Implant placed deeply due lack of palatal bone height: ramifications?
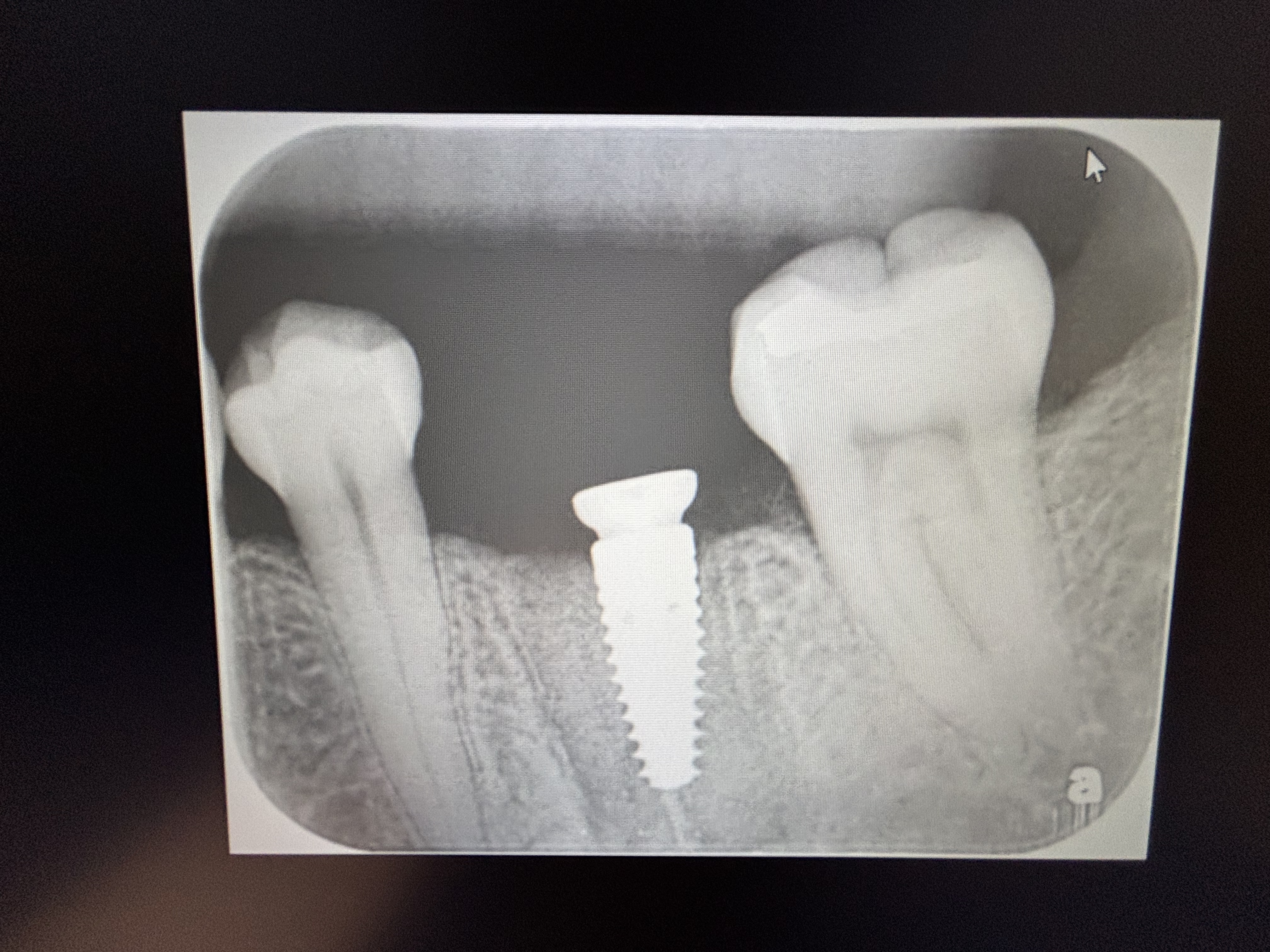
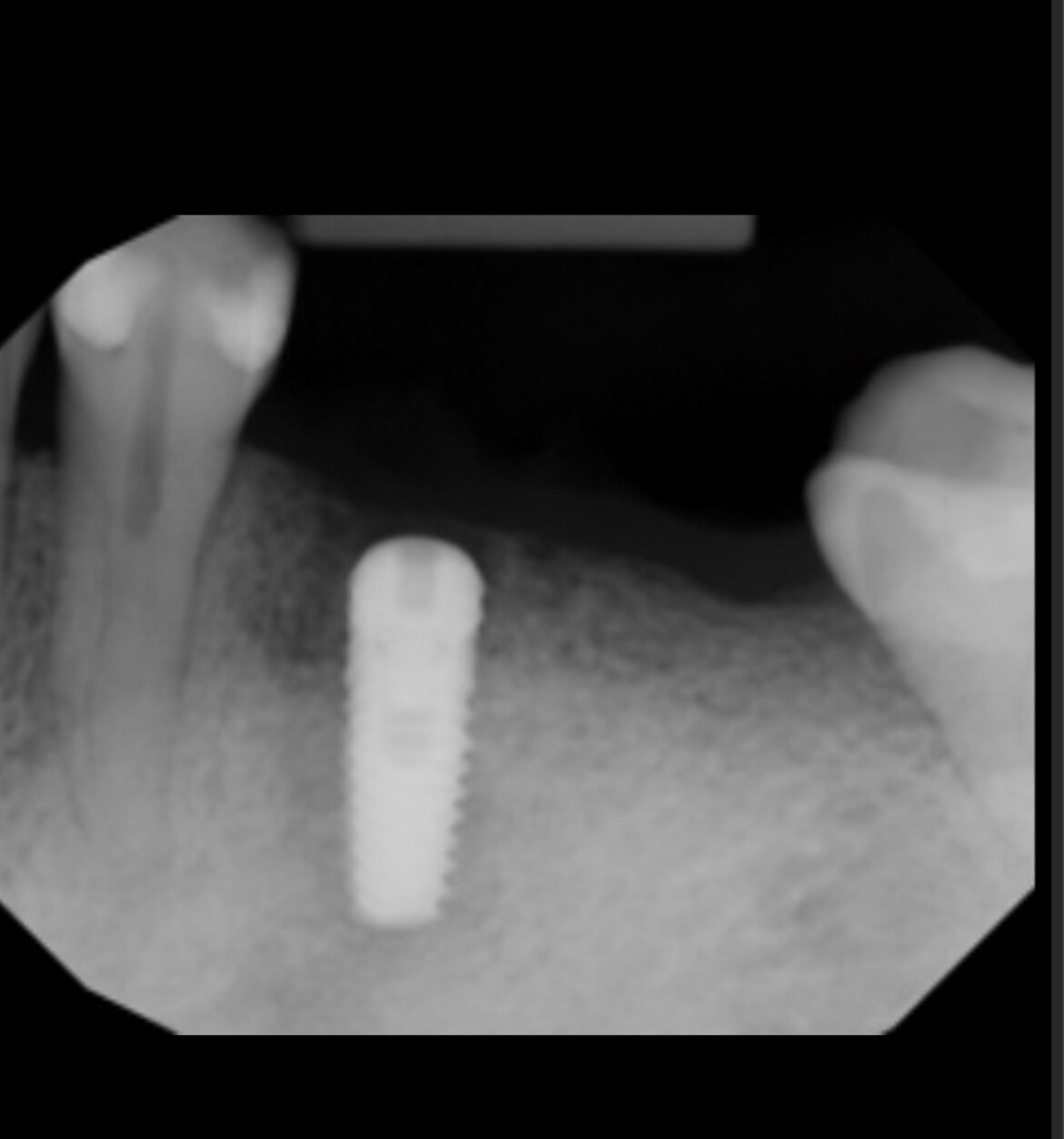
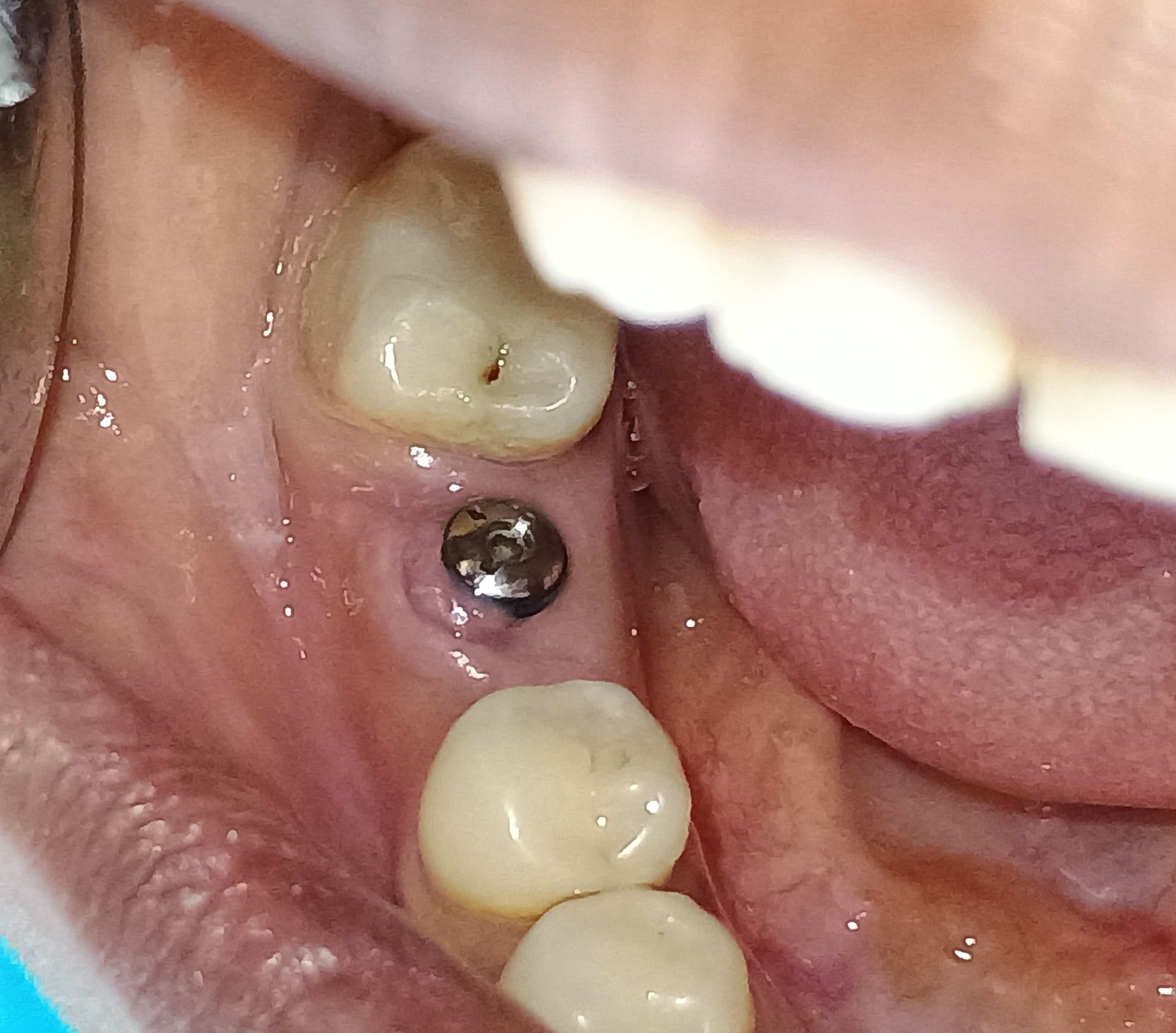
As you can see in the radiograph, I had to place this implant very deep because of lack of palatal bone. The buccal bone is 4mm higher than the palatal. I am concerned about long term prognosis for this implant. I am also concerned about the biological width and if this will threaten bone loss on the adjacent teeth. Aesthetics are actually okay. No other significant signs or symptoms. What do you recommend that I do at this point? Should I attempt GBR to augment the vertical height? Any other thoughts?

7 Comments on Implant placed deeply due lack of palatal bone height: ramifications?
New comments are currently closed for this post.
Gregori Kurtzman, DDS, MA
8/28/2017
I would have used the next diameter up which would have allowed it to be placed more coronal and still have primary stability to heal. Can also at time of implant placement place an osseous graft and resorbable membrane and allow it all to heal before starting any restorative phase.
As it is not the platform is very deep compared to the adjacent teeth and you may see adjacent bone loss over time as the bone remodels.
Ken Templeton
8/28/2017
Do nothing. Observe and if you detect progressive recession, inflammation, and bone loss then treat accordingly. Bone grafting without adjacent bony walls is not a pathway for success. Bone loss to some degree will be dependent on the type of implant/abutment connection.
GB Oral surgeon
8/28/2017
Agree with DrKurtzmann. Two stage would have probably worked better . I have my concerns in some cases as reconstruction lost palatal cortex is not easy, even with two stage .
There is also a new dimension of thinking in terms of placing subcrestally , but I don't see any evidence yet .
Recently I had a similar case but used Bond Apatite which works well in palatal augmentation cases.
If you can share pre op imaging that would be great .
Richard Hughes, DDS, HFAA
8/28/2017
I would observe. A wider implant may have to little bone circumferently, which is essential for long term success. I would have totally implant protected occlusal scheme.
A CBCT would be helpful.
This is a case that may have been best treated with a Maryland Bridge.
Peter Hunt
8/29/2017
This brings up an important question relating to the depth of placement for the implant platform. With the concerns about peri-implantitis there is a valid argument for saying that the rough surface of an implant should be placed at or below the bone line. Slightly below is reasonable because there may be some bone recession as a result of the placement procedure. The desire is to make sure that there is no exposure of the rough surface because once this becomes contaminated then peri-implantitis potential increases.
Unfortunately, many of the depth placement protocols for implant placement were developed years ago, when implants had a machined collar. Most companies did not change their surgical kits when they changed their implant to bring the rough surface up to the implant platform. To add to the problem, most bone surfaces are not flat but curved and the depth stops on the drills will prevent deeper placement. In such situations, rough surface exposure is inevitable.
There are other advantages to deeper platform placement as well. It's easier to develop an emergence profile in the abutment and restoration. It allows some "tooth movement" to provide a more natural emergence. In fact there are more advantages to having the implant platform deeper than more crestal. The one requirement is that the materials for the abutment emergence need to be bio-compatible. This means no PEEK, no gold. The best is zirconia.
dok
8/29/2017
Deeply seated implants ( for emergence profile. bony morphologic reasons or othewise )
create periodontal pockets since soft tissue periodontal attachments to abutments/ crowns is unpredictable at best. As we all learned in dental school, deep periodontal ( greater than 4 mm ) pockets allow for uncleansable surfaces to harbor biofilm. It is then nothing more than the hosts predisposition/susceptability to the biofilm pathogens that determines whether perio pathology developes. So no, it is not OK to give a patient deep pockets ( and the potential for periodontal disease ) by placing implants too deeply.
Mircea Stapanoiu
9/10/2017
How deep is too deep? We agree that slightly below crest placement works for most implant systems without machined collars.Then we have the problem of soft tissue thickness. A4 to 6 mm gingiva will give us enough headache, and trimming it will result probably in bad estethics.