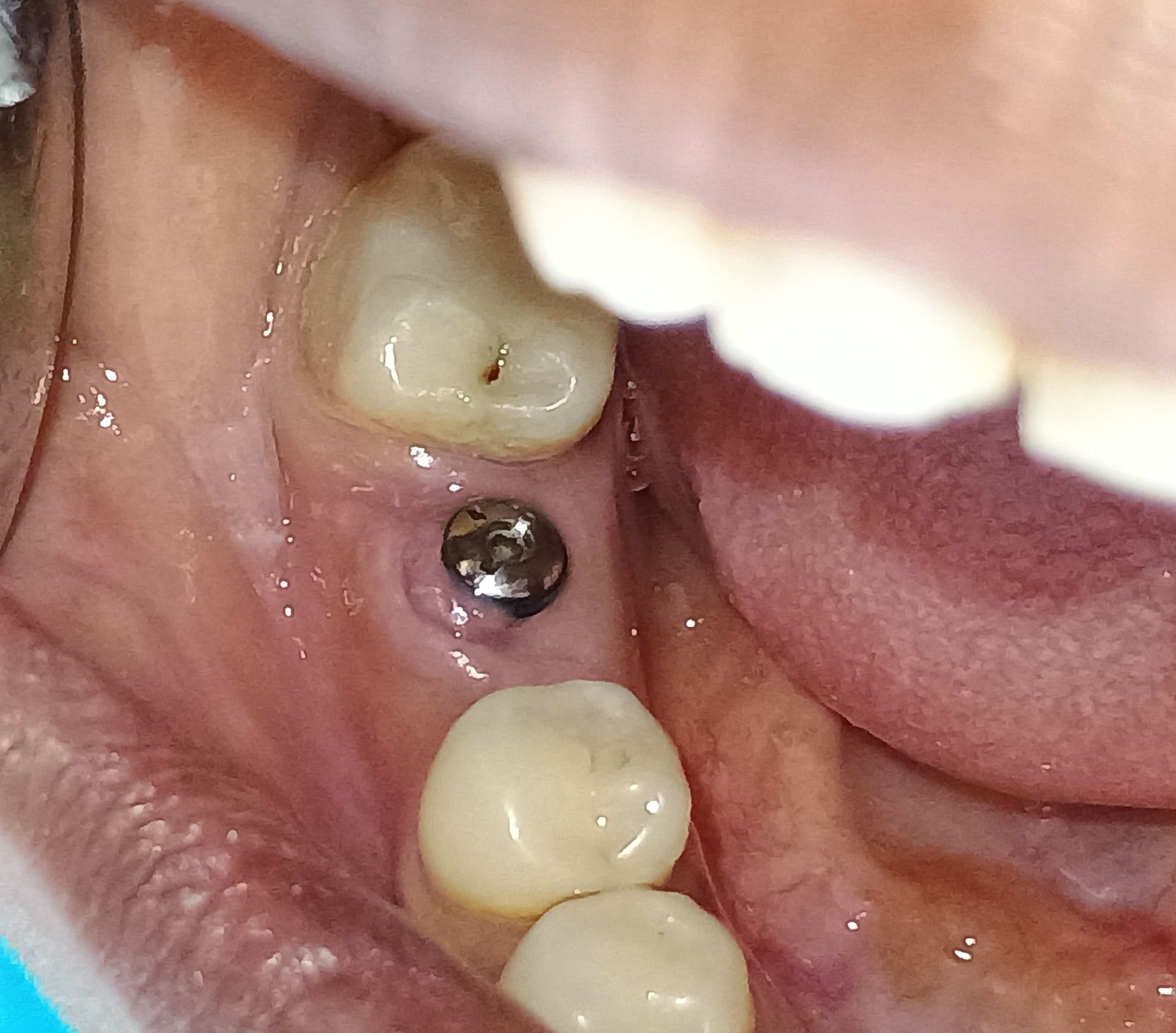
My patient presented today for placement of an implant replacing tooth #4, (patient will be getting a crown on #5 to address recurrent decay and restorative space). Upon initial exam of radiograph, I noted that the patient did indeed have a pneumatized sinus floor in close proximity to where we would be placing our implant. I went into this procedure anticipating placement of the implant with a crestal lift by Summer’s technique if necessary. My plan was to place a 4.3x10mm fixture.
As I worked my way through the drill sequence I was able to get my osteotomy to just shy of 10mm (with the CASKit lift kit) with no sinus perforation, verified visually and tactilely with a probe. I then decided to place the 11mm stopper on my drill just to get a little more depth to ensure good crestal even slight sub placement 360 degrees around my implant. Well as I took it a little further, I did in fact get sinus communication on the distal apical portion of my osteotomy.
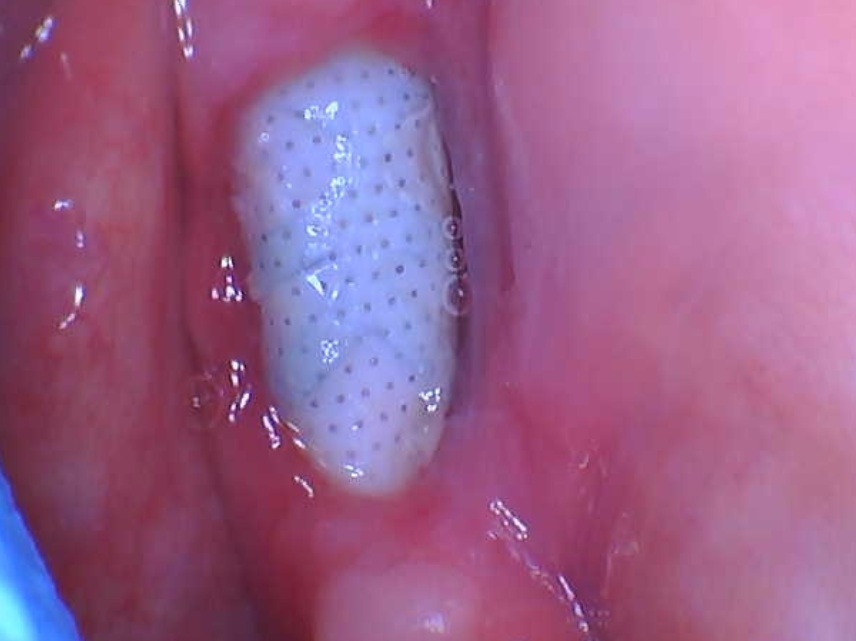
Upon visual inspection, I could see the perforation, however was unable to visualize the sinus membrane which I’m assuming could have been due to a perforation. I decided at this point to place a collagen tape dressing at the site of the perforation, and opted to not place any bone as I felt it would not be necessary due to the minimal perforation of the sinus floor. At this point I decided to hand torque my implant to the desired position upon which an insertion torque of around at least 70Ncm was attained… My patient was already pre medicated with 2g of amoxicillin with a prescription for a week worth of abx coverage post surgery.
So short story long, my questions are…
1. With the assumption that a perforation (1-2mm) did occur in the apical portion of the implant, was placement of a collagen dressing at the site of the perforation a proper means of repair?
2. Given that the implant may in fact be in communication with the schneiderian membrane (1-2mm) what kind of complications should I be looking for?
3. I may be beating this dead horse but I have seen so many conflicting opinions and reports referencing high insertion torque as it relates to crestal loss, pressure necrosis, what are your thoughts currently from those who have been doing this a whole lot longer than myself?
Again, thank you very much and I appreciate any and all input.