Vertical bone loss and possible grinder: Is a third implant over-engineering this case?
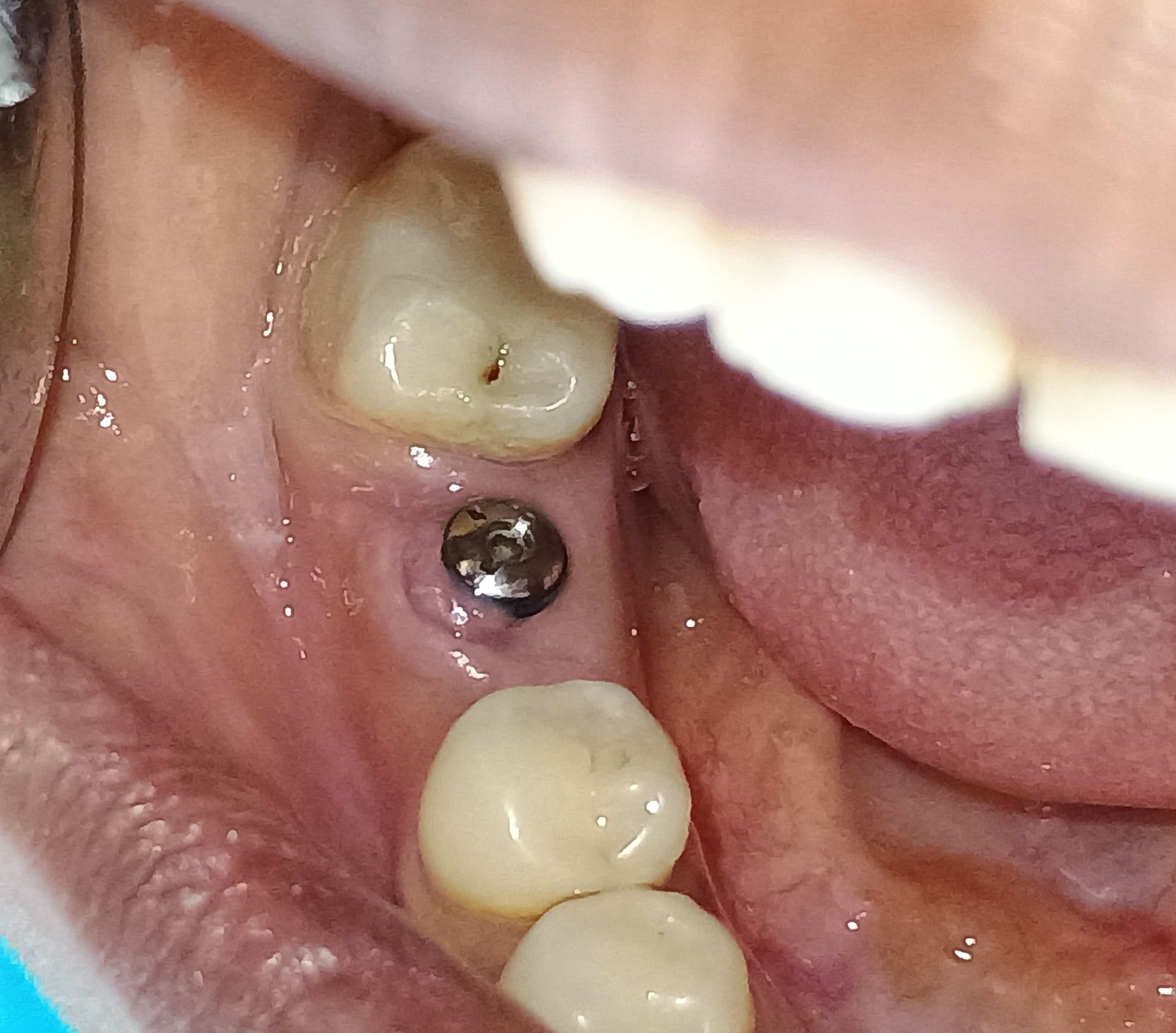
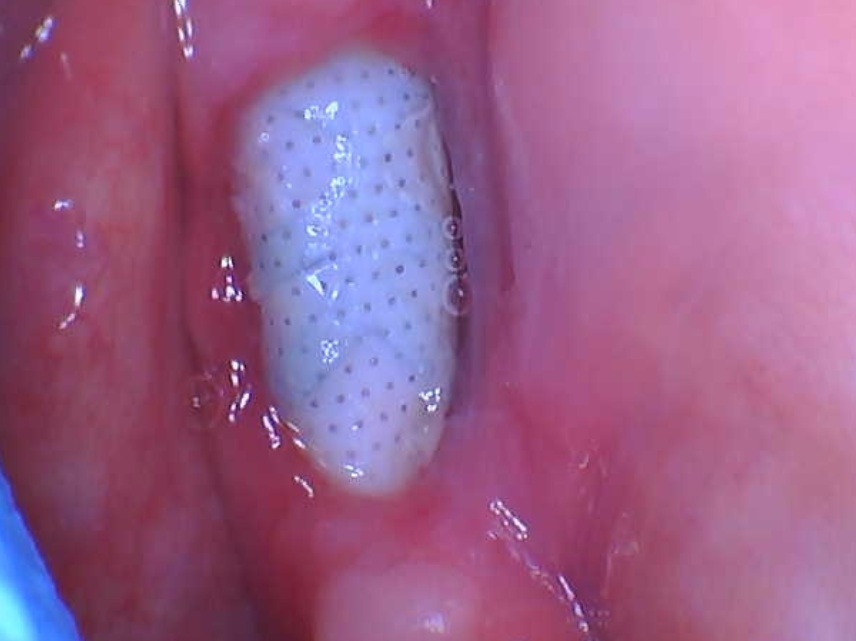
I have a 50 year old patient in excellent health who does not smoke and does not have diabetes. I have treatment planned for installation of implants in #19, 20 area [mandibular left first molar and second premolar; 36, 35]. The patient has significant vertical bone loss but declines a bone graft. I suspect that the patient also is a severe bruxer. I plan to install two 4.1 x 11.5mm implants and splint the crowns. I am also wondering if I should install a third implant in #18 site [mandibular left second molar; 37] and then splint all 3 crowns. Maybe over-engineering the case would compensate for the bruxism. What do you recommend?



46 Comments on Vertical bone loss and possible grinder: Is a third implant over-engineering this case?
New comments are currently closed for this post.
Justin
12/17/2013
Is there an opposing (#15) ? Its my humble opinion that the patient should get a full coverage HNG to mitigate the bruxism.
Mark D
12/17/2013
No, there is no #15. Please tell me what HNG is?
Justin
12/17/2013
HNG = Hard Night Guard.
Mark D
12/17/2013
Got it. Thank you!
HIMAKSHU
12/17/2013
Hi
If your patient is refusing to under go grafting , and you suspect he has parafunctional tendancies, do you really want to open yourself to implant instability and possible failure and then incur extra costs later if they fail and then do a graft ?
If he doesn't accept the graft, then refuse to do it and let him be not your problem but someone else's
Just a thought
CRS
12/18/2013
Remember that due to the Bruxism a patient actually gets pretty dense bone due to the forces on the bone, many even develop exostosis. There is plenty of bone there, if it were me, I would place two implants tenting up 2-3mm of bone with particulate graft probably a membrane over the top bury them and allow to heal. Then expose don't splint, hygiene issue, I like Zimmers due to the flat screw, often the bone will grow over the top and need to be removed at uncovering. Now here is the key, a balanced occlusion, bite splint and stress reduction for the patient. I would placed Botox if the masseter muscles are hypertrophied depending on your comfort level refer for that. That way you are treating the problem directly not relying on splinted implants in dense bone to fix it. And you're welcome!
Mark D
12/18/2013
CRS: My current plan, provided the anatomy, to put 11.5mm TSV. Are you suggesting to put may be 13mm and do GBR. Pardon my ignorance on the subject of grafting, but what type of material would you elect for this? Would FDB work. DO you think additional 1.5 or so mm of implant height would make a difference in the outcome. Would the quality of the new bone around the coronal part of the implant be better than native cortical bone around coronal part of the implant in current scenario?
Dr No OMFS
12/18/2013
Agree with everything that you have said but I am having a problem understanding the need for the grafting given the cross sectional films demonstrating fairly ample available bone height and width. What do you see (that I am not) as far as the benefit from the additional graft procedure and additional risks associated with it. Just curious - Thanks!
CRS
12/19/2013
What your missing is the bone height relative to the natural teeth,a better restoration can be planned. The crown won't be as long and will be easier to maintain. The graft would be replacing what was lost and it is a small amount of grafting to replace it. Remember that crestal bone loss will occur over time and fixing it at placement is best. Think like a regenerative surgeon not a dental technician. I see many of this deeply placed posterior implants with perio issues down the line. Dentists tend to look at the wrong place, it is about crestal height lost not the implant length and small corrections make a difference in the long run. And hopefully you understand occlusion and bruxism. Lastly make a scan appliance it needs to be done at the time of the scan not trying without to eyeball it with the implant software you will avoid problems in the future. Dentist tend to ignore the golden opportunity of placing the roots of your restorations in an ideal location based on the individual patient not implant software theses implants look a bit buccal but I can't tell since a scan appliance is not there. We learn this stuff in dental school implants don't change those principles but are an aid to what you already know. Your question demonstrates that you need to focus on the replacement of what was lost and future problems not the implant length; with implants the restorations come first that's the key. If you don't get appropriate grafting concepts the results are compromised and you will be scratching your head in the future, not best for the patient. I see a lot of cases where these steps are missed by dentists that are learning, this case is not easy for a novice since the right side molars will fail in the future based on the film. I always suggest performing within one's strengths and teaming with an experienced surgeon it is best for all and mitigates future problems. It puts the patient first. Thank you for your honest questions implants are not easy and we sometimes don't know what we don't know.
Mark Dankowski
12/19/2013
CRS, thank you. That's profound that you just wrote!!!
Dr No OMFS
12/19/2013
Thanks CRS - an excellent answer. Hard to argue that we need to treat to the ideal if the patient will allow us to do so. Unfortunately, not all patients will allow us that luxury and sometimes a couple of millimeters is just not enough of a difference for them to justify the added procedure and cost.
P.S. The SimPlant software will allow one to import an optically scanned model which can (at times) be preferable to a scan appliance. This would also negate the need to rescan this patient and allow for what you suggest (which I totally agree with.) Typically, one would take a PVS quality impression of the arch and make two pours (master and working model.) The master is optically scanned, imported into the software and indexed to the original CBCT scan via the existing teeth. This then becomes a virtual model which is used for the fabrication of the surgical guide. A clinically acceptable wax-up is then done on the articulated working model and this is also scanned and imported into the software. Both scanned objects (both models) are visible in all sectional views and in the 3-D rendition to assist with an accurate planning. There are many advantageous to this technique but that is beyond the scope of the space available and the interest of most. You probably were aware of this but Mark D may not be familiar with this option. Personally, I prefer this approach to a scan appliance in most cases.
Mark Montana
12/17/2013
Studies show loss of the 2nd molar have little impact on the stability of the remaining teeth, therefore replacement by implant is not recommended unless a specific purpose is defined (opposing tooth, bridge abutment) or a patient requests it. Therefore, I would probably not plan for it.
With regard to the bruxism, adding the second molar will have no real benefit. Also, if bruxism is diagnosed by tooth wear, be aware that the loss of occlusion on the side in question may result in increased pressure on the remaining teeth. Often the result is accelerated wear.
Mark D
12/17/2013
Very interesting so far. Waiting for more input. Appreciate it!
Dr No OMFS
12/17/2013
Over engineering is usually good in a bruxer but would only place implants that will be opposed in function. If #18 is opposed than it should be a consideration if you have the bone volume and mandibular opening allowing you to placing it. Just curious, why the 4.1 diameter instead of the 4.8 (or larger) and why not a wide neck in lieu of the bone level for the molar (if you are using Straumann)? In your SimPlant w/u it would appear that you have plenty of room for a larger diameter implant.
CRS
12/19/2013
The Straumann transmucosal is an excellent idea to help with the crestal bone height issue. They are technically more difficult to place for a novice but are great in dense bone. I wish I had thought of it!
Reg O'Neill
12/17/2013
You are correct in the assumption that by placing additional implants it is possible to compensate for additional loading forces, however both mandibular flexure and torsion can be significant in a heavy bruxing patient. Given that maximal flexure will be distal to premolar area it would be wise to consider premolar units separate to more distal implant crowns. You have not detailed any opposing occlusion or occlusal analysis apart from your "suspicion" that he is a severe bruxer. I would suggest it best to confirm such a diagnosis categorically at an early stage in planning as it will determine at the very least, your implant design, implant number, position, restorative materials, maintenance issues (biteguards etc) contributing to overall long term success or complication risks. In the absence of such diagnosis you will find it difficult to defend any later accusations of negligence. Despite "significant vertical bone loss" you can plan 11.5mm length implants. Your excellent CT imaging shows very clearly an adequate ridge form with a low alveolar nerve complex. What would you be grafting? Thankfully your patient has declined your offer! My humble advice is to continue with your diagnosis prior to plannng. If you co-diagnose with the patient they will generally accept your recommendations but of course this is reliant on accurate diagnosis - not available by loading up a CT image and using a computer aided on screen implant placement. You could have a rewarding case here, ask an experienced colleague to work with you and best of luck
Mark D
12/17/2013
Very valuable, thank you so much, Reg O'Neill!
Mark D
12/17/2013
I may consider 4.7. All I place is Zimmer Tapered ScrewVent.
Dr No OMFS
12/17/2013
A lot of ways to over engineer a case and increasing the implant diameter (where you reasonably can) is one of the easiest. I know that Zimmer makes a 6.0 diameter in the TSV series and would think about that for the molar. Watch your peri-implant bone density go up in the SimPlant stats as you approach the cortical plates with a wider implant. I don't personally like second molar implants but have done them to disperse occlusal forces over more teeth. I also don't like splinting if for no other reason than it creates the usual hygiene issues - I always try to look for a better answer. Lastly, if your patient is truly a bruxer, you could "consider" Botox in the masseter muscles as one of several remedies to reduce occlusal loading. Best of luck!
Mark D
12/17/2013
OK, very good! I'm certainly considering at least 4.7X11.5. What do you think about increasing osseointegration time?
Dr No OMFS
12/17/2013
Increasing the osteointegration time beyond the manufacturers recommendation will probably not do you to much good from what I have read and seen. Progressive loading "after restoration" will increase the bone density around an implant but that won't do you much good if your patient is bruxing hard on the implant prosthetics from day one. One option is to initially place provisional restorations slightly out of occlusion to prevent bruxing on them for a period of time, but still allow for some functional masticatory loading. After a few months, these can be converted to traditional restorations. This can backfire if the patient won't tolerate the lack of occlusal contact - but since he is missing these teeth currently it has a good chance of working and might be worth considering.
Another option, from a loading standpoint, is not to place two implants (bicuspid and molar) - place "three" implants spaced for bicuspid sized teeth and restore them individually. In effect you now have three implants supporting roughly the same occlusal table area as two with the single bi/molar scenario. Placing a bicuspid and "two" molars can do roughly the same thing. Unfortunately, the only way to take advantage of the additional second (posterior and unopposed) molar for loading support is to splint everything together. Again, splinting is something I personally try and stay away from if possible. Just some thoughts IMHO.
Mark D
12/17/2013
Guys, I have not heard anything about increase in osseointegration time from you. Any merit to that?
Mario K Garcia,DDS
12/17/2013
In response to you question; A few insights
1- I believe that implants (fixtures) replace the roots of the missing teeth. So if you are going to replace a bicuspide and a first molar and no second molar is present (open ended) you should really place 3 implants. Even if the upper second molar is missing. Remember; molars on implants are like bicuspides in shape.
2- When treatment planning patients that have para-functional habits; we need to augment the bone to implant contact in order to compensate for the para-function.
3- When the existing bone height is compromised or reduced; more implants (BIC) needs to be planned to compensate for the enlarged crown height space.
Based on these 3 recomendations and to assure a long term success of your case; go with the 3 implant plan. Even more so, if no anatomical structures are compromised.
In any case if you have 3 implants and one fails; you may still have a chance of success. But if you place 2 implants and one fails: then what?
Thank you for subminting your concern and accepting my humble opinion.
Good luck and happy holidays.
mike shulman
12/17/2013
Interesting, no suggestions on prosthetic, What material would be suggested for the restorative? PFM (metal occlusion), zircon (super popular) or?
Thanks
Vipul G Shukla
12/17/2013
Dr. Mark D,
What we sometimes suspect as a bruxer could just be a patient chewing well on one side of the mouth for many years and showing the corresponding increased wear due to unilateral function. Other times, we see the results of bruxism from a younger age.[Maybe he is divorced from his stress now ;) ] What you need to check for is masseter tenderness (you can palpate this) especially in the morning for night-time bruxers and late afternoon tenderness in the Muscles of mastication for daytime clenchers and grinders. Unless you can confirm whether this guy is an active bruxer a third implant is simply increasing your work load and the patient's cost.
I would most definitely consider wider diameter implants in this area, even 5.0 or 6.0 mm, lengths dictated by the anatomy.
Increasing the time beyond three months is usually not necessary, and research from the Straumann ITI group actually states that the final cortication of bone only happens once you start loading them after say 2-3 months. Good old Wolfe's law.
Nice case. Good luck!
Mark Montana
12/17/2013
In the early '90's the push was to use wider and wider implants, the common sequelae was bone loss due to over-thinning of the buccal bone, compromising bone supply. Therefore, we should not be so quick to suggest a random diameter without knowledge of the bucco-lingual dimension. Better a modest diameter than exposed buccal threads.
Vipul echos my comment about suspected bruxers, diagnosis is needed to separate them from patients suffering from shortened dental arches and those with historical damage.
In 2013 (almost over), with 95% success, we really shouldn't be thinking of placing an extra implant in case one fails.
Dr No OMFS
12/18/2013
Yes, in the 90's it was commonplace for many to "oversize" implants which would cause the sequelae that you describe. That is different from "optimizing" the size of the implant for the existing anatomy. With existing CT imaging and software, one should not have to guess and use a sub-optimal diameter implant just to be safe. Why would that make any more sense than placing an extra implant just in case one fails which you criticize? Mark D has the CT, the software and the responsibility to determine what that optimal implant diameter is. Given the case description, why would it be wrong to maximize the implant diameter, loading tolerance and thus the ultimate success potential? I would feel that we need to learn from past mistakes and do things because they are reasonable, predictable and relatively safe. Larger diameter implants are, indeed, sometimes indicated. And yes, I do agree, the integrity of the buccal plate is paramount.
B. Milligan
12/18/2013
Just curious about the mandibular right and the patient's total occlusion. I would be very concerned with the patient's total occlusion. Have you discussed this with the patient- looks like there will be/are significant problems on the right. What is the patient's comprehensive treatment plan?
Mark D
12/18/2013
I know it looks drastic on CT but the right side is in relatively good shape. I think you see apico done on #30 that throws things off.
Peter Fairbairn
12/18/2013
Hi Dr Mark D , both the last two posters have hit the nail on the head , loading earlier may be of benefit rather than later . As you know when you break a leg skiing you do not lie in bed for 6 months to get "a better " healing , no earlier function improves regeneration in the ethos of Woolf .
As to Dr Montanas response , increased width is not the answer but mangement of the bio mechanical forces . By increasing the width of the Implant we are reducing the amount of residual host bone and increasing the chance of exposing buccal threads which may result in issues later if there is reduced attached gingiva.
The final issue to think about is the properties of the Ti Implants which flex ( all systems have a weak point or stress riser where the bio-mechanaical forces are managed through flex ) . Thus going wider or splinting may be counter productive to this force management .
We can often see bone loss on one implant when the Implants are splinted due to a number of factors including co-axial forces from the splinting .
So best ia to keep it simple and deal the the bruxism as you normally would using hard splints or Botox .
Peter
Dr Bob
12/18/2013
There are now very strong lab processed composite restorations that are milled or built. These restorations unlike harder materials will wear and self adjust as the natural teeth wear. It is not a substitute for failure to correct and stabilize an occusal problem, but could be used to reduce stress on the implants. It is like using a shear pin on a boat prop to protect the more costly and difficult to repair parts from breakage. Discuss there materials with your lab it may or may not be what you want for this case, however, you will find uses for these materials in implant dentistry even if just for transitional restorations.
Mark Dankowski
12/18/2013
So far I'm finding everyone's posts to be incredibly stimulating. I will welcome more. Thank you, all!!!
Melissa
12/18/2013
Great suggestions.
Something to considered now when you have a possible bruxer..... Studies show now, that they are all sleep apnea patients, they are related.
So what do you treat? The night guard will nly block more the airway.... Have to find degree of apnea. There are some questions about there sleep quality, exam findings ,
......in their mouth, neck size, tired? Wake up at night?.... There are many dentist now that treat sleep apnea.
Good luck
Mark Dankowski
12/18/2013
Melissa, your comment prompts me to think about getting more training.
Dr Bob
12/18/2013
SILENT NITE a snoring device (there are others also) that many dentists provide for patients that have a spouse that complains about the noise keeping them from sleep. It does work. Similar devices are available that are for sleep apnea. Be careful because sleep apnea is a medical condition that can kill. SILENT NITE is not specificly for sleep apnea and should not be sold as such. It does provide airway opening by positioning the lower jaw slightly anterior. It also serves as a night guard at the same time. If sleep apnea is suspected please refer if you are not trained to test for and treat this condition.
Richard Hughes, DDS, FAAI
12/20/2013
CRS, you brought great points to consider. Looks to me that the bone loss on the posterior right is due to the loss of teeth, etc. Bruxing is certainly a major issue to mitigate. Bruxing has been the major reason for the loss of teeth, bone and restorations through the ages.
To say that this bone loss pattern is due to bruxing is questionable.
I would not bother in this case with grafting. For one the patient does not want grafting. So use Bicon implants. If there was more vertical loss, then a ramus blade would work wonderfully with a FPD abutted to #21 and #22. Especially the ramus blades from Pacific Implants, Inc. They have a tremendous amount of load bearing area.
I would rather have a mind open with wonder, than closed by belief!
I know that blades are against some peoples belief systems, but they can make a case like this work very, very well!
CRS
12/20/2013
Richard help me out on this one, when I look at a case with a discerpancy in the crestal height is there a rule if thumb if how deep you can place an implant without added bone to correct the crest discrepancy with the natural tooth. I'm not talking about the implant length but the loss of crest when restoring the implant crown. I get the crown root ratio but I'm concerned about the hygiene and perio issues with the natural tooth. Am I stressing out about this seemingly minor amount of bone I add which I roll into my implant fee? I love it when I see bone almost covering my cover screw at uncovering and I know with some implants we get some dieback over time. What are your thoughts?
Richard Hughes, DDS, FAAI
12/20/2013
CRS, I'm not sure if I understand the question. There is no rule of thumb per say. Yes , implant/crown ratio is a factor!
I look at the potential success of the bone grafting. Duration of treatment and cost. I know Hilt Tatum with his concepts of vital segmented osteotomies is changing treatment methods and goals. But this is catching on slowly. We do not always get patients with ideal conditions.
If your considering placing the implant and then tenting ok. But grafted bone is not the same as real bone and bone has its epigenetic potential.
I too am concerned with perio and hygiene issues. I am also concerned with phonetic issues.
On some cases I do add a particulate (OsteoGen) atop the implant and a slurry of OsteoGen in the osteotomy prior to implant insertion.
It's nice that you care about quality. I do too.
As per the loss of stress when restoring the implant crown, I think its an implant design issue, some is occlusion, some is cement, some is due to the occlusal table width and cusp height and inclination.
As a surgeon some issues are out of your control. They are influenced by the restoring doc. I perform both duties, so I am dogmatic about the occlusion and prosthetic design.
You can perform great surgery, all to have it compromised by the restorative phase, not to mention the patient. I have a patient that bruxers like the dickens ( broke three bars, broke his overdenture numerous times, the same healing collar always backs out when his OD is in the lab for repair. He is an outlier. I recently sent him to an OMS for Botox. I have ruled out hyperocclusion. He has a most over active parafunction. He owns this!
So we as Doctors have to accept that we can do out job as best as possible but the patient is going to do their thing.
Don't be so hard on yourself.
CRS
12/20/2013
Thanks for your insight and wise words, I appreciate your advice.
Richard Hughes, DDS, FAAI
12/20/2013
Another implant to use for the rehabilitation of this area is the Quantum implant. Quantum is based in Plantation Florida. It's like a Bicon, but twist in. It has an internal well built into an external hex. Either way it has minimal if any micro movement or leakage.
sb oms
12/20/2013
I would use Straumann standard implant. 2.8 mm polished transmucosal flared shoulder to 6.8mm diameter. A great fixture for cases like this. Brings the implant abutment junction higher up and has a very natural tissue friendly emergence profile. Don't make a wide occlusal table.
I would not graft the crest here. I don't think you get anything but trouble and uncertainty with no longterm added benefit from trying to graft the crest with a tent approach as was recommeded.
Don't splint the crowns.
Lots of cases like this with longterm success (well maintained and parafunctions managed appropriately of course)
Gerald Rudick dds AFAAID,
12/25/2013
Mark D, you are obviously a very caring dentist and the comments offered above are all very worthwhile.
Dr. Joseph Choukroun, of Nice, France, well known for his work on PRF, makes an important point on implant success based on a patient's Cholestrol levels.
In the case you present, we are told that the patient is 50, has no diabetes, non smoker, and generally healthy........we have not been shown the opposing teeth, we do not know the sex of the patient, nor are we sure of the blood chemistry...so there are a lot of variables.
There is no such thing as over-engineering when it comes to dental implants......if they are well spaced...more is always better. When the implants are allowed ample time to osseointegrate, do place acrylic temporary crowns, that will allow the implants to be in function, with a lighter load....bruxers always present more problems than people who do not exhibit parafunctional habits.....perhaps Botox injections into the muscles of mastication would lessen the forces......leave the patient in temporaries for 12-18 months....and if successful, then do the final prosthesis. .... if there is a failure, the patient did not spend a lot of money for expensive crowns....temporaries can be made chairside, with no lab fees.
Mark D
12/25/2013
Garald, very valuable, thank you!
rokoba
12/28/2013
Bruxism is an indicating factor of the need of new implant post materials. Titanium has not the isoelasticity of bone.
And even bone has not the same in all areas.
Some of the possible risks are not predictable. Imagine non-bruxer getting in divorce or other problems and you just find out when implants and teeth tilt.
You can not avoid risks and are not responsible for everything.
As you know having a bruxing patient my
statement is: additional implant regio second molar is mandatory-as this is more resistant against resorption in comparison with second premolar region. And, progressive loading.
Good luck and help us god.
Helpfull recommendation for the patient:
more sports activity usually reduces bruxism activity. Compensation of hereditary phylogenetic "decompensated" behaviour.
Oleg Amayev
10/16/2017
Based on these Xray I don't see significant bone loss.
Can you tell me how you planning to add bone vertically if patient will say YES?
If patient is a bruxzir then have these two implants splinted with Bruxzir zirconia crowns.
Also when you planned Implants on your CT did you have teeth wax up made or at least did you placed virtual teeth from that software in order to properly align these implants with this teeth? This is just my recommendation if you didn't do it. Good luck.
Oleg Amayev
10/16/2017
Yes, I see the teeth on Ct, i didn't see it before, sorry.