Lesion and Bridge Removed: Place implants or not?
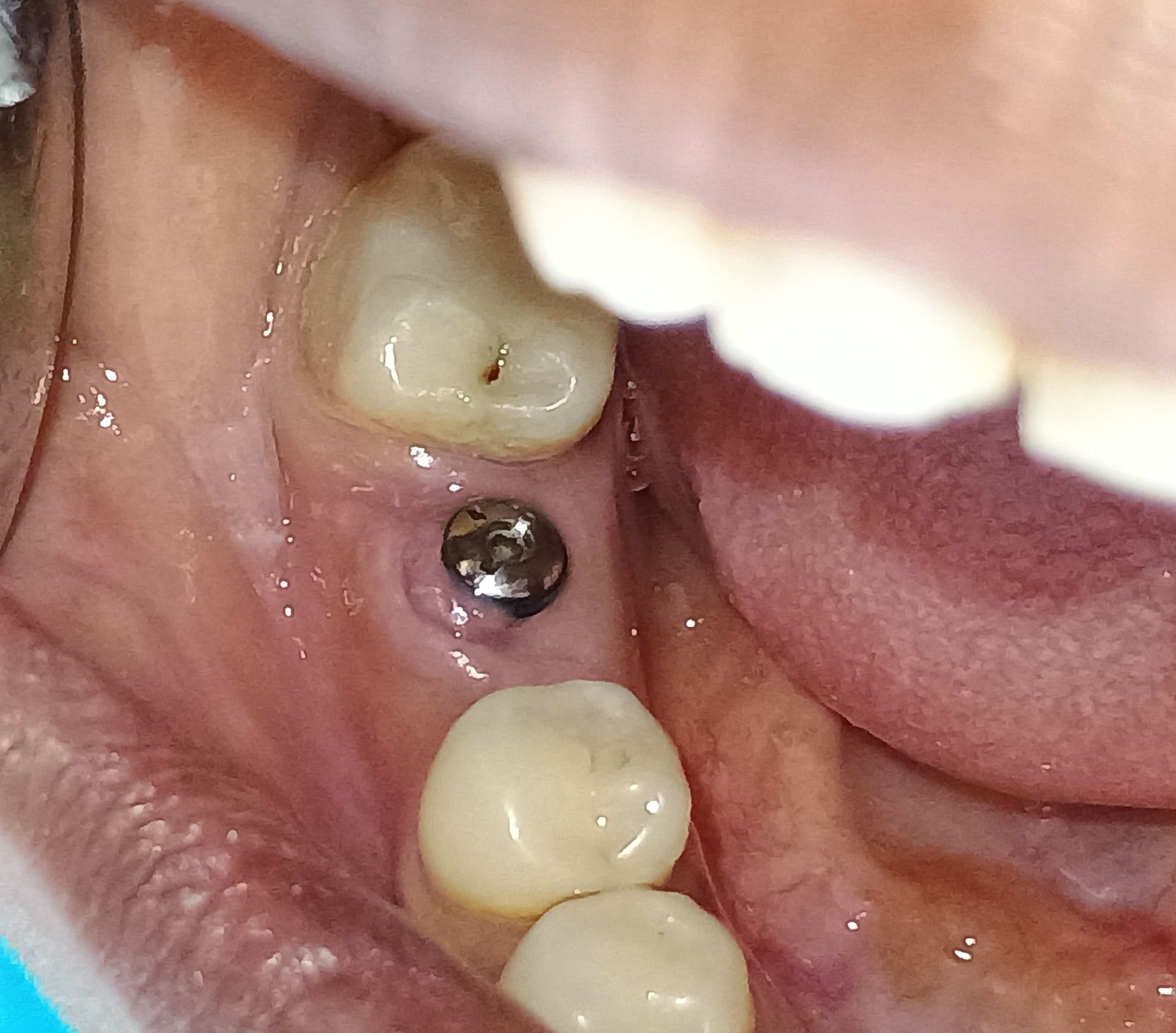
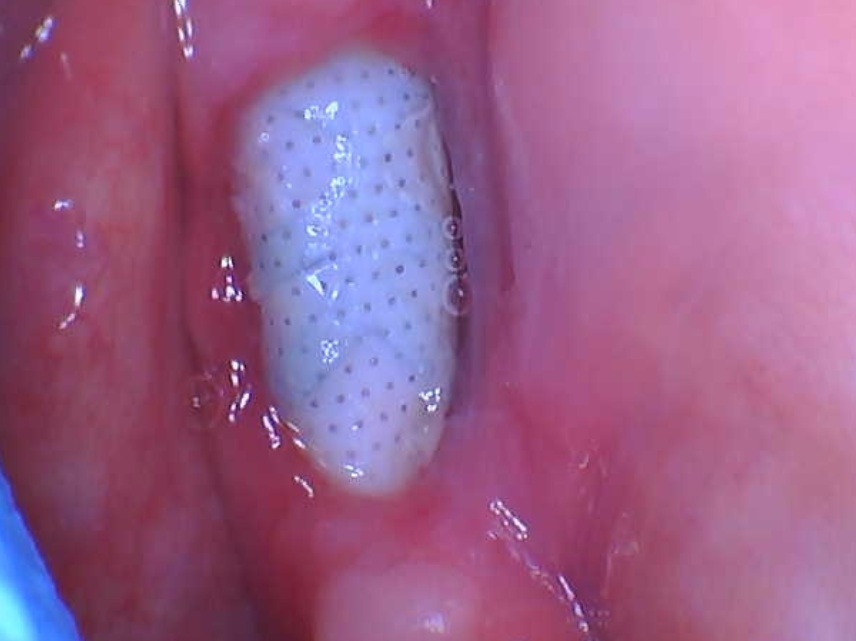
This patient had an extraction rt. lower 1st and 2nd molar 10 yrs ago with pfm bridge from 35 to 38, done at a different office. Now the ceramic has chipped off completely. RCT was done 4 yrs ago via the bridge on 38, elsewhere with an amalgam access cavity closure. The patient is 50 yrs old, post menopausal. No medical complications. Bite is a deep bite. The patient says the lesion was noted at the time of tooth removal 10 yrs ago, and has been under constant monitoring with no change in size or shape. No bony swelling intraorally. Asymptomatic on palpation. I have cut and removed the old bridge and attached xrays and cbct of the same. Another dentist has suggested a new bridge from 35 to 38 with questionable prognosis, or crown for the premolar with implants for 36 and 37 with extraction of the third molar. My questions
1. What is the lesion we are dealing with here?
2. Can we go ahead with implants or is it better to do a new bridge with questionable prognosis?
3. Do we need to do a biopsy?
4. Alternate treatment plans? Please note she does not want a removable prosthesis
Please let me know your thoughts.
thanks