Patient with Throat Cancer: How To Approach This Case?
Dr. M asks:
I’d a like a second opinion please on this case. I have a patient, late fourties pretty healthy. He’s one of those patients where endo just doesn’t seem to do well. A few years ago I took a CBCT. We found some good looking endo tx, but large abscesses on several teeth. #14 and 15 were two of these teeth, one had been retreated. With class 2 mobility, and one with a draining fistula the prognosis was guarded. The endos looked great, that’s saying something when it looks great in a ct scan, and I could not find any missed canals. Gave patient option of trying apicos and retro fills or ext. If I could see poor endo I would traditionally retreat, but didn’t. Patient chose exts and, as he doesn’t have much money I thought it was a reasonable decision. So we removed the teeth and made a temporary partial denture.
A year after this he was diagnosed with throat cancer, 20% five year survival on average. Chemo and radiation were done and now he’s done with that. He is really unhappy not having his posterior teeth on the left. Two of the other teeth that had abscesses were #’s 2 & 3.
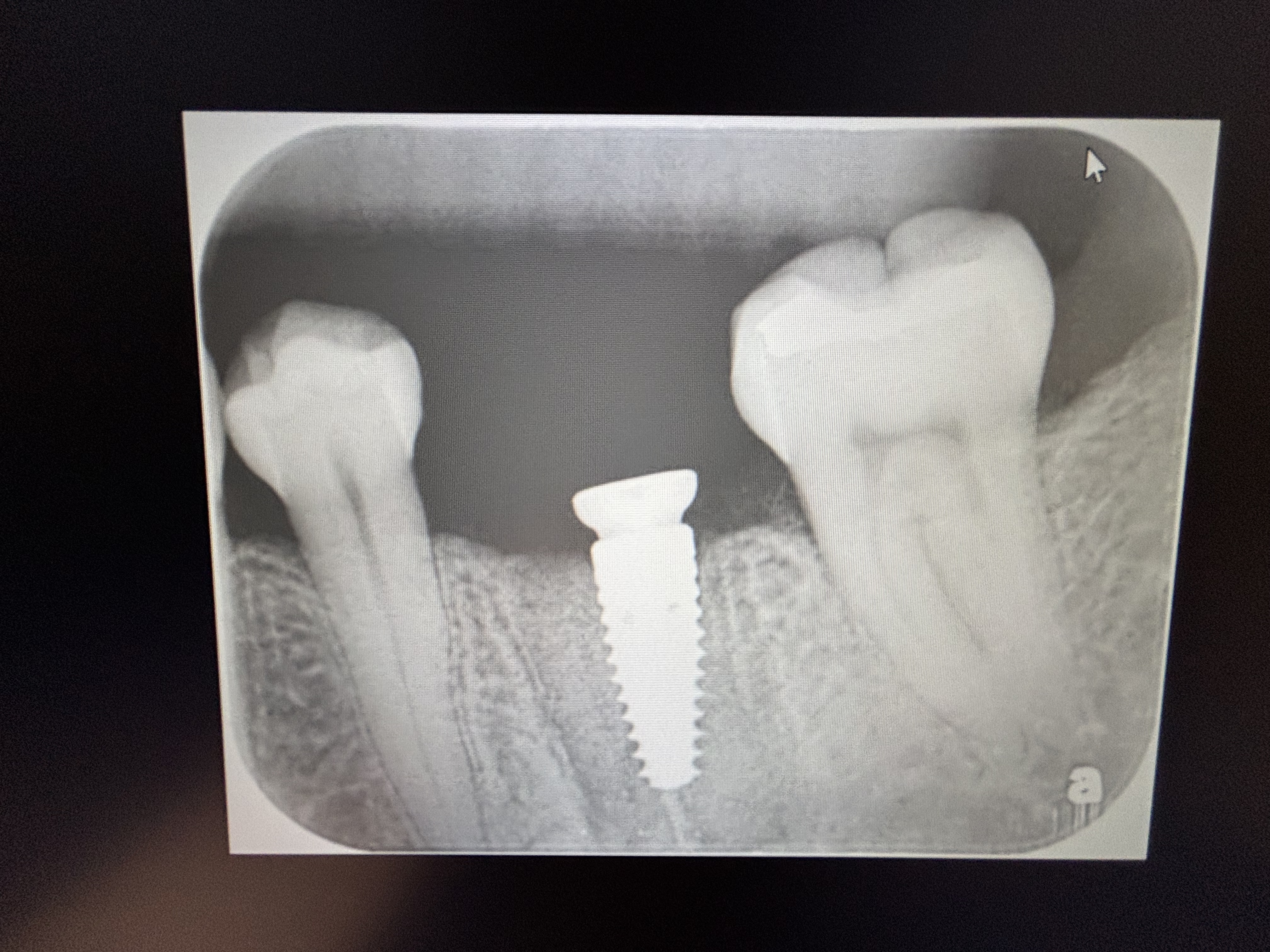
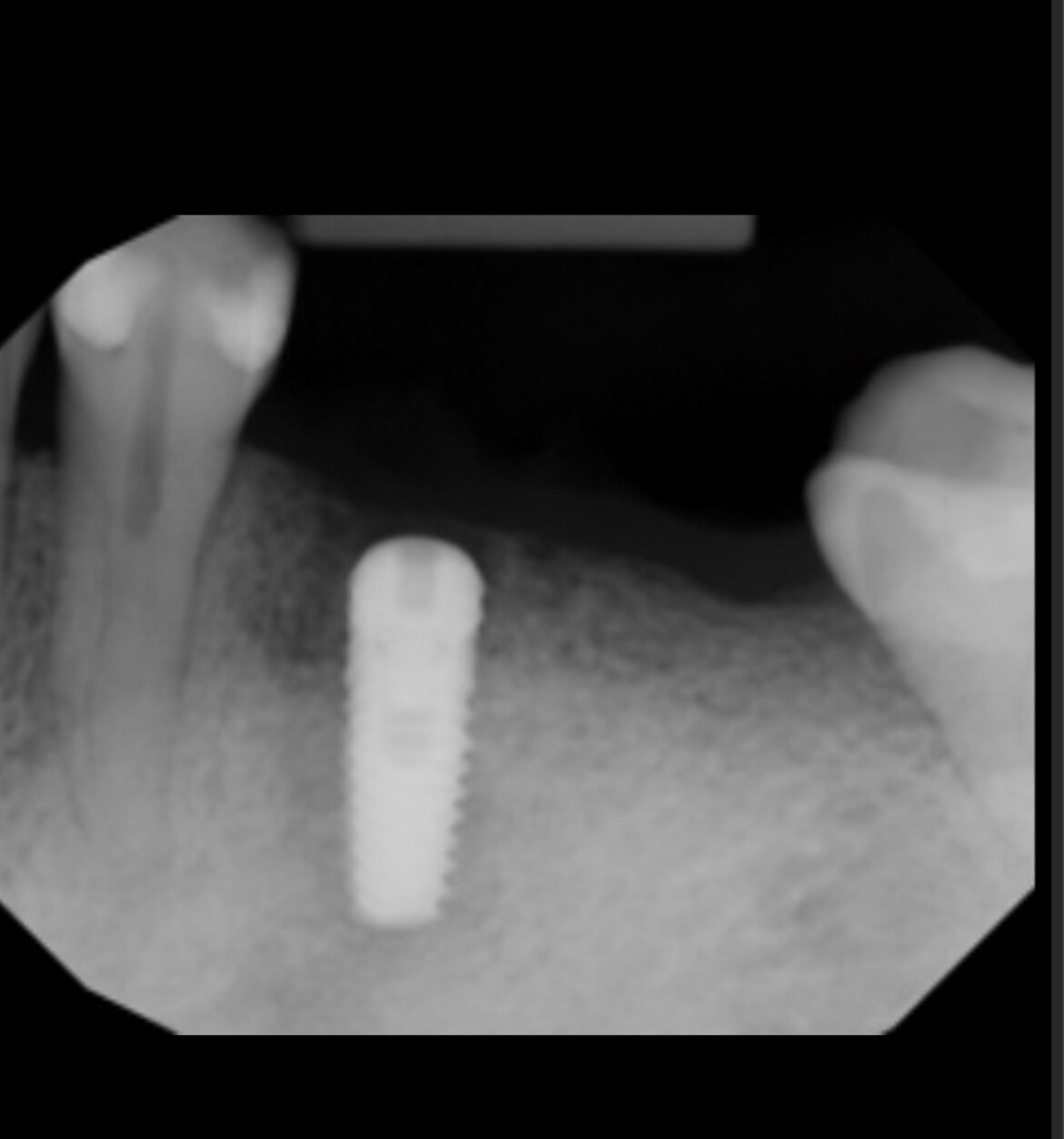
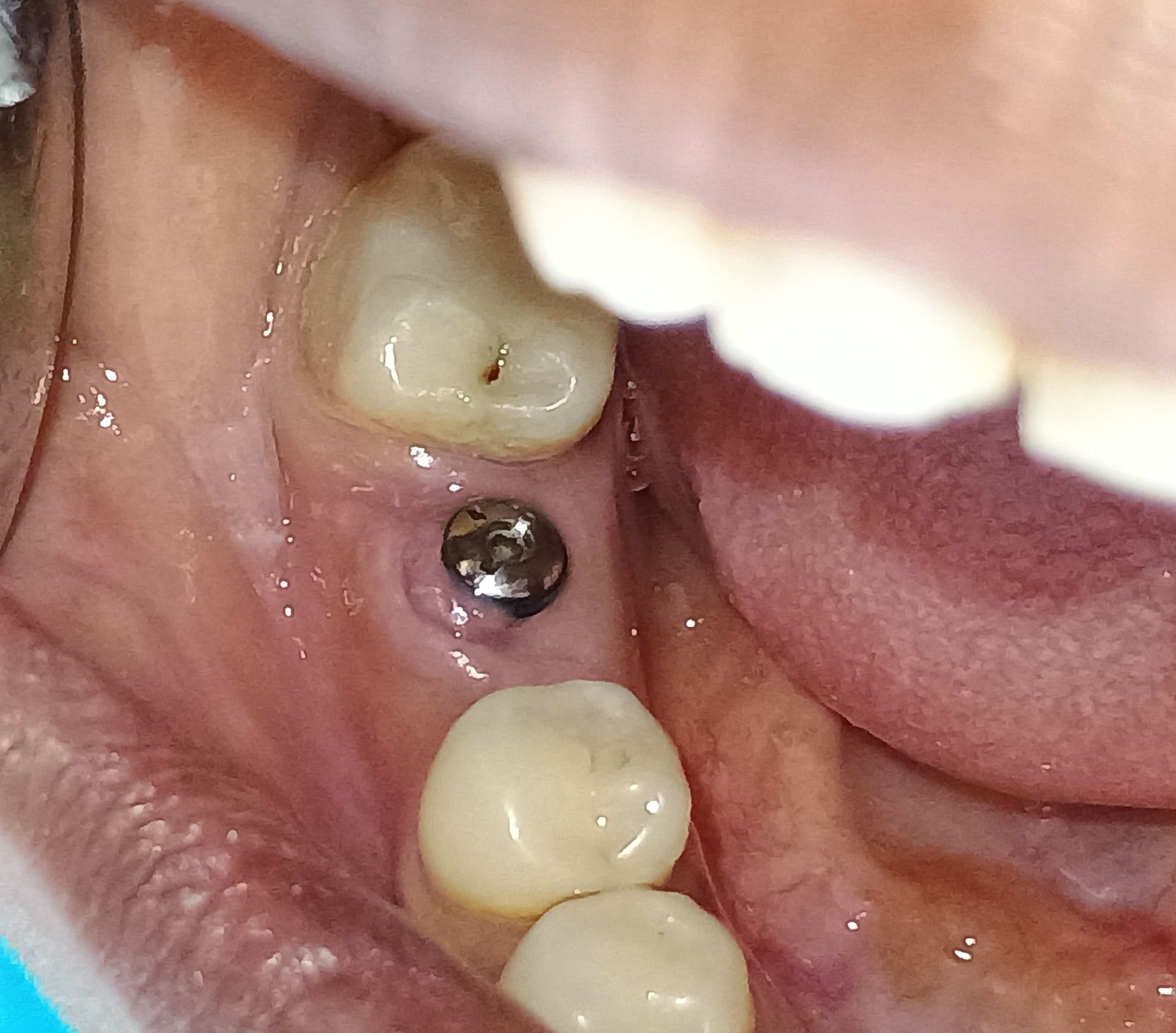
So here’s the question, do I insist he remove them? What if after the chemo and radiation his immune system was lowered and they are getting worse? PA’s really can’t show things and he is wary to have more radiation with another scan. I want to warn him in no uncertain terms of the risks, including life threatening infection/bacteremia and let him keep them, but legally I am concerned. Take a look.