Recessions of lower central incisors: comments?
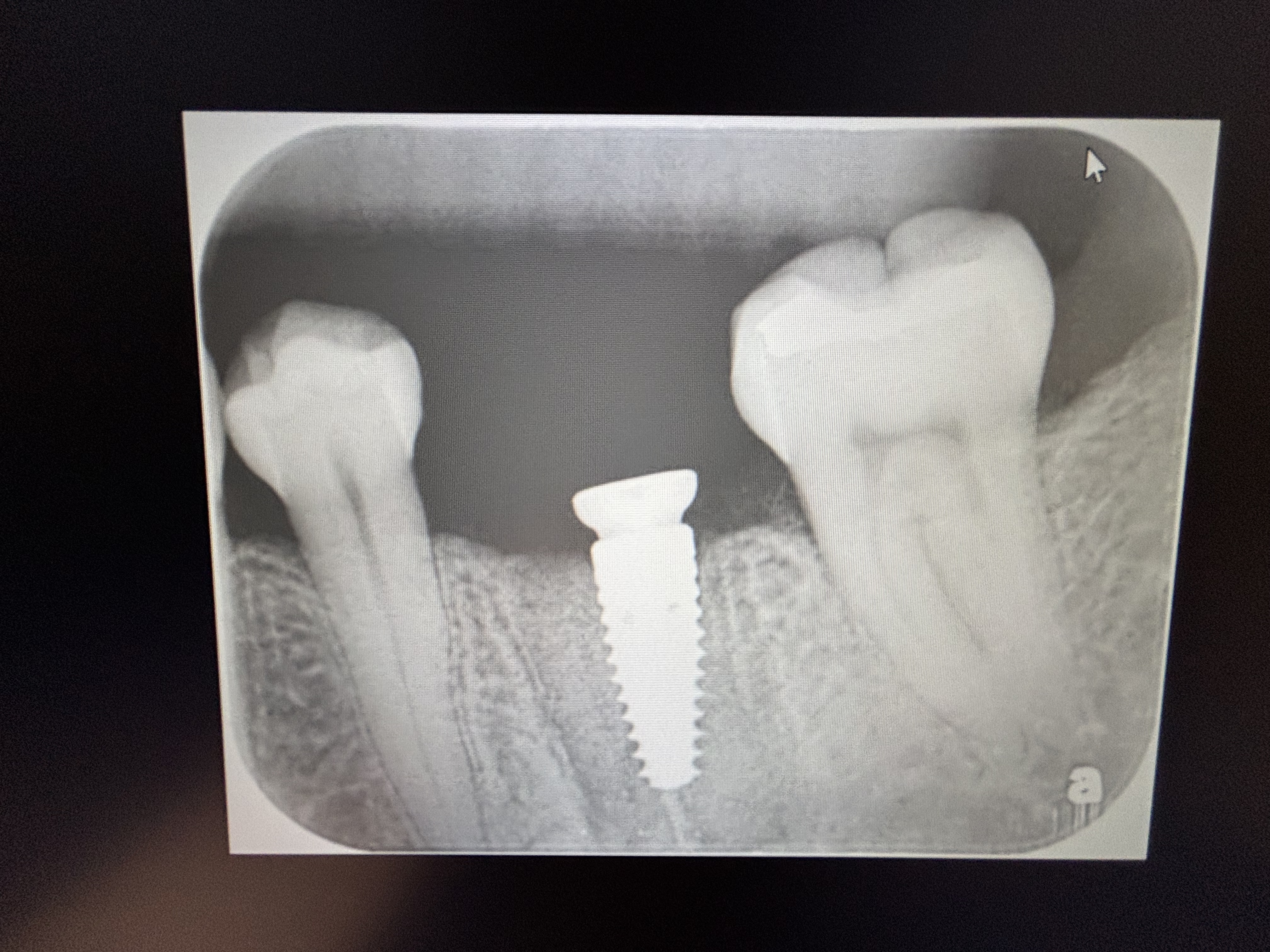
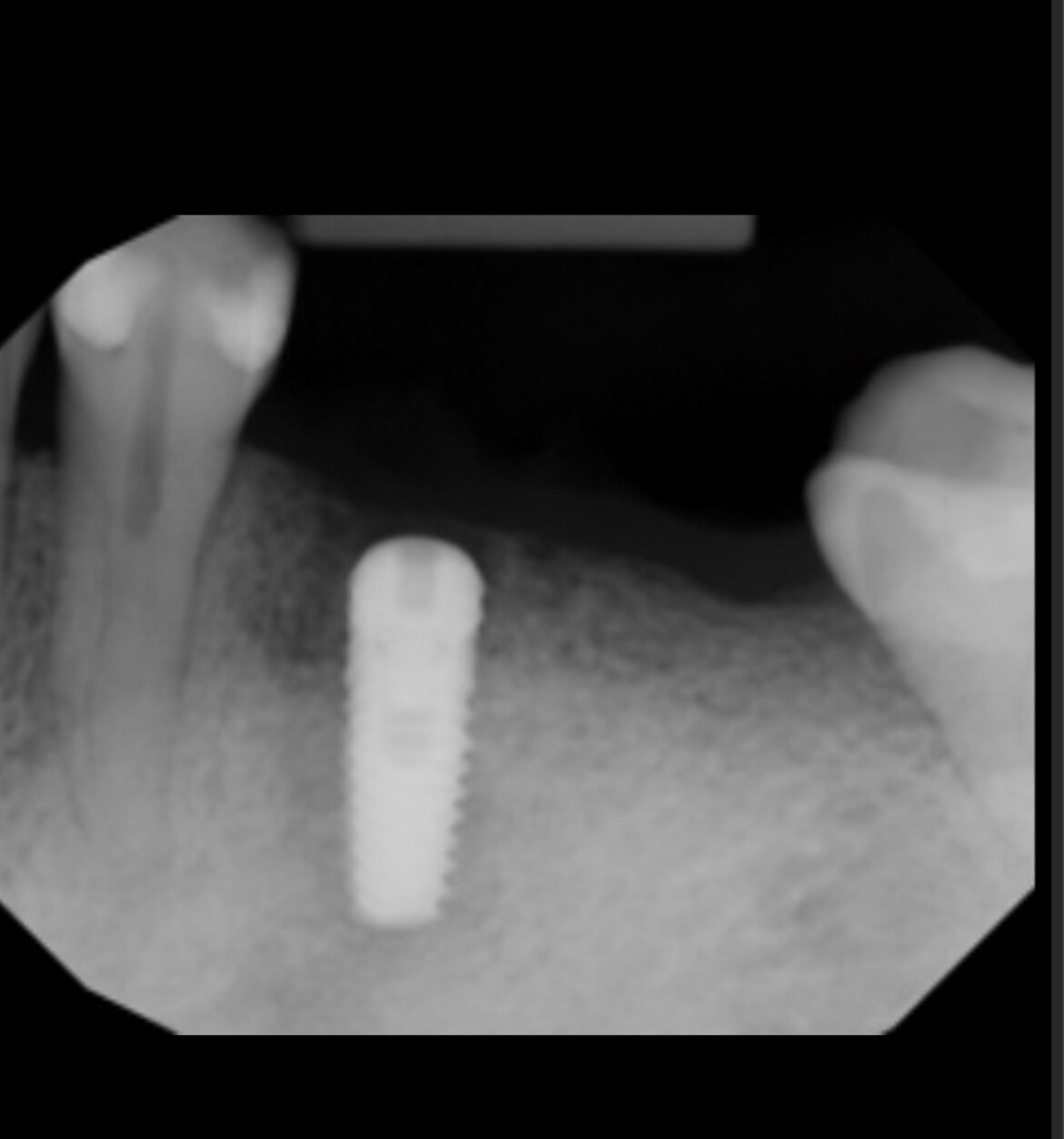
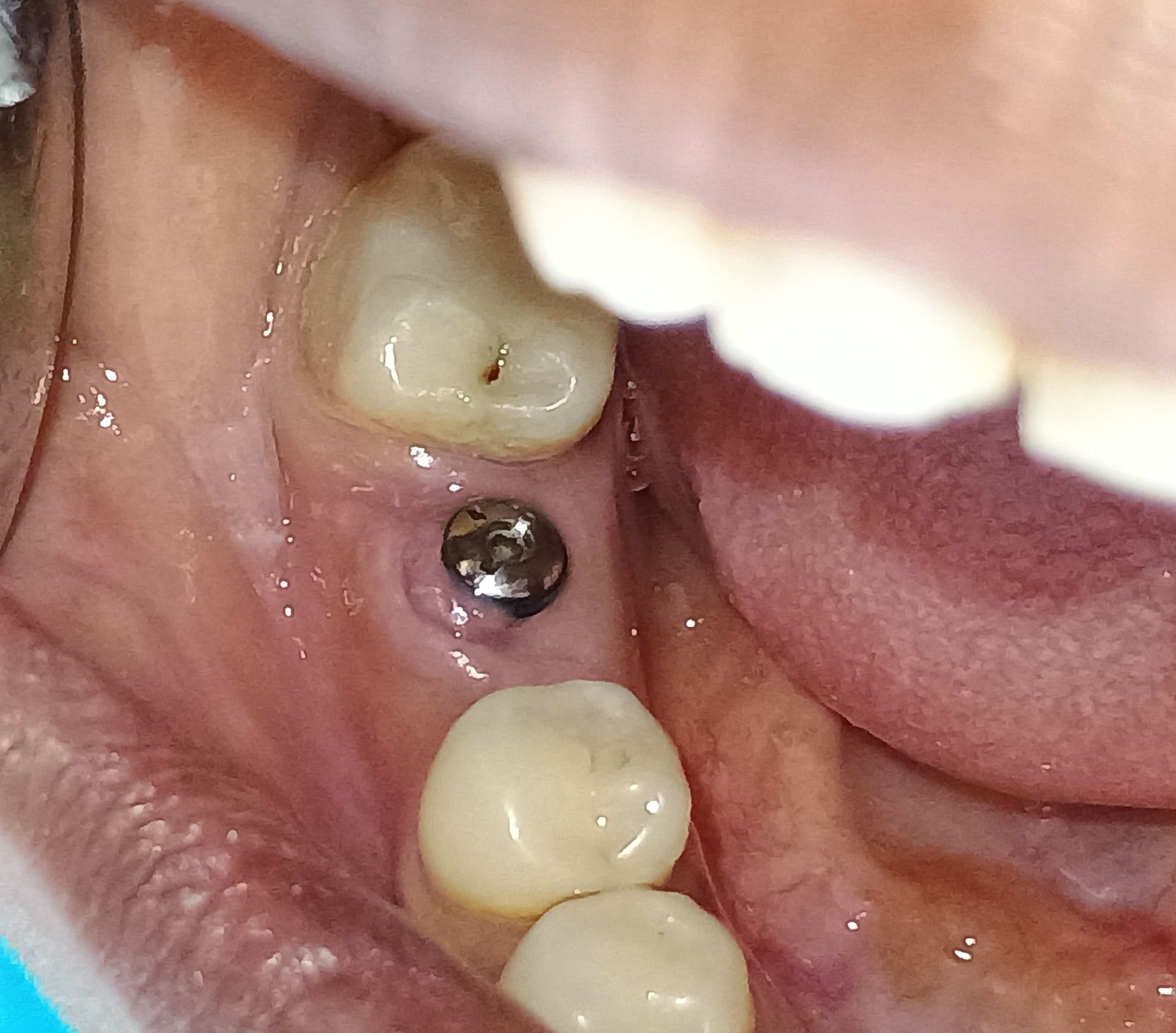
A 23-year-old female patient came to me with a complaint about gingival recession of her lower central incisors. The interdental alveolar bone crest is 6 mm below the CEJ. The teeth are slightly rotated. Please comment!
Thanks!



18 Comments on Recessions of lower central incisors: comments?
New comments are currently closed for this post.
Richard Hughes DDS
4/27/2018
Need more info. Such as prior Hx of ortho Rx, smoking and or substance abuse and diet.
Alan Merchanthouse, DDS
4/27/2018
My immediate thought looking at the photos is that these two central incisors have no space between them (roots) for good healthy bone or soft tissue to grow or be grafted back. Without careful orthodontic root separation, this area will continue to fail. But don't put the roots against the laterals either or the problem will just be moved to the adjacent interproximal spaces.
Don Callan
4/27/2018
This area has a very poor prognosis, I’d suggest removing the two teeth, as soon as possible cut your losses and make a bridge or do two implants. There has been too much damage to the root surfaces and there is no cementum.
Dorian Hatchuel
4/28/2018
Very extreme. Committing a 23 year old to a life long of anterior prosthetics.
Get more information first.
Sam Markzar
4/27/2018
I certainly agree with Alan . You can NEVER gain any bone , or soft tissue when there is no space , or even if the space can not be maintained. ( one of the main principles of any tissue regeneration) . The root proximity and the anatomical shortcoming will prohibit any successful outcome . .... and .. as far as placing 2 implants in this very same space of these 2 teeth will cause you another major failure , since the needed inter- implant space is even MORE than minimum interradicular space requirements. (Even if you use the narrowest Implants) .
I might suggest a thorough orthodontiic consult to check possible interproximal disking to gain space , or alternatively strategic extraction .
Good luck ðŸ‘
Dale Gerke - BDS, BScDent
4/27/2018
This is an interesting case and I agree an ortho consult would be wise. I have seen this type of situation several times previously and it was caused by a tight frenum and the mobility of lip. With the current case, it is not easy to see whether this might also be the issue but I suspect it is involved to some degree. I suggest checking this carefully since with the recession it is sometimes not immediately obvious that the frenum is involved. Previously on similar cases I have found when I released the frenum the problem was arrested (albeit the gingiva does not grow back). As well, you might want to check the vitality of the teeth since an "endo-perio" issue is a remote possibility. Clearly the lack of bone is an issue but I would not "jump" too quickly at extraction (unless advised by an orthodontist) and certainly not implants. Having placed many single implant bridges in similar circumstances, I have found that the emergence profile is hard to obtain, aesthetics hard to gain, and cleaning is difficult - sometimes impossible. Furthermore, after 46 years experience I have found that although teeth may look "terminal" from a perio point of view, in the majority of cases (with good oral hygiene) the teeth will last decades despite almost not bone being present. Lastly it would be wise to have the patient consult a periodontist in order to get their opinion. So... what I am trying to emphasise is that there are many points to be considered and haste is not wise. It would certainly never hurt to get opinions from different specialists so that both you and the patient can make an informed decision as to how to proceed.
Comlan
4/27/2018
What about getting periodontist consultation first before talking about orthodontic movement.
The etiology of the severe bone and soft tissue could well be orthodontic movement of the teeth. Need more information
This is class 4 gingival recession and there's close to zero chance of gaining bone and soft tissue with any procedure. Im completely against rushing to remove those perfect teeth for implant. Patient is just 23yo. What's the life span of an implant? 30-40 years success rate? Anyone knows? Nope
Those teeth from the lingual still have goo bone heigh. I will recommend refer patient to a good periodontist for management.
Soft tissue procedure done in 2 phases with EMD and some GTR would give an acceptable result.
Paul
4/27/2018
The patient is concerned or else would not seek help. A CT scan would definitely answer some questions and in a critical case that options is viable and important. The re is no doubt that the labial bone is very thin and possibly third molars may contribute to crowding. Rather than guessing the most prudent approach would be to evaluate the present condition and prognosis to exhaust all diagnostic options. Being well informed the patient will provide a reasonable response to any further options available.
Dorian Hatchuel
4/28/2018
There is adequate attached (masticatory mucosa). The problem here is tooth position. Consult an orthodontist to find the right teeth positions. Then re-evaluate the periodontium for ease of "cleaning".
Then consult a prosthodontist to ensure no Occlusal Disease is present. (Unless they are dogmatic about functional occlusion).
Very minimal treatment may be necessary.
Danev
4/28/2018
After consultation with an orthodontist, it became clear that it was the 1st tooth class. There is a slight crowding and a slight retrusion.
The following questions arise:
- Is complex treatment justified?
- Is it predictable?
- Who should begin: periodontist or orthodontist?
- Is it possible to gain interdental bone between 41 and 31?
- Are complications possible?
Danev
4/28/2018
The orthodontist proposes stripping of the upper and lower front teeth ! Is it justified?
Alan Merchanthouse, DDS
4/28/2018
I graduated from dental school in 1970!! Have been doing perio oriented treatment my whole career with great periodontists, orthodontists, etc. In '70's, a most likely treatment would have been extract and prosthetics, fixed or removable. But today with grafting, CBT scanning and implants in our hands, go conservative first. Try and save what was there originally - teeth! If preservation cannot be made to work, only then should an implant be considered. And only one, placed in the middle of the space where a lot of bone has been placed and made as healthy as possible. Then a screw retained prosthesis can be placed on the single implant located ideally. Finally, exemplary oral hygiene and followup forever. Two implants would fail fast due to a serious lack of space for them. One should be fine. And why strip upper teeth? That only makes the bite tighter. A little overjet would help this case. I find today too many dentists turning to implants as a first choice. They are not without problems and don't always last a lifetime. So if the implant(s) fail in a case, what is your next choice? More implants? Also, the patient needs a well padded checkbook as dental insurance will NOT take them very far. To borrow an expression seen on TV, I know a lot because I've seen a lot!! Also too bad this patient is so young.
roadkingdoc
4/28/2018
The X-ray posted and the clinical picture do not correlate in my mind. Are you sure you have the correct radiograph?
Danev
4/28/2018
The radiograph is correct, but the quality unfortunately is not good.
So I was not the only one
4/30/2018
So I was not the only one the suspected that they don’t jive
PA
4/29/2018
bone loss is not limited to these two teeth, even other teeth also invoved, check the etiology, (frenum,post ortho bone loss or any systemic factors with poor oral hygiene, trauma from occlussion),,remove the etiology and observe,if no improvement then perio graft
Julian O'Brien
4/30/2018
Academically it would be interesting if there had been a history of trauma or even an existing parafunctional protrusive bruxism. My head is denuded of hair follicles which, like the patient's gingival contour is not life threatening nor terminally progressive. Treatment of either "condition" involves a lot of perhaps unnecessary expense, pain and time whereas "living with it" involves simplicity. Only a hero would intervene unless there was evidence of pathology, progression or symptoms.
Sb oms
5/2/2018
Pic and x-Ray can’t be same patient - no way.
Perio consult