Possible palatal perforation with bicon implant: recommendations?
I had a seemingly straightforward case of missing maxillary left premolars, for which I placed two Bicon implants just over four months ago.
As can be seen on the x-rays, there was a weird “dip” in the bone in the area of 25. This did not bother me at the time, as this part of the ridge was very narrow to begin with, but gets wider more apically, so I simply used the base of the dip as my depth gauge. This measured 15mm from the base of the dip to the sinus floor, plenty of space.
I tried to line the 24 up with the 23 and the 25 with the 26.
Directional pins were placed (one is angled, as I only had one 180 degree one at hand) depth and position looked right.
I trephined up to a 4.5mm final drill. I harvested less bone from site 25 than site 24. At the time I assumed the difference was due to a difference in bone density.
I placed the implants (both 8mm in length) with the Bicon mallet. Before doing so I scraped the osteotomy site and didn’t feel any perforations. Sutured and patient returned for follow up 2 days later. Patient wears a denture over the submerged implants and hasn’t experienced any undue discomfort.
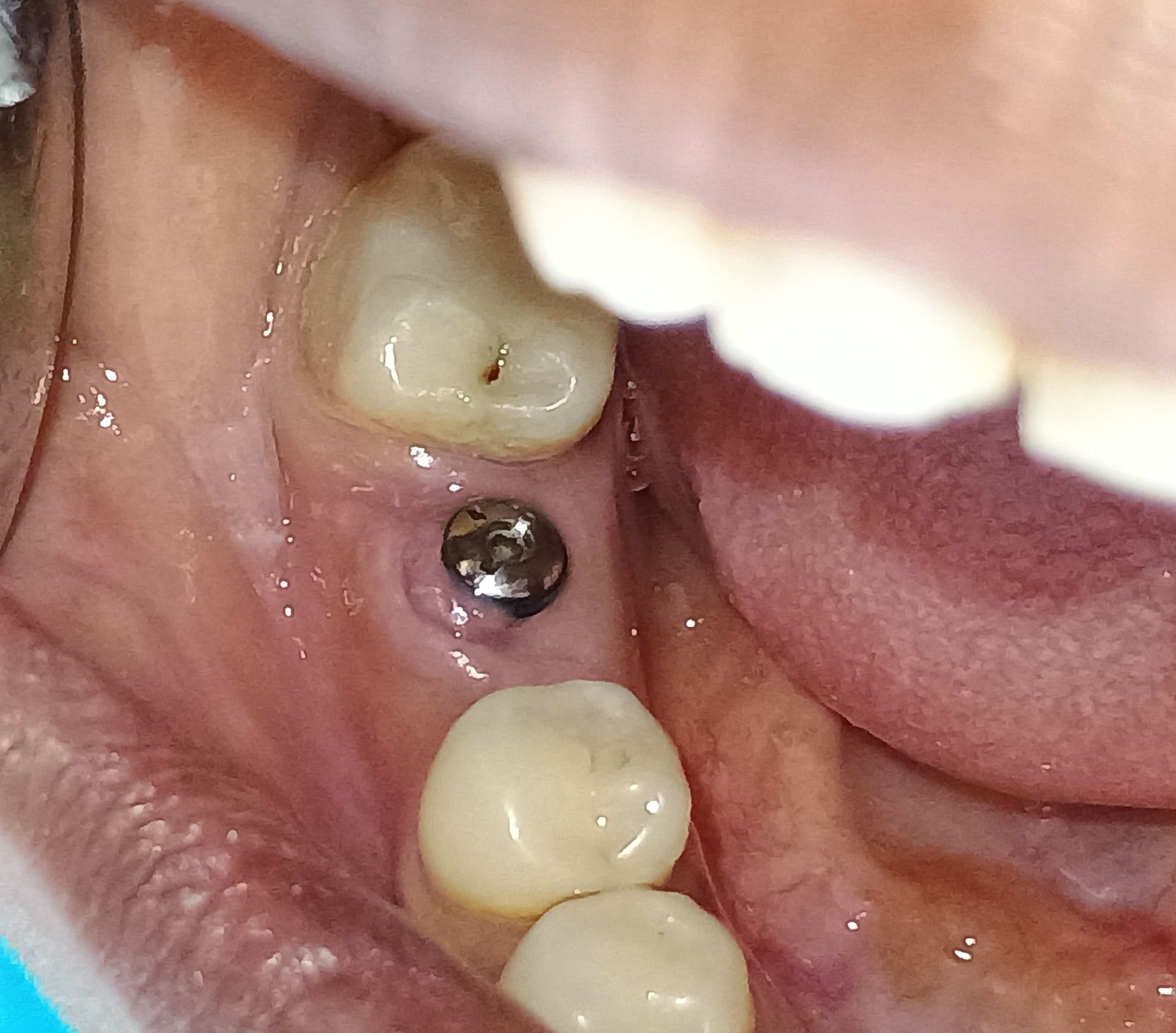
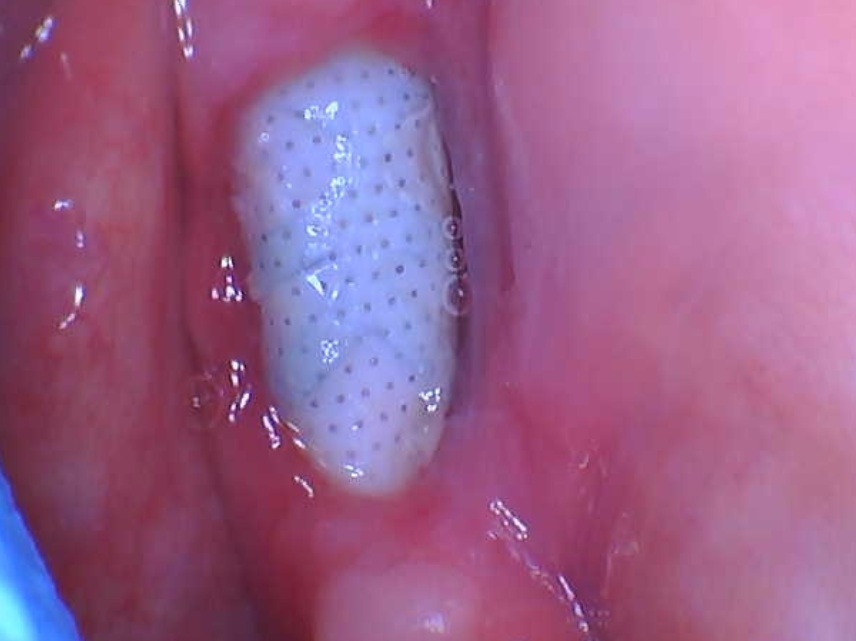
Four months later, the patient is happy, but there is plenty bone loss visible on x-ray around 24. Upon palpitation of the palate, the patient felt “something” when I pushed my finger in the area of the 25 apex.
My concern: I think I may have misdirected the drill, aiming too much towards the palatal, and with placement tapped the tip through the cortex. This could easily be verified via conebeam, but I would have to refer the patient for one and even if the outcome is as I fear, I have no clue as of how to proceed from there.
My questions:
– If the tip of the implant is indeed exposed through the palatal cortex, is it a significant problem?
– If it is not 360 degrees integrated, will loading dislodge it and push it into the sinus?
-Will the possible failure of the 25 influence the 24 which also experienced bone loss?
-Will loading the 25, even if it is partially integrated lead to ulceration and eventual exposure through the palatal mucosa?
-If the cone beam shows that my fears are realized, but in the absence of symptoms and with a seemingly stable implant, can I proceed with restoration and hope for the best? And restart when/if it fails in time?
-And if the implant fails, or the overall recommendation is to remove and restart, is there a way to remove a Bicon (fins, not screws) without a trephine?