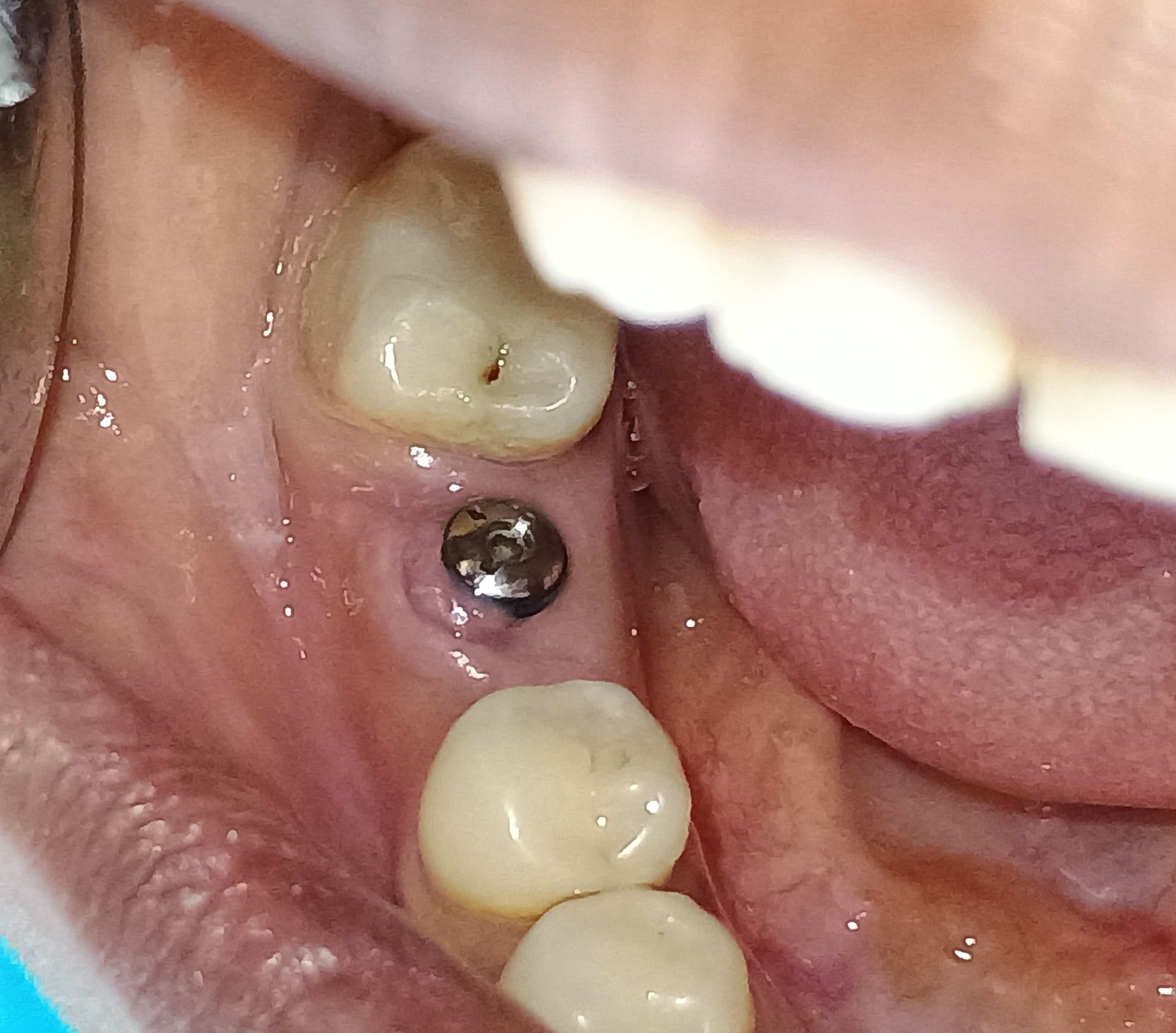
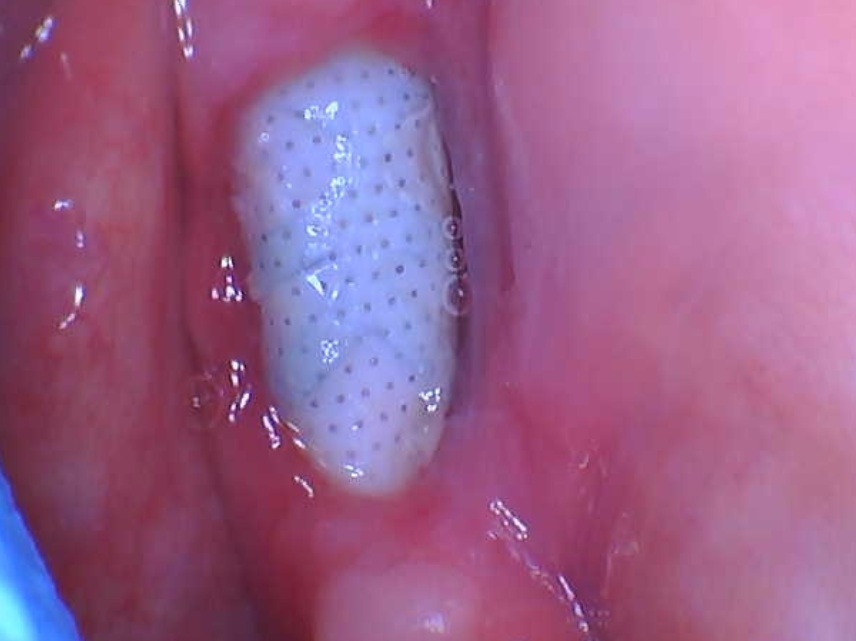
Soft tissue dehiscence 3 weeks after implant placement: thoughts?
I had placed 2 Nobel Parallel CC implants in the 4th quadrant in the premolar and molar region [lower right]. It was a straightforward case, I thought, and I also placed 2 implants in the 3rd quadrant [lower left]. The patient experienced severe pain for a week and came back to me with a soft tissue dehiscence. As the patient was medically fit, I advised the patient to leave it for 2 to 3 weeks and hopefully it would granulate. I put her on chlorhexidine rinses and hyaluronic acid application. She has come back today but unfortunately it hasn’t healed yet at 3 to 4 weeks after surgery. The other side has healed fine. I am thinking of removing this exposed part of the bone and covering with PRF. Thoughts? Any other ideas are welcome.
![]soft tissue dehiscence](https://osseonews.nyc3.cdn.digitaloceanspaces.com/wp-content/uploads/2018/10/8168-24-20181011_162724-bbf45279dacb-e1539261928620.jpg)