Implant placed close to root: will problems develop?
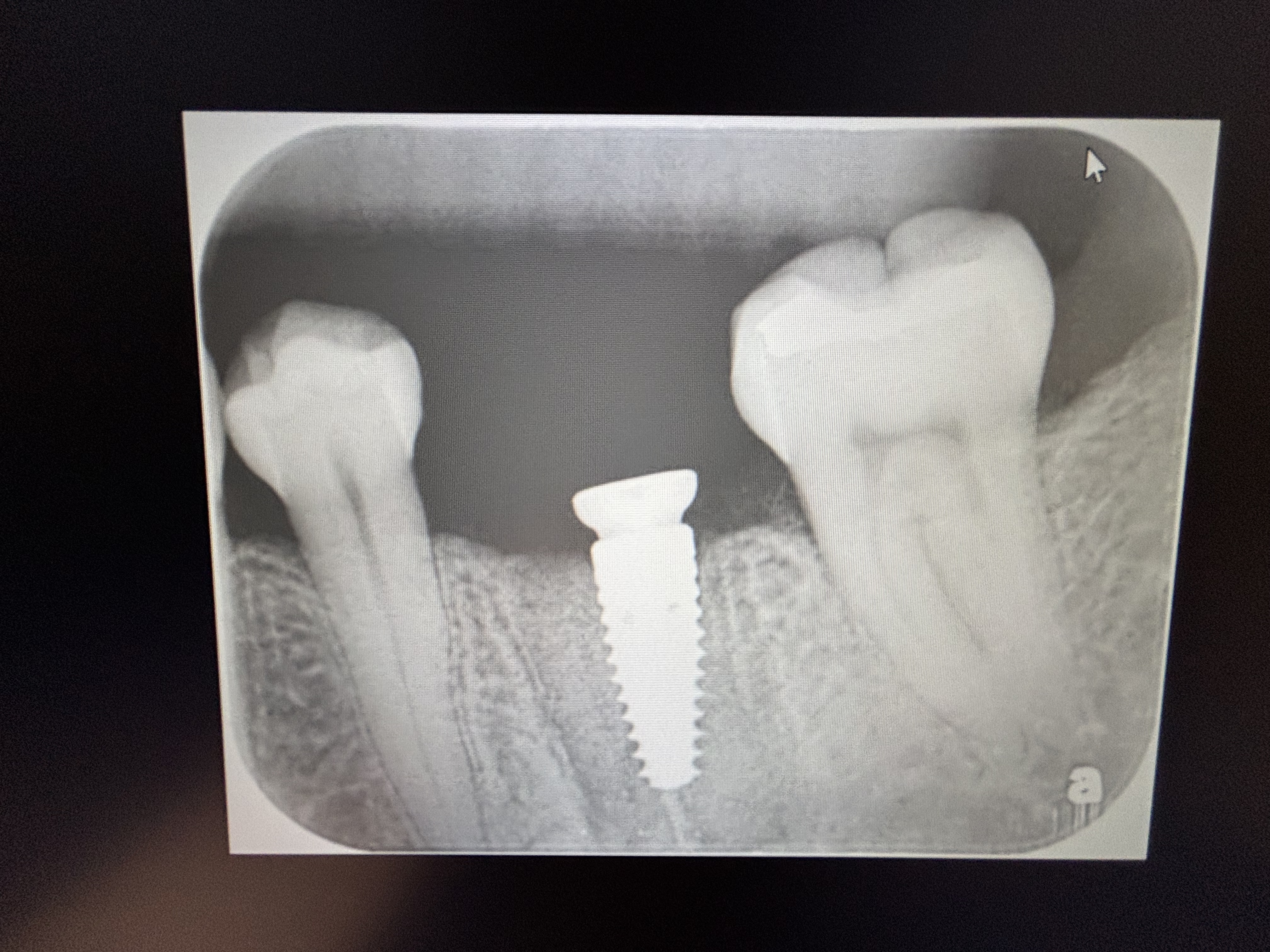
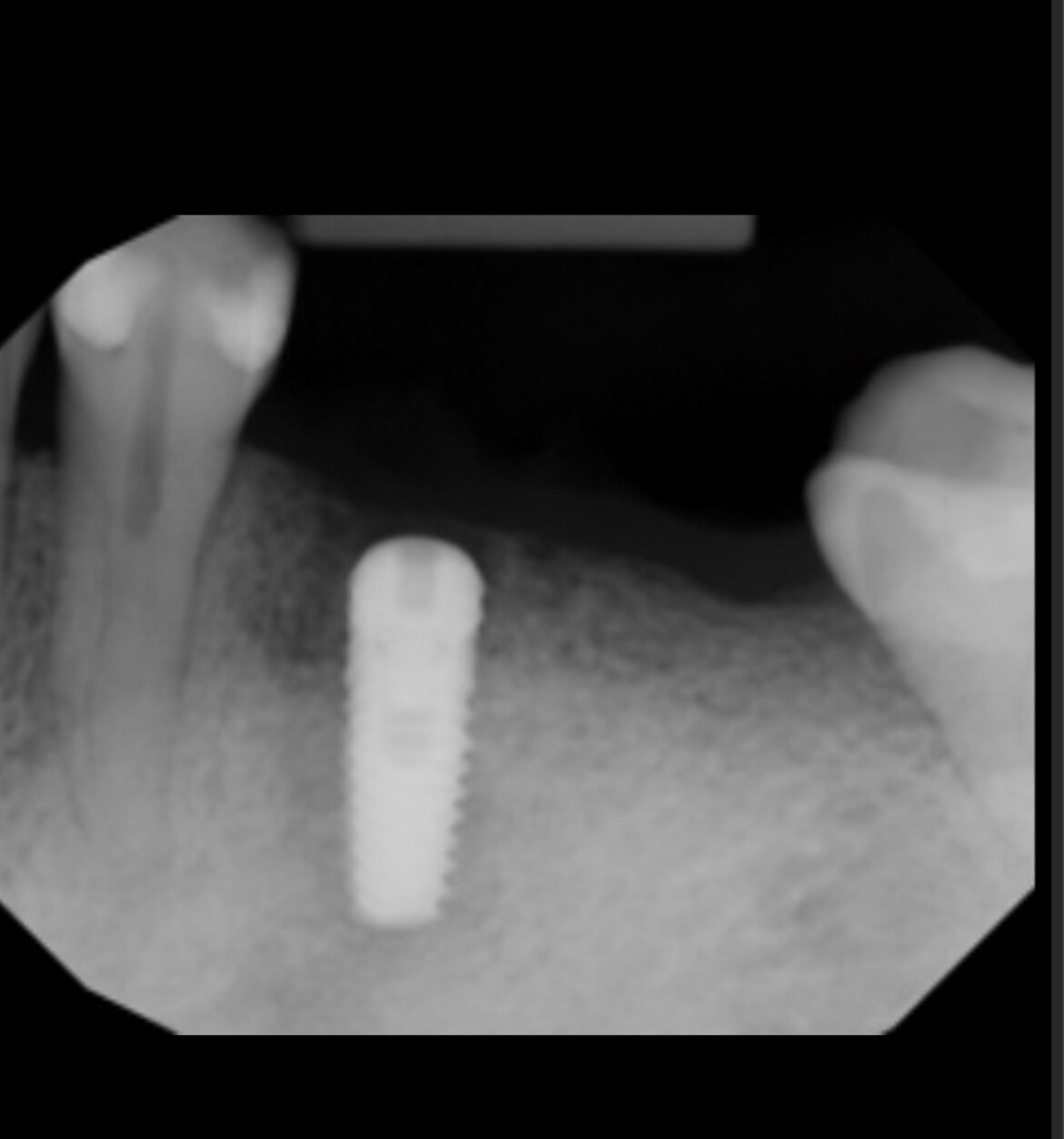
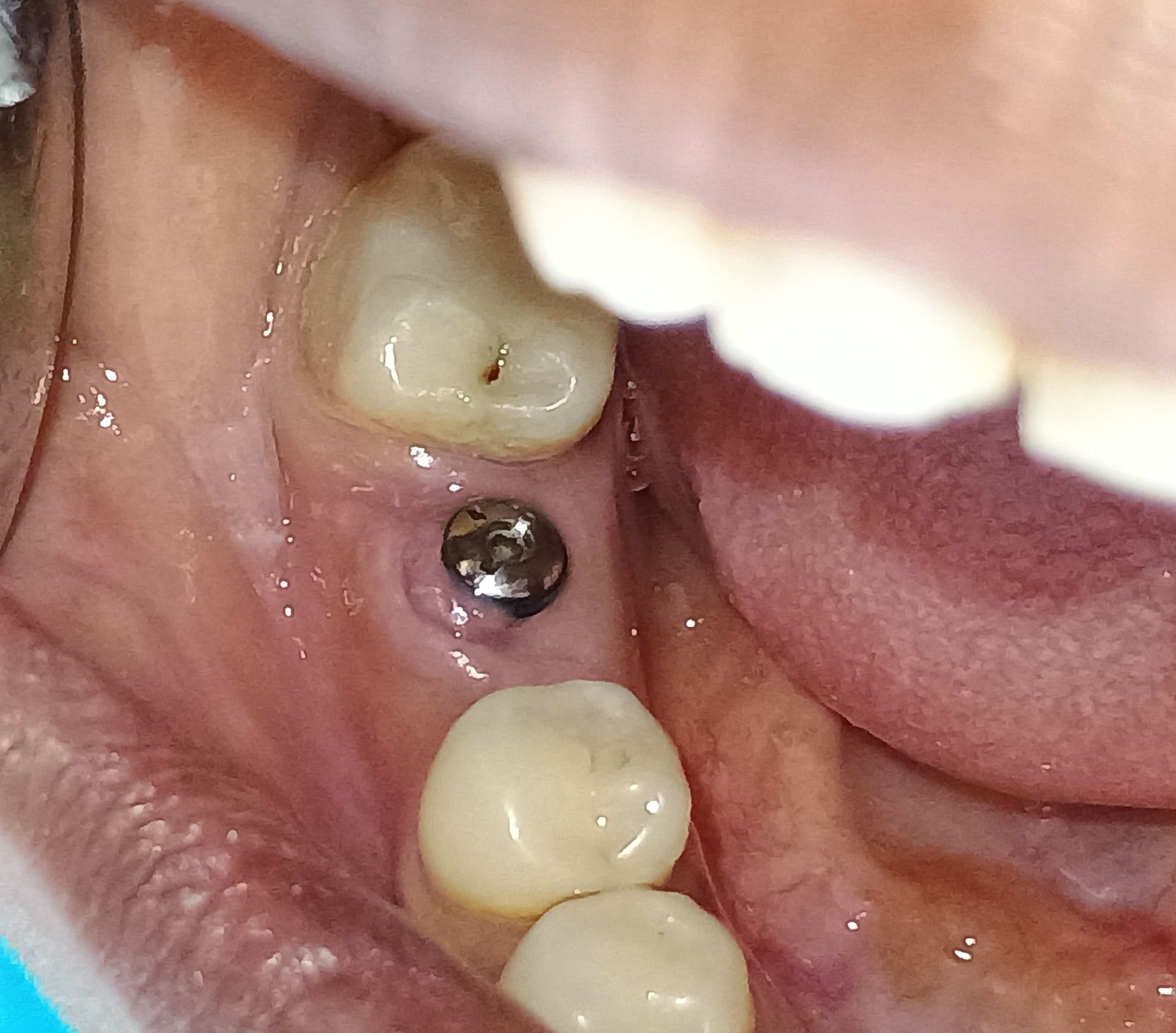
I installed an implant in #12 site [maxillary left first premolar]. The apex of the implant is very close to the root of #11 [maxillary left canine]. Do you think any problems will develop from this? What do you recommend that I do?

27 Comments on Implant placed close to root: will problems develop?
New comments are currently closed for this post.
PeterFairbairn
10/12/2015
Take two rads from different angles to assess wether it is not merely the angle of the x-ray.....
Can leave and monitor ........ but always looks messy to any future dentist , so nex time CHECK before final length and final drill ...
Peter
DR JL
10/12/2015
It should be fine if it's not touching the PDL. I would take some differently angled x-rays to be certain and then hopefully place more implants.....I would not take it out; removing it may cause more problems than leaving it in place.
Best wishes!
CRS
10/13/2015
I agree with both posts. However after assessing on angled films or better yet a cbct and you still don't like the position then remove it since it is not integrated which is simple. Place a bone graft, wait then redo with the implant parallel to the tooth root. Since you were the one there, clinically the position relative to the opposing occlusion and restor ability next to the premolars are key. You do't want to treat an X-ray, they can be deceiving.
steve
10/13/2015
no need to bone graft, but get out that bad boy asap and replace it the same day parallel to the tooth next to it. Please make sure to take an intra-op and post-op x-ray before you let the patient out of the office. Left as is, the tooth mesial to the implant will eventually require endo and most likely apico. The success of the implant is questionable as well. But as stated in my first line, this is an easy problem to repair. Just call the patient and tell them that after examining the radiograph you would prefer a better angulation of the implant and that it will be easy to fix. Deal with it now, not later.
Ziv Simon
10/13/2015
Best to Leave as removal may cause additional damage. It's a very common mistake we have all done with a first upper premolar not taking into account the distal angle of the canine. Good learning experience
papajim
10/13/2015
I agree with taking PAs at different angles.
Also, on a slightly different topic, from this image it looks like you're going to have a poor crown:root ratio. Since it looks like you have plenty of bone apically, I'd consider removing it, placing a longer implant more parallel to the canine, and slightly further distal to leave more bone circumferentially around it.
shadia
10/13/2015
I think this problem occur when bad drill angularion used during implant insertion but it may go without a problem in some patient and may cause severe pain and tooth affection specially if the cementum is injured. This complication need a thourough follow up with the patient, and endodontic treatment if pain continue.
Alex
10/13/2015
Who did not came across this situation, did not do enough implants, because we fall to learn walking... I have worse situations followed for about 10 years and everything is allright. Of course it is not a recomended situation but if you leave the implant enough time to allow osseointegration, is better to leave it in place than removing.
Take it easy colleague!! it is not as close as it could be ;-)
lance
10/13/2015
I have watched one exactly like this for ten years, no problems have developed yet............ the radiograph comments are correct. sometimes a bad radiograph will make your implant position look awful. I am amazed at the poor quality of bitewings and periapical radiographs that I sometimes see. Teeth should appear like teeth, not foreshortened, elongated, or overlapping contacts in general. I absolutely guarantee thousands of decayed areas are missed or non-decayed teeth are treated due to poor radiographic quality. take a few different angles and good for you for trying!
Dr Dave
10/13/2015
One of my first supervised implants over 10 years ago now was very similar to this one. Felt the rush of "oh no". The supervising surgeon said told me to relax and leave it. Stated 1 mm of bone beyond the pdl, while not ideal, will be just fine. While I understand the urge to make things perfect, after practicing almost 30 years now i find a lot of near perfect and not so perfect functioning just fine. Primarily I dont see the need to subject the patient to another surgery just to be straighter. And the angle can be corrected in an abutment. The maxillary bone, especially in the first Bicuspid area is a fragile being in my view. Inform the patient and monitor
Dr. JL
10/13/2015
I have one like this, its been about 10 years and so far, no problems. Learning curve is right!
drt
10/13/2015
I'm almost embarrassed to admit, but I've had 3 of these over the last 10 years. Two are fine, one might have contributed to the adjacent tooth requiring endo. The tooth was occasionally symptomatic prior to the implant, and I probably just broke the camel's back with the implant proximity. I did the endo no charge as a courtesy and nothing more has come of it. That was six years ago.
Don't stress over it. It happens. Explain the risks, alternatives, and options to the patient and let them decide if they want to go through another surgery on the chance that the tooth might develop a problem at some time in the future.
It's called INFORMED consent for a reason. Dentistry is an imperfect science at best.
Jeff K
10/13/2015
I suspect one factor in the malposition of this implant is the inherent conflict between the desire to place the implant parallel to the adjacent tooth, perpendicular to the opposing occlusal plane, and have the shoulder parallel (flat) to the ridge crest. The severe angulation, or slope, of the ridge makes coordinating all of these goals impossible. A couple of degrees more distal-apical and this would have been an acceptable strategic compromise. A useful strategy when one feels that there is no acceptable compromise in the implant position that avoids the mesial shoulder being too deep, the distal shoulder being supra-osseous, risking adjacent root contact with a tipped natural tooth, and non-axial placement of the implant relative to occlusal forces is to place two or more implants is the posterior positions (not much posterior occlusion in this case?) and cantilever the mesial pontic. Cleansable, allows more axial alignment of the posterior implants, less risk of root proximity or contact, etc. Not right for every situation, but is food for thought when the situation arises. Also, between private practice and teaching at two major universities I have seen probably 10 of these cases over more than 20 years and none have turned out bad. Granted I have not been able to follow them all for that length of time. For perspective, I have not done it, but some faculty members in a graduate Periodontics residency have been comfortable enough (in an extreme case) to do elective endo and intentionally intersect a root to solve an angulation challenge. I am not sure what one case example means, but I guess it is an evolving paradigm, like the historical fear of single stage placement in healed ridges, or immediate placement in extraction sites. Onward and upward on your learning curve. Good luck.
Vick kargodorian
10/13/2015
I would take a scan first but it seems like you can leave it alone and it will be restorable
It is a good lesson indeed so take an Intra oral x ray first with a direction indicator before going to a full length drill
Dr. S
10/14/2015
Leave the implant alone and keep an eye on it. Most likely things will turn out just fine. I have been in the same situation many, many times and most of the times the implant does integrate just fine and I was able to restore it. We, dentists, are our worst enemies. We are so critical of ourselves and each other as well. You don't find this behavior for some reason in other branches of medicine. Good luck and keep drilling.
laxmi
10/14/2015
I have also gone through with such situations.. They don't create always problems. Don't remove the Implant, just do the follow up. But very good lesson for future implant placement angulation. All the best
SAM latif
10/14/2015
I agree with the previous remark, leave it alone . if pain persists you can then take it out, often the angle of the x-ray gives you distorted image that you are closer to the root than what it appears, Perhaps three D , can verify the proximity of the Implant to the root, test the vitality of the tooth,if its sore to the touch and pain upon chewing, the implant will fail,
Dr. Samir Nayyar
10/15/2015
Hello
First of all the reason i think for this problem is mostly due to the finger rest we take while drilling. Surgery should be done free handed for better control on angulation. Always take multiple x-rays at before each step to get rid of this problem. Sometimes improper positioning of the patient can also result in wrong angulation.
Now the best way would be to go for cbct and if the implant is away from pdl then leave it as such otherwise change the implant asap and insert the new one at better angulation. You'll have to do compromise with the current situation and patient didn't pay you for any compromises.
Best of luck doc.
J Bueno
10/15/2015
You're just fine. Use a custom abutment and the patient will be fine. Inform the patient of the less than ideal position, the pros and cons of another surgery to correct it or to simply leave it as is, and possible symptoms should the cuspid require future treatment as a sequelae of the implant proximity to the apex. But, you're fine.
Antigone
10/19/2015
You should be fine. The topic is very interesting and made me wonder on whether anyone has come across any papers on the topic. If you have seen any research on the topic please let me know. Thanks
Zafar
10/20/2015
It could be much further away from adjacent tooth than you think. Avoid high radiation and cost and take a simple vertical bitewing to see the spacing. That way you can get the results now rather than waiting for CBCT results.
Will Johnson
10/22/2015
Whew! Close, but still, not a cigar! If tooth showing no symptoms yet, leave it is my vote.
Wise dentists above admit to same situations. Nice looking device there should last 50 years!
Install the next implant!
Luci Rodell
10/22/2015
What if implants 28 and 30 are placed on mental foramen nerve or 1 mm away. Do u suggest bone grafting on another implant to build up tooth?
Third and fourth implant is 19 or 21.
Thank you
Do u refer to micro neurosurgeon if nerve damage is evident?
steve
10/22/2015
please make sure to contact me within a year when the adjacent natural tooth starts failing.
Jawdoc
10/28/2015
Monitor for any canine symptoms. If symptoms occur, root canal treatment of the canine might be needed. But in this case, u're probably alright. Angulated abutment needs to be used or U'll get a medial over-contour of the implant crown. What's ur resto plan btw? Implant-supported bridge (with a probable sinus lift posteriorly)? If so, why didn't you place the posterior implant too?
Cheers. Thanks for sharing your case.
SAM latif
12/3/2015
I would leave the Implant alone, if the tooth becomes symptomatic , I would take the tooth out and place another Implant without charging the patient for it,
Next time placing Implant, make use of the surgical stent.
good luck
JCF
4/19/2017
First Bicuspid implant placement can be deceptive as the root of the canine is often in a distal inclination. You think you are parallel to the canine root when placing your implant and end up with the apical end of the implant close to the canine. In this case your not directly touching the root so implant and canine health should be fine. I agree with our other colleagues removing the implant may damage the microcirculation of the cuspid and endodontic involvement. I would follow up with a PA in a year to check for any change in the bone on the apical portion of the cuspid and implant.
To avoid this take a PA when you first start your osteotomy with you pilot drill after several mm to check your orientation. This can happen even with a guided placement so always check your pilot drill position before continuing the full length of the osteotomy.
In my opinion this can be one of the more difficult implants to orient because you think you are parallel to the cuspid and have adequate distal clearance from a coronal view but you may need a slight distal orientation to your implant placement to keep it parallel.
I always look at the PA or CBCT just before placing my pilot drill to orient then check with radiograph. Thanks for posting your case it is good review and learning experience!