Failing bridge due to internal resorption: thoughts on treatment plan?
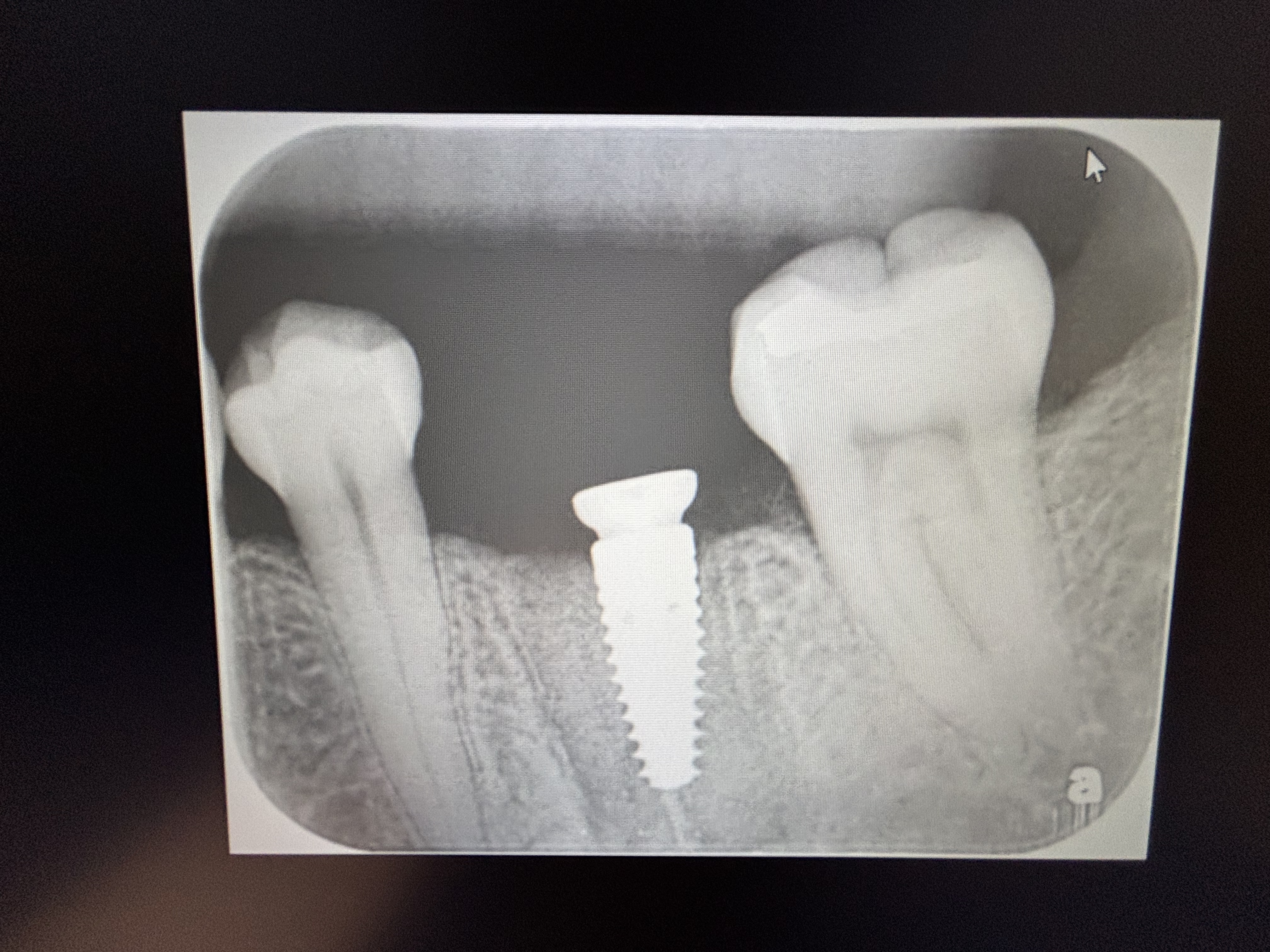
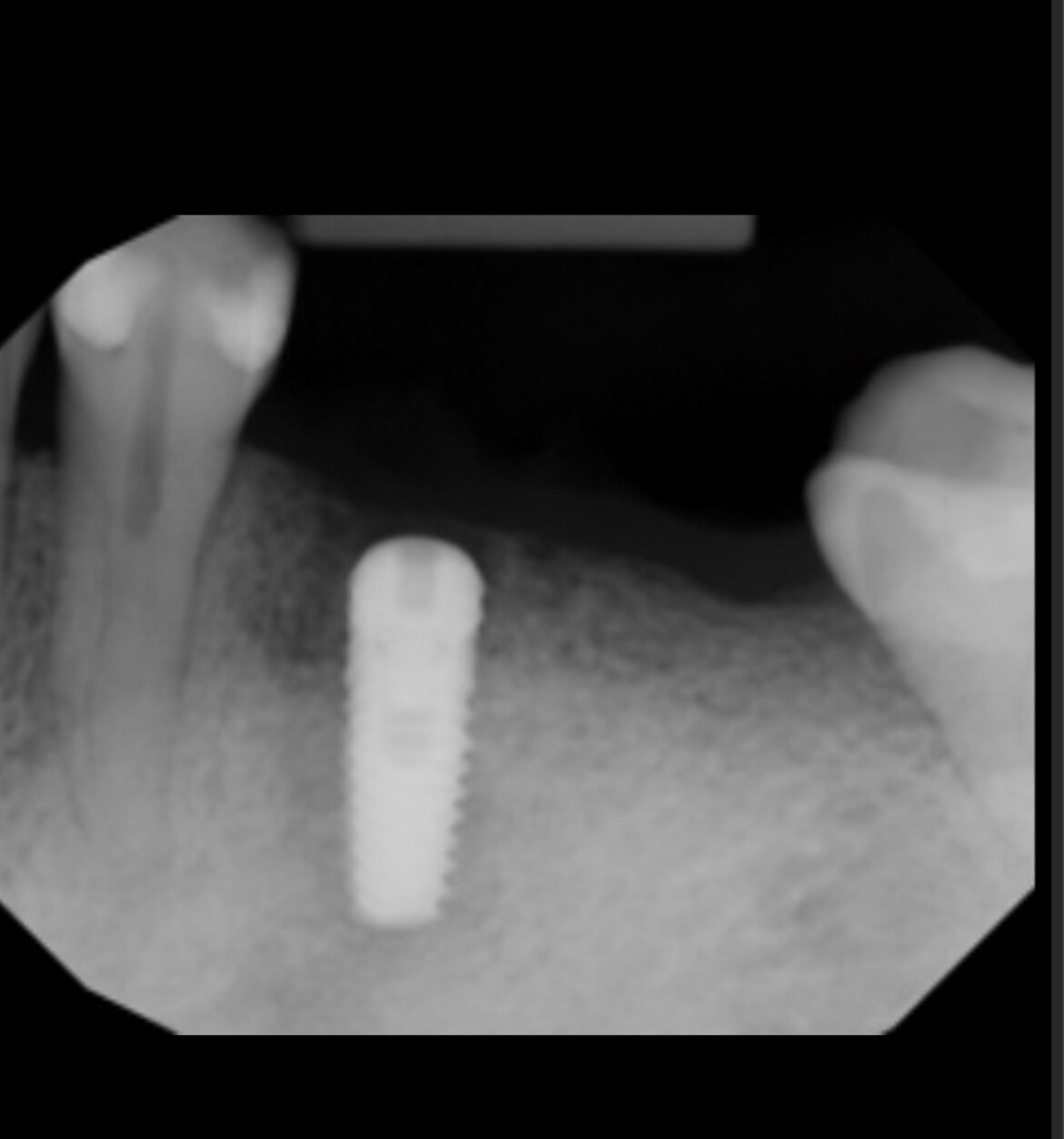
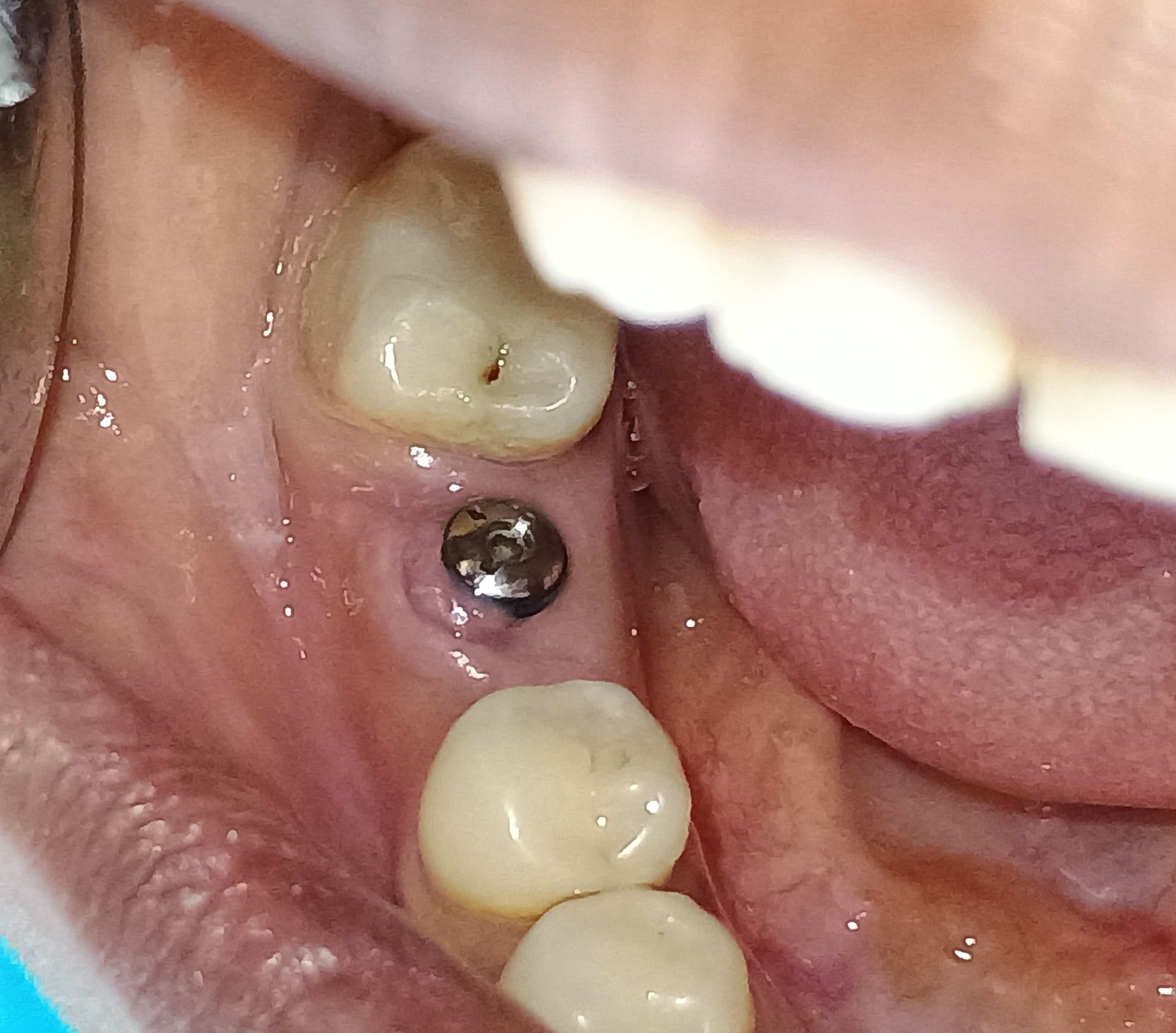
Failing bridge #3,4 to #9,10 retainers, the rest are pontics. #3,4 have internal resorption. Patient is missing first bicuspid(#5). Alveolar ridge vertical and horizontal deficiency. My plan is to place #6,7 guided. Ridge split, Densah bur, protocol for ridge expansion. Veneer graft on buccal. Extract #4 and possibly place immediate, if I can get primary stability which is not likely( no apical height to grab on). Leave #3 for now to hold a temporary bridge in place while #4,6,7 are healing. After three implants integrate extract and cantilever #3 for a final implant supported bridge#4,6,7,8(#3 is cantilever,#8 is cantilever. Compensate for vertical deficiency of the alveolar ridge with pink acrylic. The reason for not replying #3 with implant is to keep a bridge as a temporary and not get him into a flipper and also to shorten treatment time . While there are many ways to augment or compensate for the vertical height deficiency that seems to be a good balance of TX length and predictability. Please provide a critique and some advice on this plan. Thanks.